Gaza medical staff: “We are alive, but we are not OK"
story Apr 26, 2024
Get the latest news, stories, videos, and more from our medical humanitarian projects around the world.
Speaking out about the emergencies our staff and patients witness is part of who we are. Explore our history and principles.
Developing Story
Oct 14, 2023
What to know about the humanitarian catastrophe in Gaza and how MSF teams are addressing the dire needs on the ground.
Read More
Developing Story
Oct 04, 2023
How MSF is responding to urgent needs inside Sudan and in neighboring countries.
Read More
Story | Apr 26, 2024
An MSF-supported free clinic lets people get tested, diagnosed, and treated in one place.
Read More
Story | Apr 26, 2024
The mental health impact of an unyielding war will leave health workers with scars for years to come.
Read More
Story | Apr 25, 2024
A small MSF team has been working alongside other nonprofit groups for the past two weeks to assess the medical needs of asylum seekers and migrants.
Read More
News | Apr 25, 2024
Transparency on clinical trial costs must become the norm to improve access to medical products worldwide.
Read More
Story | Apr 25, 2024
Communities where MSF operates are among the most vulnerable to AMR.
Read More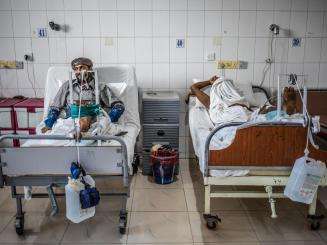
Story | Apr 24, 2024
People in Ikongo district are struggling with malaria coupled with malnutrition, a dual crisis fueled by the climate emergency.
Read More
Story | Apr 23, 2024
People should not be dying of cholera in 2024. We need to act quickly to prevent more deaths.
Read More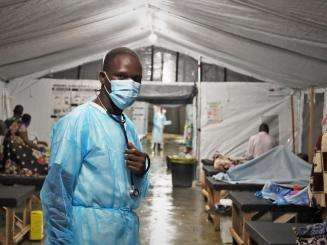
News | Apr 23, 2024
Medical testing shouldn't be a luxury. Danaher and Cepheid must drop the price of GeneXpert for low- and middle-income countries
Read More

Your unrestricted gifts enable us to provide lifesaving medical humanitarian care on the ground and speak out about what we see.