Zahra Koochizad, a midwife supervisor with Doctors Without Borders/Médecins Sans Frontières (MSF), was working in the maternity ward of Kabul’s Dasht-e-Barchi hospital when it was attacked one month ago, on May 12, 2020. Unknown gunmen stormed into the MSF-run maternity ward killing 15 mothers, five of whom were in labor, and two children. MSF midwife Maryam Noorzad was also killed in the attack. The death toll would have been even higher if more than 100 people had not found shelter in the safe rooms of the facility. Zahra writes about the unfathomable losses, and her determination to continue her work.
As midwives in Afghanistan, we bring new life into this country under conditions more difficult than in most. Approximately 130 million babies are born worldwide every year. This also means there are millions of women needing assistance to go through their pregnancy and labor. Giving birth, in my opinion, is one of the most glorious and most critical moments in a woman’s life.
My passion to see new life coming into the world and my strong desire to serve my own people made me choose to become a midwife. Some of my aunts and cousins also work as midwives in different hospitals in Kabul. They also chose this profession because of their desire to serve, and because they learned that, in Afghanistan, most women who die in childbirth died from preventable complications.
Despite some improvements over the past years, Afghanistan has one of the highest maternal and newborn mortality rates in the world. The need for specialized care is vital. In Switzerland, five mothers will die per 100,000 live births; in Afghanistan, 638 mothers will die. This does not include the 15 mothers and five unborn babies who were systematically shot dead in the maternity ward where I work a month ago.
Afghanistan has one of the highest maternal and newborn mortality rates in the world. The need for specialized care is vital.
Zahra Koochizad, MSF midwife supervisor
One of the biggest challenges that every midwife and pregnant woman in Afghanistan faces is insecurity. I’ve painfully experienced this firsthand.
I am the midwife supervisor in the MSF-run maternity wing of Dasht-e-Barchi hospital in Kabul. The attack there occurred on May 12. I remember that day: we had very nice weather, the air was fresh, and I felt a sense of peace when entering the hospital. Once I arrived, I saw my colleagues working; they all looked motivated and eager to start a new day of providing services to pregnant women in need. On a daily basis, we are used to tragedy in our communities but nothing could have prepared us for the horror to come.
In Afghanistan, a maternity ward is one of the few spaces where women are the leaders. The terrorists entered an area where no men are ever allowed to go. They stormed the maternity wing armed with guns, killing pregnant women, new mothers, and newborns. Their leader must be very proud—celebrating victory over an army of one-day-old babies and women wearing only their hospital robes.
A hospital is supposed to be a protected space. It says this under international humanitarian law. And yet the assault on my maternity wing is not an exceptional case—attacks on health care happen frequently here. What is different about this attack than all the others?

As midwives in Afghanistan, we are the silent leaders of our country. We are at the bedside of pregnant women giving birth to the country’s future—and we need to be protected. To safeguard a maternity wing like mine is to safeguard our future, along with the midwives working there. Midwives like our beloved Maryam, who was killed in the most incomprehensible way as she assisted soon-to-be mothers giving birth.
As midwives in Afghanistan, we are the silent leaders of our country. We are at the bedside of pregnant women giving birth to the country’s future—and we need to be protected.
Zahra Koochizad, MSF midwife supervisor
On the day of the four-hour assault on Dasht-e-Barchi maternity wing, the terrorists not only attacked pregnant women and newborns, but also the decades of work to reduce maternal and newborn mortality in Afghanistan. Because of this attack, the western area of Kabul, with more than one million residents, and women coming from faraway provinces, no longer have access to any comprehensive obstetric and newborn care.
Their only option now is a 50-bed hospital close by, but with only seven beds devoted to maternity services. I do not know if the pregnant women who go there, or to other hospitals, are being cared for as they need. Will they receive the help they need? Will they have the means to pay for hospital services? Will they survive their labor if they are not admitted to any hospital?
I am scared to think about what will happen to those women who would have otherwise come to us.
Each month, the MSF-run maternity wing provided quality services to more than 1,200 mothers who delivered their babies there. I know that if the women in the Dasht-e-Barchi area need childbirth assistance, they would go to the 50-bed hospital; but if they have any complications, they will not be admitted there. There is no operating theater for emergency cases, for example. And with the COVID-19 pandemic, the options for women who have complications or special needs are even fewer, and farther away, than before.
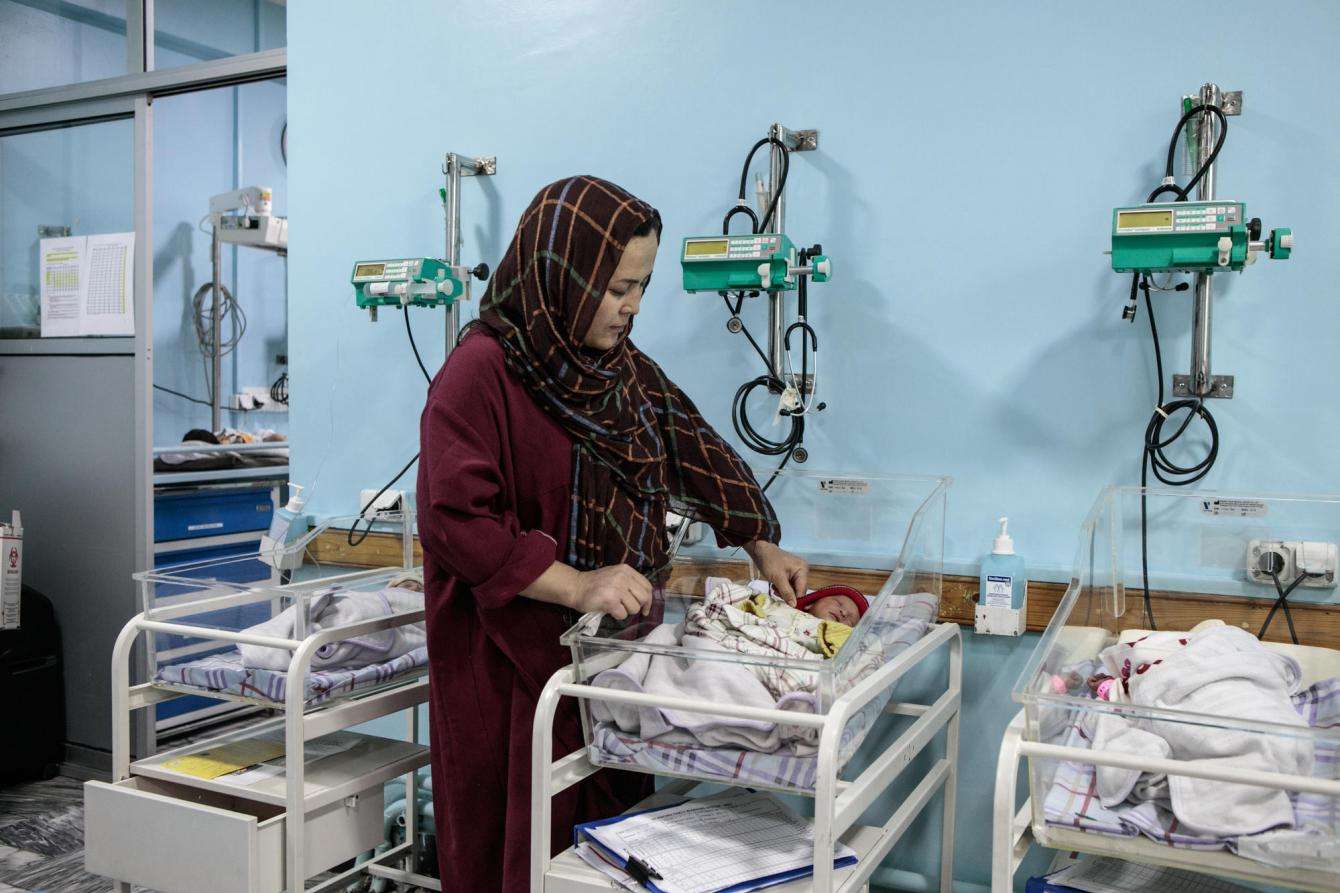
Most patients who came to Dasht-e-Barchi belong to the Hazara community, a historically marginalized and still poor ethnic minority. They don’t have the means to pay for their treatment in other places. Some of the women arrived at the hospital in terrible condition.
I can recall one patient in particular. She came to us for the first time, but she could hardly walk and looked very pale. She came from an area on the outskirts of Kabul. I examined her and realized she had severe anemia. There was no antenatal care available where she lived. Due to the lack of means to buy food, she was not eating properly. When I asked her when she had last eaten, her answer was “yesterday.” My heart broke when upon hearing that, but I was so happy to see her recover and give birth to a healthy baby.
Her story is just one of the thousands that describes the reality of life for patients in the Dasht-e-Barchi area. Some of them would come to the hospital and not have money to get back home.
All of our patients and the wider community were very happy to count on our maternity wing that provided services for free, especially since government hospitals charge some amount of money. I am saddened to see how poverty, the lack of a good health system, lack of resources, insecurity, and the COVID-19 pandemic are all limiting possibilities for people to receive proper health care. Health care centers in Kabul are already operating at reduced capacity because some of their staff are infected with COVID-19.
I am hurt, my life has changed, but I am still committed to continue my work. I know my people need us and expect me to get back on my feet again with the support of MSF. I cannot forget all those patients who need a helping hand and a good level of care. I also want to honor all of those patients who have become our friends and have been praying for me. I do not want to disappoint them, especially now, when many are also suffering from the COVID-19 pandemic.
I see our people suffering from greater obstacles, in a situation which is already critical—and the need for health care services has never been greater.