The current Ebola outbreak in Democratic Republic of Congo (DRC) is the worst on record in the country and the second-largest epidemic of the disease recorded anywhere. More than a year after the declaration of this Ebola outbreak in August 2018, it is clear that crisis in DRC are still not under control—despite having new tools like an investigational vaccine and developmental treatments. Nearly 2,000 people have died from the virus, and patients have been identified in new geographical areas in the last few weeks, including in South Kivu—the third province affected by this outbreak.
On July 17, the World Health Organization declared the Ebola outbreak in DRC to be a public health emergency of international concern. Doctors Without Borders/Médecins Sans Frontières (MSF) hopes that greater international attention will improve the response to the epidemic and lead to a revised strategy that is more patient-focused and community-centered.
MSF is providing care—in collaboration with the Ministry of Health—for confirmed Ebola patients in Goma, North Kivu province, Bunia, Ituri province, and Bukavu, South Kivu province.
MSF has repeatedly stressed that the spread of this deadly virus cannot be stopped without building greater trust between those involved in the Ebola response and the local communities directly affected. All actors involved in the response need to review what must be done to bring the Ebola outbreak to an end while constructively engaging with community. We also believe the Ebola response should be integrated into local health care facilities so that medical services are easier for people to access.
Ebola situation report as of August 26, 2019
|
Total cases: 2,983 Total deaths: 1,994 |
*Data reported by the DRC Ministry of Health and published by the World Health Organization. "Probable" deaths refer to deaths that were linked to confirmed Ebola cases but not tested before burial.
This is the tenth outbreak of Ebola in DRC in 40 years and by far the country's largest ever documented. It is also the second largest Ebola epidemic on record anywhere, behind the West Africa outbreak of 2014–2016.
DRC’s Ministry of Health officially declared the latest outbreak of Ebola virus disease in North Kivu on August 1, 2018, but the outbreak likely began months earlier. In the first eight months (from August 2018 to March 2019) more than 1,000 confirmed and probable cases were reported in the affected region. However, from April to June 2019, that number doubled, with an additional 1,000 new cases of Ebola reported in this short period alone. During the past few weeks, the number of new cases reported per week slightly decreased, averaging 72 people per week, but the number of affected areas has increased.
Ebola response
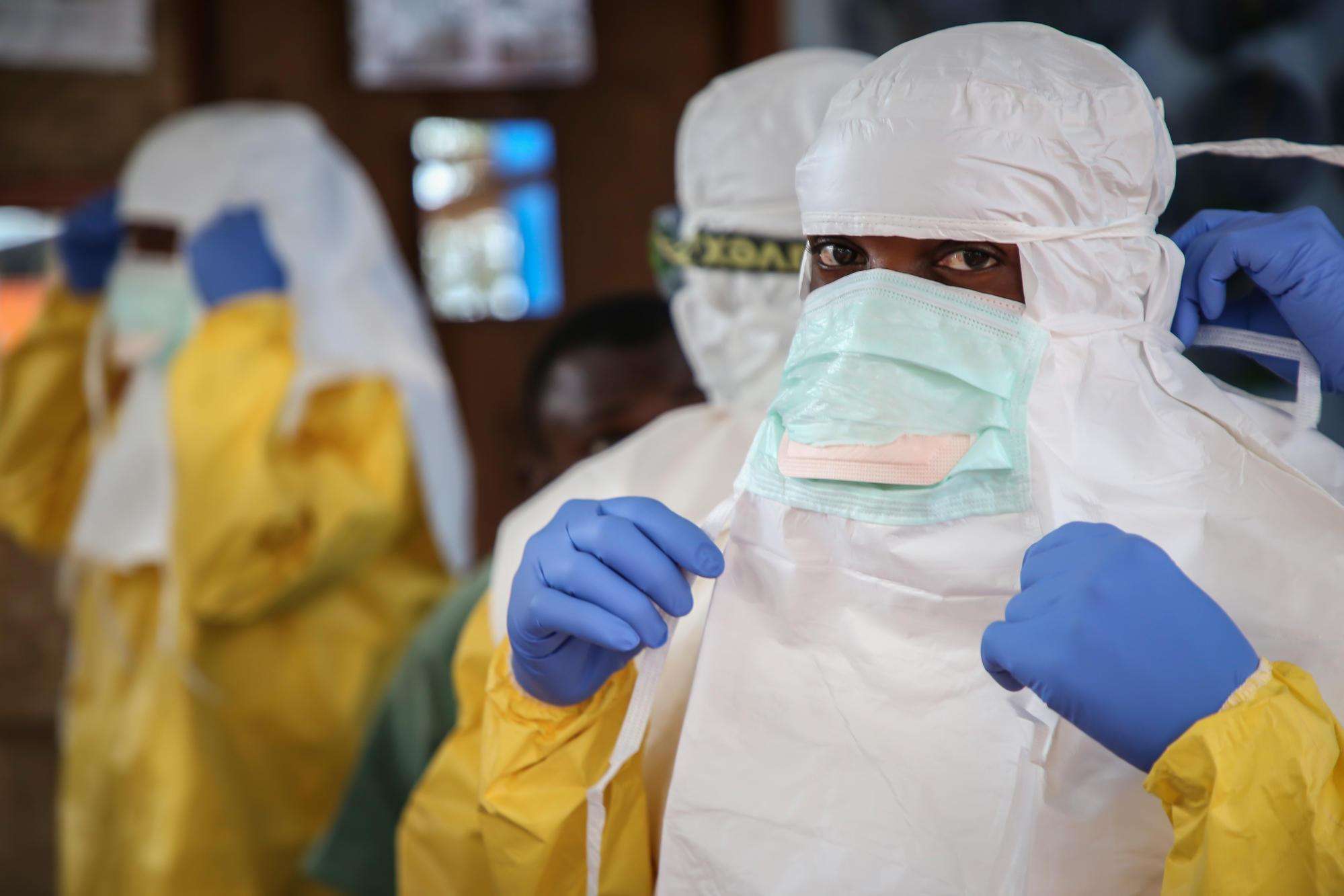
MSF currently has 10 Ebola projects and is providing care for confirmed Ebola patients in the three affected provinces, including an Ebola treatment center (ETC) we are currently managing in Bunia, Ituri province, in collaboration with the Ministry of Health and a new 50-bed ETC in Nyiragongo health zone of Goma, North Kivu province. MSF is also currently constructing an ETC in the Mwenga area of South Kivu. Earlier this year, we withdrew from our ETCs in the North Kivu cities of Butembo and Katwa following separate attacks on the facilities.
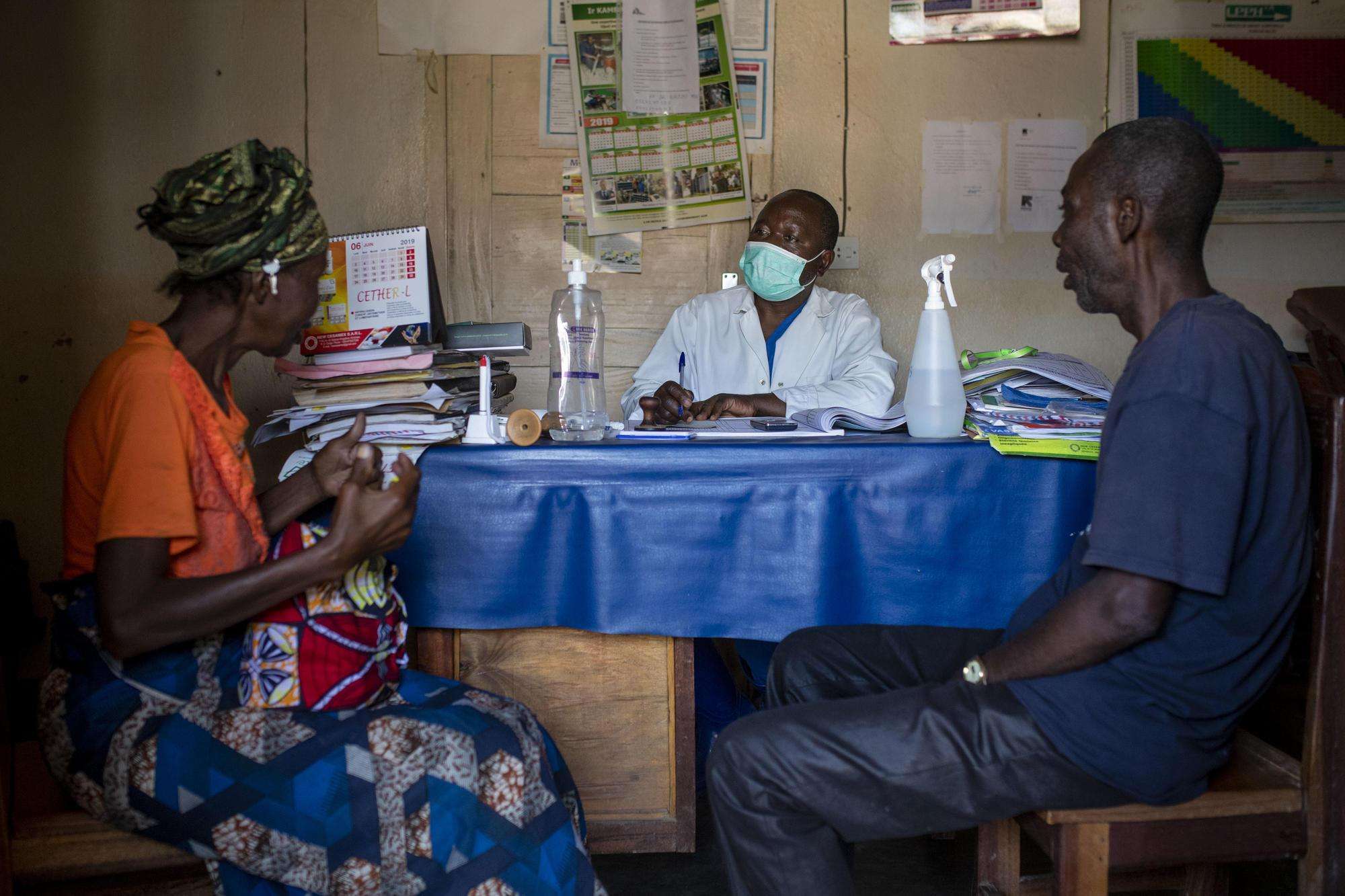
We are also helping existing health care facilities in the affected provinces prepare for and receive people who may have Ebola, managing transit centers where patients with suspected Ebola are tested and sent to ETCs if they test positive, and working to implement and strengthen disease surveillance and infection prevention and control activities in the region. For example, MSF has been present in Goma for Ebola preparedness for more than eight months now, reinforcing the disease surveillance system and ensuring there is adequate capacity to manage those who might—or have been confirmed to—have Ebola.
As Ebola is only one public health crisis among several others affecting people living in this region of DRC, our main priority is to give timely and appropriate medical care to patients, regardless of their illness. To do so, we’re working closely with the affected communities to identify their needs and ensure that access to essential health care services is guaranteed for patients suffering from all major diseases affecting people in the area, such as the massive ongoing measles outbreak, malaria, and diarrheal diseases. That’s why MSF teams are also present in local health structures, where we offer general health care services and work to increase access to health care for all patients.
As of August 2019, MSF has more than 615 staff deployed in DRC for the Ebola emergency.
Integrating care
MSF aims to integrate its Ebola response activities into the existing health care system to ensure such services are close to those who need them.
Integrating the Ebola response in the health care facilities is key to bringing the epidemic to an end since many people experiencing symptoms of Ebola continue to seek health care at facilities that they are already familiar with rather than going directly to an ETC. Working more closely with local health centers also helps identify people with Ebola earlier, which helps to ensure that they receive proper care (giving them a better chance of survival) and also prevents the spread of the infectious disease.
The results of integrating care are encouraging; in July, 10 percent of the confirmed patients admitted to an ETC in Beni had been referred there from a health center supported by MSF. That is a higher percentage than that of patients referred from dedicated Ebola transit centers.
Vaccination strategy
As part of a larger consortium, MSF and Epicentre—our research arm—are active contributors to discussions around the vaccination strategy, including the possible introduction of a second investigational vaccine. MSF has also expressed its willingness to participate in the implementation of a revised vaccination strategy for the currently deployed rVSV-ZEBOV vaccine—the Ebola vaccine currently being used in DRC.
We consider that the ring vaccination strategy implemented so far is not enough to contain the epidemic. The current strategy involves vaccinating anyone who’s been in contact with someone infected with Ebola, as well as their contacts. This approach relies heavily on the identification and follow-up of contacts in a context where doing so is very challenging and the affected communities are often moving around. In order to have any impact on controlling the epidemic, at least 100-150 identified contacts and contacts of contacts need to be urgently vaccinated around each person confirmed to have Ebola, and this has never been achieved during this outbreak so far.
We agree with the experts’ recommendations of adopting a vaccination strategy that is based on geographic targeting and facilitating access to vaccination for more people, including all people who are at risk of contracting the virus. We have to consider increasing the number of people receiving vaccination against Ebola in the current epidemic as an alternative strategy if we want this potentially game-changing tool to demonstrate real impact.
The number of doses of rVSV-ZEBOV available in DRC should be increased. Full transparency should be ensured with respect to the status of the global stock of the rVSV-ZEBOV vaccine, which is made by pharmaceutical corporation Merck.
Given the concerns about the current number of rVSV-ZEBOV vaccines available, and the need to expand options in this and future epidemics, the authorities in DRC are now reconsidering the decision to refuse the trial of a second investigational Ebola vaccine in DRC during this epidemic.
Local context
The epicenter of the outbreak remains in North Kivu province, a densely populated area in northeastern DRC with approximately seven million people. Despite the challenges of rough terrain and poor roads, people in this region are highly mobile. North Kivu shares a border with Uganda to the east and sees a lot of trade, as well as human trafficking and “irregular” crossings. Some communities live on both sides of the border and cross back and forth frequently to visit relatives or trade goods.
North Kivu has been an area of conflict for more than 25 years, with more than 100 armed groups estimated to be active. Criminal activity, such as kidnapping, is relatively common, and skirmishes between armed groups occur regularly. Widespread violence has uprooted people and made some areas in the region quite difficult to access.
Since the start of the outbreak, 28 health zones out of a total 47 in the provinces of North Kivu and Ituri have been affected by Ebola. In August, Ebola was reported in Mwenga health zone, South Kivu province, increasing the total number of affected provinces to three. Currently, 18 health zones are considered as active transmission zones, meaning that they have reported newly diagnosed people in the last 21 days. Five new health zones—Goma, Nyiragongo, and Pinga, North Kivu province; Lolwa, Ituri province; and Mwenga, South Kivu province—were recently added to the list.
Since mid-June, Beni, North Kivu province, has reported the highest number of Ebola cases, followed by Mandima health zone, Ituri province. Former hotspots such as Butembo, Katwa, and Kalunguta health zones are also reporting more cases in the recent weeks.
There have been three people with confirmed cases of Ebola in Goma—the capital of North Kivu and a city of two million people located on the Rwandan border. Following the first confirmed case identified in Goma, the World Health Organization on July 17 declared the Ebola outbreak in DRC to be a public health emergency of international concern.
On June 11, Uganda announced that three people from a single family had been diagnosed with Ebola, the first cross-border cases since the outbreak began. Uganda has not recorded any further cases.
Community Engagement
All actors involved in the Ebola response, including MSF, have failed to build trust within the local community. Widespread mistrust, as well as violent attacks against the Ebola response, are hampering efforts to control the epidemic. People are not seeking care in ETCs, resulting in an increased likelihood that the virus could spread in other health facilities that aren’t equipped with proper infection control procedures and equipment.
Security conditions have also made responding to this outbreak challenging. Targeted violence against those working on the Ebola response has disrupted crucial activities like vaccination, contact tracing, community health promotion, and safe burials, in addition to discouraging people from coming to ETCs for testing when they fall ill and present Ebola-like symptoms. Such violence is partly linked to the specific issues of deploying a massive responsive in an area of long-term conflict and political tensions. But the attacks also reflect, once again, the Ebola response’s failure to engage with the affected communities and the lack of understanding and consideration of the needs highlighted by local people.
In order to stop the outbreak, we have to constructively engage with local communities in the design and implementation of the response.
Epidemiological concerns
MSF is extremely concerned about the lack of visibility on the actual epidemiological situation. Many people have died of Ebola in their communities before they could be identified, diagnosed, and admitted for treatment of the disease. Roughly a third of Ebola-related deaths have been diagnosed only post-mortem, which is a clear indication the response to the epidemic is failing in identifying and tracing people who’ve potentially contracted Ebola.
Since the beginning of the epidemic, the delay between the onset of the symptoms and admission has remained unchanged at around five days; the longer an Ebola patient stays in the community without proper isolation and care, the lower the chances of survival and the higher the risk that they will pass the virus to others. The high number of Ebola deaths within the community (reported between 19 percent to 32 percent of all fatalities) has increased during the past weeks, a strong indicator that the outbreak is still not under control.
In the past few months, only around half of the new reported Ebola cases have been identified as contacts of previous confirmed cases before falling ill and seeking treatment, or dying without receiving proper Ebola care. These figures highlight the many challenges related to the identification and close follow-up with contacts of people infected with Ebola (both confirmed and probable cases), which would allow people who have the disease to receive adequate and timely care and reduce the risk of transmission by facilitating the vaccination of those contacts. The facts that many contacts are lost and many cases go undetected indicate that the Ebola response is still struggling to work with the affected communities, understand their needs and concerns, and gain their trust.