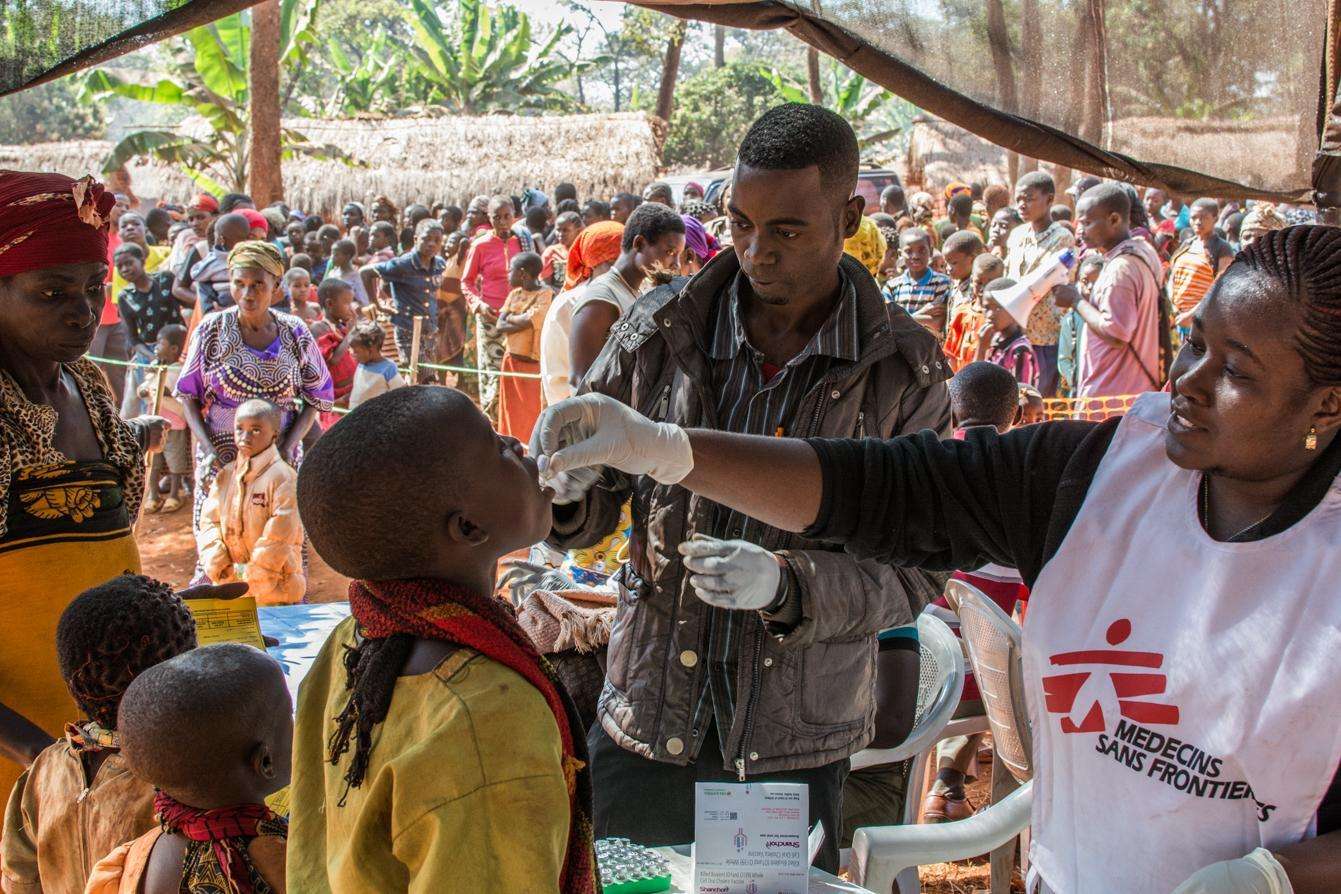
“I think people in Western countries generally tend to forget about the importance of vaccination because we’re all vaccinated [against most common diseases],” said John Johnson, Doctors Without Borders/Médecins Sans Frontières (MSF) medical vaccination referent for epidemic response. “So people don’t see what happens when you’re not.”
MSF teams see firsthand what happens to communities when vaccines are out of reach—from measles epidemics in remote regions of Democratic Republic of Congo (DRC), to cholera outbreaks in war-torn Yemen, to a rare outbreak of diphtheria in refugee camps for Rohingya people in Bangladesh. In places with fragile or collapsed health systems, people often miss out on routine vaccinations that protect against certain diseases. This is especially true during humanitarian emergencies—including conflicts and natural and human-made disasters.
With decades of experience in outbreak response, we have learned some important lessons about how to use vaccines alongside other tools to effectively end an epidemic. We often have to adapt and innovate to meet the evolving needs.

Recognizing the needs
When an Ebola outbreak hit northeastern DRC in 2018, many people living in affected areas wondered why health workers from around the world rushed in to respond. They were facing many other imminent threats, including diarrheal diseases, malaria, and pneumonia. A major measles epidemic swept the country in the shadow of Ebola, ultimately killing more than 7,000 children— triple the official death toll of the headline disease.
“There were hundreds of thousands of cases of measles, and tens of thousands of deaths in DRC and neighboring countries between 2019 and 2020,” Johnson said. “At the same time, there's a massive international response mobilized for an Ebola outbreak in DRC, where there were about 3,500 cases and nearly 2,300 deaths. Which is important, and it’s terrible—but what you see is this stark contrast. Measles is preventable, and yet there was so much less attention paid to that huge outbreak because everyone was focused on Ebola, and then, of course, on COVID.”

Throughout the measles epidemic MSF deployed emergency teams in 22 of DRC’s 26 provinces, vaccinating more than 2.3 million children. We also provided medical care for children sickened by the disease, and advocated for a stronger response from national and international actors.
During high-profile emergencies like Ebola and COVID-19, activities like routine vaccinations for measles are often put on hold, which can lead to a resurgence of preventable diseases, as in DRC, where cases of measles are once again on the rise despite health authorities declaring an end to the epidemic in August 2020. Additionally, moving staff and medical equipment to “new” emergencies can lead to gaps in care for those who fall ill from other diseases that are even more prevalent. “A one-track focus on COVID-19 will sow the seeds of other major health crises,” warned Emmanuel Lampaert, MSF operations coordinator in DRC.
That’s why it’s critical for the international aid sector to understand and address the real health needs of a community.

Earning the community’s trust
Alongside the measles response, MSF was still working to bring an end to DRC’s Ebola epidemic in North Kivu, with the country’s tenth and largest-ever outbreak finally declared over in June 2020. (This year we supported the national response to the country’s twelfth Ebola outbreak, also centered in North Kivu.) However, we learned some crucial lessons over the course of this intervention—including that having a safe and effective vaccine is not enough. “The most important thing is to engage communities,” said Dr. Nicolas Peyraud, MSF vaccination advisor. “Vaccination campaigns cannot be effective if they don’t reach people.”

Many people here were understandably skeptical about getting the newly available vaccine—which went from being evaluated in a clinical trial and then more widely used over the course of the outbreak. Some people didn’t even believe Ebola existed. And, regardless, it wasn’t their main concern. This was a conflict-affected area that had been largely neglected for years. How could we expect people to want a vaccine for a disease many had never heard of while the global health community ignored their other needs?
The key to ending this outbreak was informing and engaging with the community, reducing the stigma associated with Ebola, providing care closer to where people lived, and adapting aid to what people identified as their most urgent health needs. Once they felt more involved in the Ebola response, they were more likely to trust the vaccine
During DRC’s eleventh outbreak, centered in Équateur province, MSF supported community-based outreach and care that complemented vaccination efforts led by other partners. This time, the outbreak was brought under control within five months. Having a licensed Ebola vaccine was critical, but only as part of a more comprehensive approach.
Reaching more people
Since first responding to cholera epidemics in sub-Saharan Africa in the 1980s, MSF has been one of the lead organizations working to prevent and treat the disease. Cholera outbreaks happen in many of the settings where we operate, including remote villages, overcrowded cities, refugee camps, and conflict zones. These are all places where clean water and proper sanitation services can be extremely limited.

But carrying out vaccination campaigns can only work if there are enough vaccines to reach everyone in need, which is often not the case. When a major cholera outbreak struck Lusaka, Zambia, in February 2016, the World Health Organization’s (WHO) emergency stockpile of cholera vaccines did not have enough to cover approximately 1.2 million people living in crowded, high-risk urban settlements.
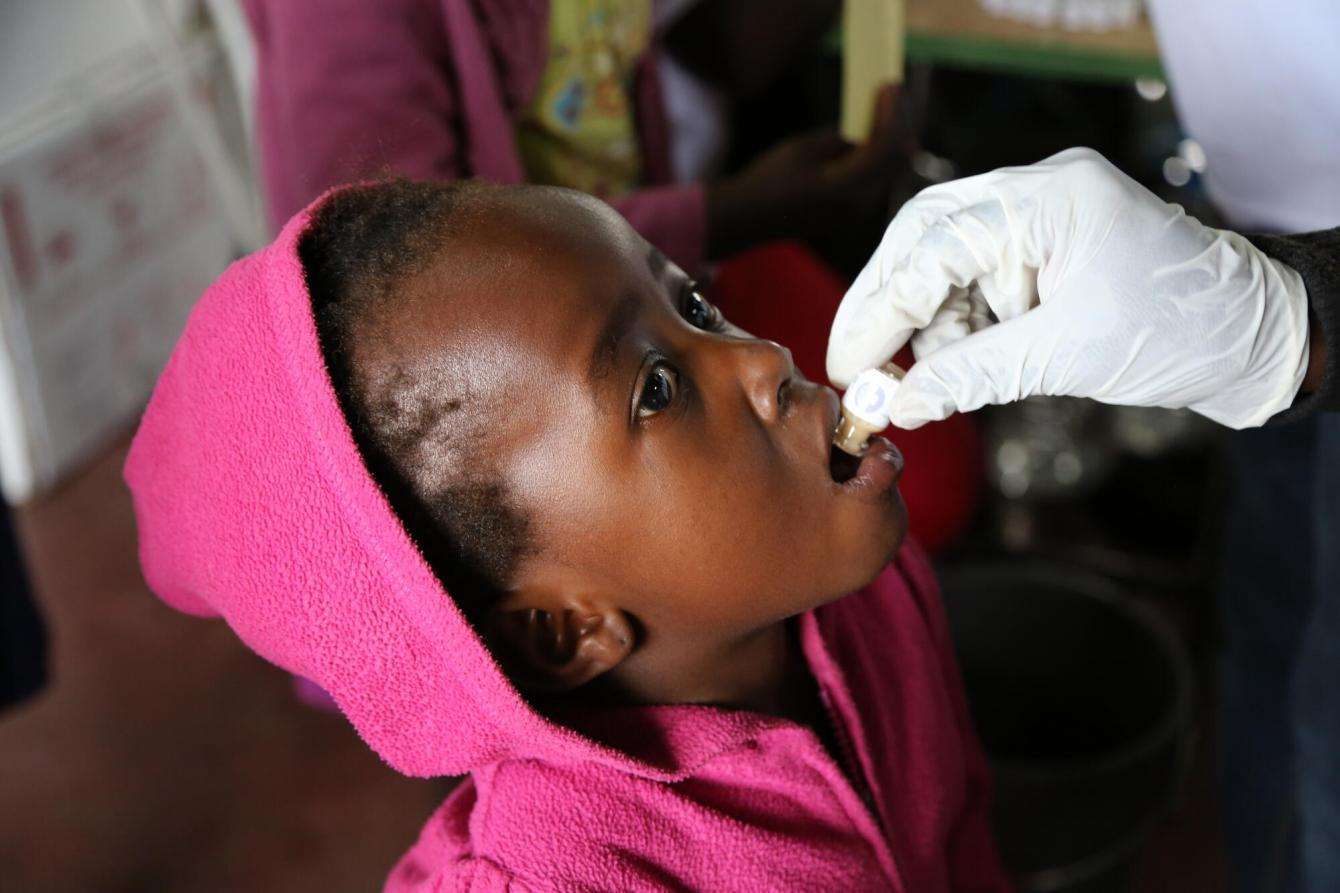
Though cholera immunization typically requires two vaccine doses, previous studies—including one conducted by MSF—showed that just one could be useful in curbing outbreaks of the disease. MSF’s use of this strategy in Zambia during this emergency was nearly 90 percent effective and helped protect more people while bringing the outbreak under control.
Another way MSF teams have vaccinated more people against cholera is by administering the first of two oral vaccine doses and then giving the patient the second dose to take home. We provided instructions to keep the dose in a cool place, such as a clay pot, for later use. This proved quite successful in 2016, during an outbreak in hard-to-reach fishing towns and floating islands around Lake Chilwa, Malawi, where MSF teams had to deliver the vaccines by boat to people living in unmapped and nearly unreachable villages with limited access to health care.
Making a global impact
While responding to epidemics with vaccines has helped MSF save countless lives, vaccinating the person in front of us isn't always enough. Our response to outbreaks and related research can also have much wider global impacts.

Earlier this year, a study conducted by MSF’s research institute, Epicentre, in Uganda and Kenya showed that giving people one-fifth of the standard yellow fever vaccine dose is safe and effective. This fractional dosing could help stretch scarce supplies, making it possible to vaccinate millions more people during outbreaks in times of vaccine shortage. The WHO will now change its guidelines to recommend that all vaccinators use partial doses of the yellow fever vaccine during emergencies. There is no cure for yellow fever, so prevention is extremely important.
“Vaccination is important in halting the spread of outbreaks,” said Juliet Mwanga, director of Epicentre's research center in Mbarara, Uganda. “Sometimes the disease in question does not have a treatment yet, and vaccination may be the only tool available to stop the outbreak. Even if treatments may already be available, vaccination prevents more people from catching the disease and reduces the load on the health systems and people’s suffering.”