Alert is a quarterly magazine published by Doctors Without Borders/Médecins Sans Frontières (MSF-USA) that features compelling stories and photography from our work in the field. Below is an excerpt from MSF-USA Board President Africa Stewart's introduction to the Fall 2019 issue (Vol 20. No. 3.), Fighting Superbugs: The Global Threat of Antimicrobial Resistance
Dear Friends,
For nearly fifty years, Doctors Without Borders/Médecins Sans Frontières (MSF) has been responding to the most urgent humanitarian crises around the world. From our organization's founding in the wake of war and famine in Biafra to our response to the catastrophic 2010 earthquake in Haiti to the massive mobilization to fight the Ebola epidemic in West Africa, we've always adapted our responses to meet the unique needs of our patients.
We’re now facing a very different kind of emergency, one that is far less visible and much more insidious. At MSF projects around the world, we see growing antimicrobial resistance—which means that many of the drugs we’ve relied on for decades to treat our patients are simply not working.
Antimicrobial drugs, and antibiotics in particular, are invaluable tools to stop life-threatening infections, curb outbreaks, and save lives. So what will we do without them? What are the alternatives?
I first encountered antibiotic resistance as a young intern in Philadelphia, while I was training in a free clinic for women. We learned to follow the antibiotic updates year after year as chlamydia and gonorrhea were becoming increasingly difficult to treat. When I began working with MSF and my practice expanded to include patients around the world, I came to understand how urgent the threat of antimicrobial resistance, or AMR, truly is.
The World Health Organization has declared that “antibiotic resistance is one of the biggest threats to global health, food security, and development,” yet international efforts to combat it tend to focus on wealthy countries.
AMR is a particularly pressing problem in countries with weak or failing health systems, poor sanitation, and especially in regions at war. If these criteria sound familiar to you, it’s for good reason: nearly all of the places where MSF works fall into one or more of these categories. Around the world, our teams are encountering drug-resistant bacteria, often at worryingly high rates.
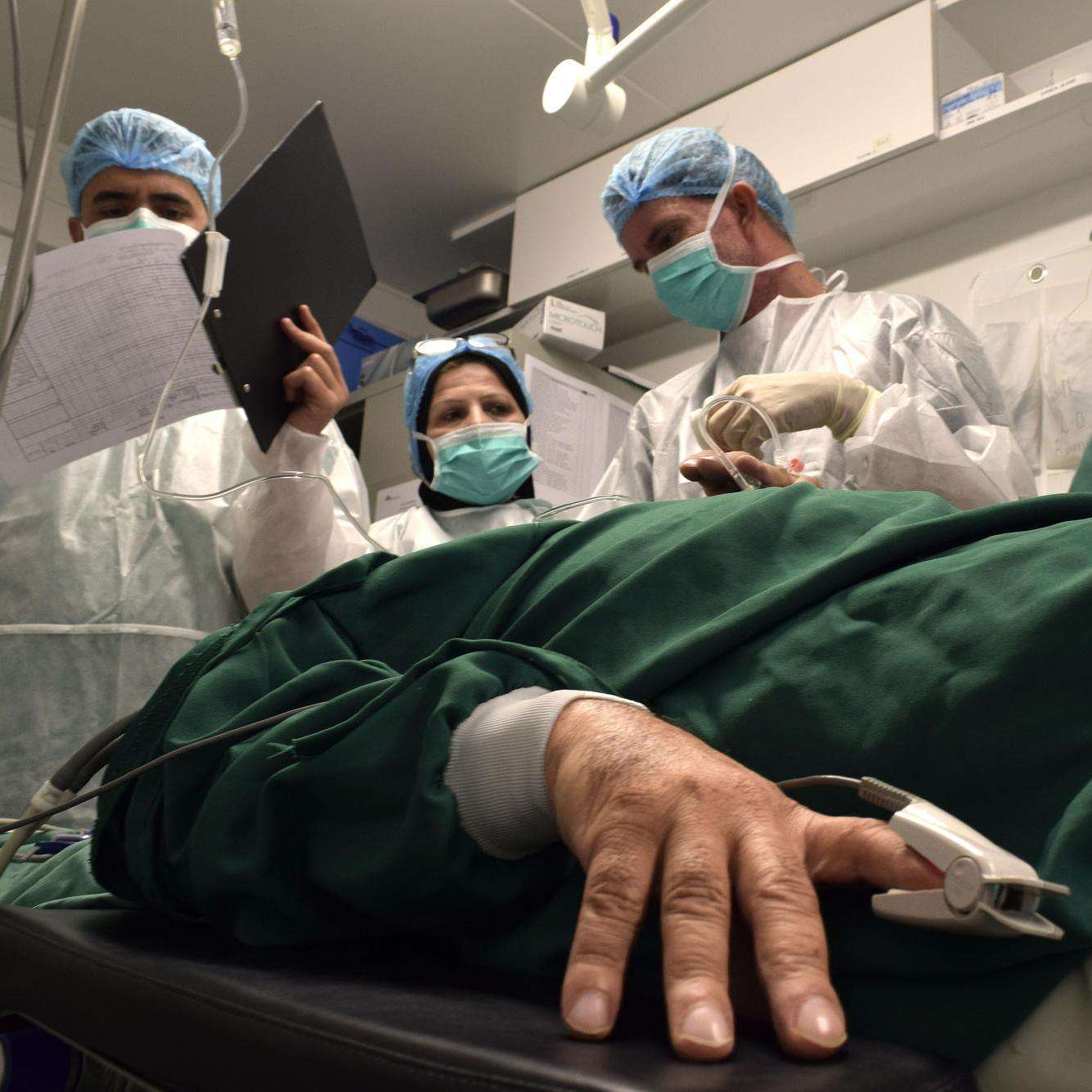
In our reconstructive surgery program in Amman, Jordan, for example, up to 60 percent of the infections our doctors and nurses treat in war-wounded patients from across the Middle East are resistant to antibiotics.
In Gaza, more than a thousand Palestinians are now suffering from chronic bone infections—many of them resistant to antibiotics—after being shot by the Israeli army during demonstrations that began in 2018. And in Port-au-Prince, Haiti, where MSF runs the only specialized center in the country for the treatment of severe burns, patients are particularly vulnerable to antibiotic-resistant infections that can further complicate already difficult recoveries.
To face this threat, we are doing what we always do when confronted with a new challenge: we adapt and we innovate. In these pages you’ll learn about the many ways our teams are working to fight antimicrobial resistance in our projects from the forests of Cambodia to the fields of southern Mali. We’re also sharing research and expertise with partners and national ministries of health. A challenge as complex as AMR requires a broad slate of strategies tailored to unique contexts and needs, from the implementation of cutting-edge technology to decidedly low-tech, community-based solutions.
None of these efforts would be possible without your support. Donors like you ensure that MSF is able to find ways to provide our patients with the highest quality care possible, no matter the emergency. We will continue to look for opportunities to improve our medical operations and help preserve lifesaving antibiotics for future generations. Thanks, as always, for all that you do.
Sincerely,
Africa Stewart, MD
President, MSF-USA Board of Directors