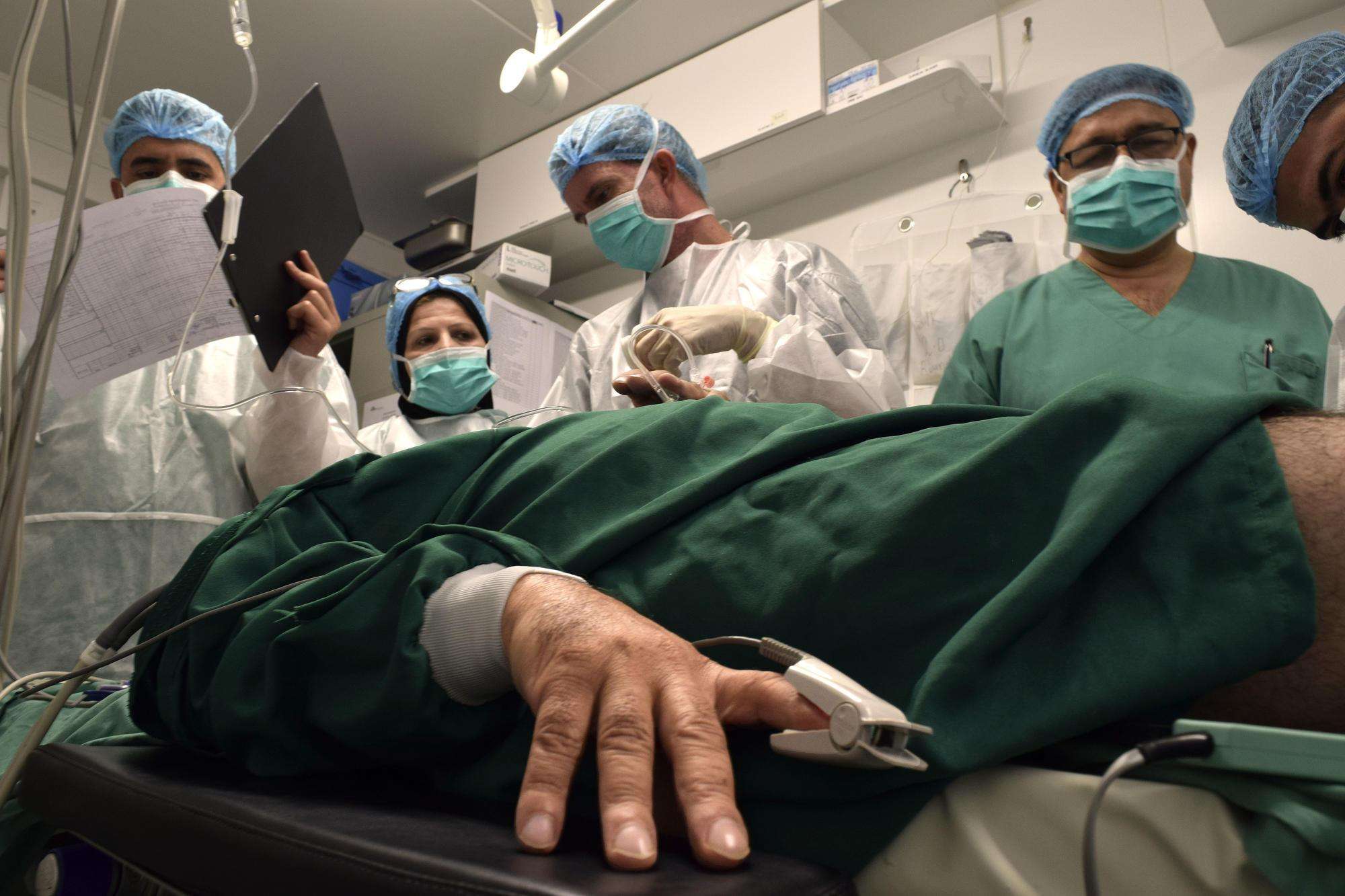
The day Saad’s life changed forever started like any other. The 46-year-old man was beginning his day in Mosul, Iraq, where his family has lived for generations. “It was an incredibly hot, overcast morning, like lots of days,” he remembers. But as he walked to his car to go to work, a sudden explosion shattered the morning calm.
A bomb had gone off in the neighborhood. The blast was not close enough to kill Saad, but it mangled his leg, fracturing his tibia and fibula. Unconscious, he was rushed to a hospital for surgery. “The first surgery I had consisted of inserting an internal fixation into my leg to enable me to walk again,” he said. This surgical method of stabilizing broken bones should have put Saad on the road to healing, but he suffered complications. “The recovery was excruciating,” he said.
When Doctors Without Borders/Médecins Sans Frontières (MSF) opened a post-operative care facility in eastern Mosul in April 2018 for people recovering from traumatic injuries, Saad was admitted. A biopsy showed that his internal fixation needed to be removed and replaced by an external one—and that he had developed a multidrug-resistant infection.
A major public health challenge
Saad’s case is not uncommon. Almost 40 percent of patients admitted to MSF’s post-operative care facility in East Mosul arrive with multidrug-resistant infections, and antibiotic resistance is a problem throughout the country. While antibiotic resistance occurs in many countries where MSF works, its incidence is particularly high in Iraq and across the Middle East.
“Antibiotic resistance has not always been a major problem in Iraq,” said Karam Yaseen, who worked as a health promoter at the hospital where Saad was treated.
“Fifteen years ago, the use of antibiotics was fairly well-regulated, and we had a good medical system.”
But the start of the Iraq War in 2003 changed everything. With the country’s health system shattered by the conflict and people becoming increasingly desperate to find care, some antibiotics that previously required a prescription became easily accessible in markets. People started to use them more and more, whenever they were sick. Over time, those drugs became less effective.
“Now, in Iraq, a pharmacist can sell you antibiotics, even the injectable ones, without a prescription,” said Yaseen. “The availability of these drugs is directly linked to the patterns of resistance that we see today in bacteria.”
In the long run, antibiotic resistance has a tremendous impact on people’s health. If antibiotics lose their effectiveness, essential medical procedures can become too risky to carry out. Antibiotic resistance also complicates the recovery of patients suffering from traumatic injuries—like those MSF treats in eastern Mosul.
Fighting resistance
When our post-operative care facility opened last year, MSF implemented antibiotic stewardship and infection prevention and control measures to limit the impact of drug-resistant infections.
“It’s crucial to avoid the transmission of multidrug-resistant infections between patients in the facility,” said An Caluwaerts, MSF’s advisor on infection prevention and control. These measures can be as simple as making sure that people wash their hands properly, one of the most important ways to prevent transmission. “Undertaken at the right time, hand hygiene can prevent the spread of resistant or sensitive organisms present in our environment and in our body,” said Caluwaerts.
“Contact precautions” are also fundamental: patients with multidrug-resistant infections are given single rooms in the facility, rather than staying in open-plan wards, to avoid the spread of infection to other patients and medical staff. Contact precautions also include the use of personal protective equipment, such as gloves and gowns; limiting the transport and movement of patients; using dedicated patient-care equipment; and making sure that patients’ rooms are thoroughly cleaned and disinfected regularly.
Mental health care and health promotion are essential
Because of their physical isolation within the hospital, patients with drug-resistant infections are more likely to experience psychological difficulties related to what they have experienced in the past as well as the challenges of their treatment.
“People who are in ‘contact isolation’ experience higher levels of anxiety, depression, and anger than other patients,” said Olivera Novakovic, a psychologist in MSF’s East Mosul project. “Many of our patients experienced traumatic events, and they have more time to think about it when they are in isolation rooms.”
MSF mental health staff are on hand to help them cope. “We’re developing individual psychological programs according to the age and the level of education of our patients,” said Novakovic. “Psycho-education is a crucial phase, because if the patient understands why he’s in contact isolation and what drug resistance is, naturally he will become more compliant with the treatment.”
At the same time, MSF’s health promoters raise awareness about multidrug-resistant infections among patients and caretakers. “Antibiotic resistance represents a severe threat to public health and it shouldn’t be underestimated,” said Yaseen, whose team conducts “awareness sessions” inside the hospital for caretakers who will be looking after relatives suffering from resistant infections.
Usually, caretakers who attend these sessions are eager to find out more about antibiotic resistance. Many are surprised by what they learn.
“They realize that antibiotics are not always the magical solution to everything—that antibiotics should always be on prescription, and that misusing antibiotics can do more harm than good,” said Yaseen.