Mirla Milagro remembers when she and her children ate three meals a day in Venezuela. She gave manicures and cleaned houses, and they got by. Their medical needs were all covered by the Venezuelan health system.
When the clinics started experiencing stock-outs of medicines and supplies, volunteer doctors from Cuba stepped in. But after a while, there seemed to be no medicine anywhere, and if they were available, they were too expensive. Milagro’s income also dried up. Food became difficult to get. “If we had breakfast, we’d have nothing for lunch,” she said. “If we had lunch, there would be no dinner. Sometimes we’d eat something at noon and leave a little for later. It really got bad.”
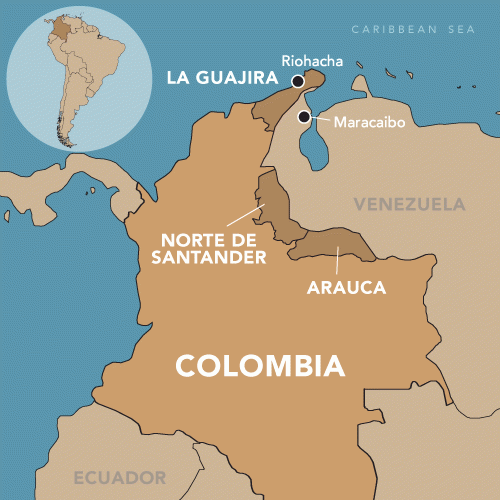
She came with her children to Riohacha, the capital of northern Colombia’s La Guajira department, looking for help. “We came skinny,” she said. As soon as she realized her children couldn’t access the Colombian school system, she sent them back to Venezuela to stay with her mother. Now she lives in Riohacha with 12 people, mostly relatives who’ve also migrated, in a shelter made of mud. She sends her mother money for food whenever she can.
More than 4 million Venezuelans have left their country since its economic and political collapse, and Colombia is hosting at least 1.4 million of them. In Riohacha, the migration is visible—people asleep in the parks and on the beach, formerly empty spaces now filled with shelters made of plastic sheeting and discarded materials, and people everywhere begging or selling whatever they can. Many of these Venezuelan migrants arrived by bus or on foot from Maracaibo, formerly the economic center of western Venezuela, close to the Colombian border. Several years ago, many of them were living relatively comfortably, like Milagro—now they’re just trying to survive.
Working to reduce maternal deaths
It wasn’t until Milagro felt sick and went to the Doctors Without Borders/Médecins Sans Frontières (MSF) mobile medical clinic in Riohacha’s La Lucha neighborhood that she learned she was pregnant. She cried when she found out. “They put me with a psychologist and everything,” she said.
The next day, at her request, MSF provided Milagro with a safe medical abortion—five pills to take over two days and directions to stay in bed and rest and come back for a check-up afterwards. When she returned, MSF also provided her with a five-year contraception implant.
Abortion has been largely decriminalized in Colombia since 2006, though women face significant barriers—from social stigma to being turned away from health structures—when requesting safe abortion care within the health system. In Milagro’s case, she says her life was at risk. Having received three Caesarean sections for previous deliveries, she’d been warned by a doctor in Venezuela that to become pregnant again would be dangerous. If she hadn’t found MSF, she said, she would have ended the pregnancy one way or another. Milagro was at risk for both complications during delivery and unsafe abortion—two of the biggest causes of maternal mortality around the world.
In Colombia—in La Guajira, as well as in Arauca and Norte de Santander departments—MSF is working to fill substantial health care gaps for Venezuelan migrants. While public hospitals are legally required to provide emergency care to whomever needs it, those services are limited to immediate lifesaving treatment, vaccinations, and deliveries. This leaves a lot of essential health needs unmet, including for women, which is why MSF has made sexual and reproductive health care—services that prevent maternal deaths and injuries—a major focus of our response to the migration crisis.
One key strategy to preventing maternal deaths is providing contraception—not just condoms, but a variety of methods that fit the needs of the individual woman and give her control of their use. This service has been well received by Venezuelan women in La Guajira, said MSF Project Coordinator Elsa Soto. “The demand is so huge that in only four months just one of our (three) teams … has tended to more than 750 family planning consultations,” said Soto.
The long-term subdermal implant, like the one Milagro received, is the most requested method, according to MSF’s Dr. Helen Aragón. “Many of them come only to see us and go back to their country, or they are constantly in and out of the country,” she explained. Contraception is unaffordable for many people in Venezuela, who are often primarily concerned with being able to buy food. MSF provides the five-year implants, three-month or monthly injections, pills, and IUDs, as well as condoms.
The demand is so large, said Soto, because women who’ve fled their country and have no stable income, no safe place to live, and may already be struggling to care for their existing children, often aren’t ready to become pregnant again.
Providing preventative care
Nevertheless, MSF is also responding to a high demand for antenatal care in La Guajira. “There is an incredible amount of pregnant women (coming from Venezuela),” said Soto. “ Most of them being in their second [or] third trimester without having had any kind of antenatal care, which creates more mortality; more complications.”
MSF teams at two hospitals and four different mobile medical clinic locations in La Guajira see pregnant women for regular antenatal check-ups, providing prenatal vaccinations and testing and treatment for tetanus, anemia, malnutrition, and sexually transmitted diseases. Patients are also checked and treated for high blood pressure, which can cause life-threatening problems for mother and baby. They receive prenatal vitamins and discuss their birth plan.
Every MSF team responding to the Venezuelan migration crisis in Colombia also includes a social worker, in part because many patients report being denied emergency care in government hospitals, including for deliveries. Social workers make certain that pregnant women receive the care they are legally entitled to so they are not left with nowhere to deliver safely, while already in an unfamiliar and challenging environment.
“(The pregnancy) was a surprise,” said Zoreima Terán, a Venezuelan migrant who has teenage children and is struggling to get by. “I never imagined that I'd go through this here.” She takes a two-hour bus ride to Riohacha from another town in order to get free, high-quality antenatal check-ups from MSF. Terán wants to go back to Venezuela, but being pregnant makes it more complicated. She can’t count on getting this care, or delivery care, in her home country right now.
At the Riohacha hospital, the government-run maternity ward is often overwhelmed with women in labor. “I would say that 95-98 percent (of the women giving birth) are Venezuelan patients,” said Maria Suárez, a doctor with the Ministry of Health. “Eighty percent of the [Venezuelan patients] we see have had no prenatal check-ups.” That means neither the patients nor the medical staff know whether there might be dangerous complications until labor is underway.
Suárez is Venezuelan; in her home country she worked in a large government-run hospital where health care was free and everything pregnant women needed was provided. But there came a time, she said, when if the patient did not bring the necessary supplies, the doctors could not provide medical care. “We didn't have a pair of gloves, we didn't have gauze, we didn't have the syringes or the painkillers for patients who arrived in pain. ... I mean, it fell apart.”
Suárez was lucky to have a profession she could practice in Colombia. Most Venezuelan migrants, including many who were professionals at home, are not able to get legal jobs in Colombia and they struggle to get by. They often make crafts to sell, gather recyclable materials they can exchange for a little money, or sell coffee on the side of the road. Some turn to sex work.
Reaching sex workers
In La Guajira, sex workers are hired in billiard halls or bars or work in less-formal situations. Regardless, they have a specific set of health needs and can be difficult to reach.
“The main challenge we face with them is shame that they have to come to us and say, ‘I am a sex worker’ or’ I’ve come to get these (STI) tests,’” said Arágon, the MSF doctor. “So, what we do is try to identify them and cultivate their trust so they can open up to us and we can provide everything MSF provides to them.”
MSF offers sex workers free testing and treatment for sexually transmitted infections, including lab work that would otherwise be expensive for them. If a patient is HIV-positive, they are referred to another organization that provides HIV treatment.
“We work (to feed) our children,” not to pay for lab tests, said Sofia Sánchez*, a Venezuelan mother of two children and a sex worker. “(MSF) offered us help, we each took an HIV test. It costs 100,000 pesos ($30)—here, they did it for free, they didn't ask us for anything.”
In addition to testing, treatment, and contraception, MSF provides mental health counseling to sex workers who might be experiencing psychological distress. “Every day, I cried. I was having a bad time,” said Sánchez. “Thanks to the psychologist—I told him everything. Thanks to him, I am already freer because he gave me some advice that really helped me.”
The sexual and reproductive health services MSF offers to Venezuelan migrants in La Guajira address the same needs we see in nearly all of our projects around the world where health systems have weakened or collapsed as a result of conflict or political instability. And, like vaccinations, nutrition support, and mental health services, they are part of an essential package of lifesaving care. “These are basic women’s needs,” said Soto.
*Name changed to protect identity