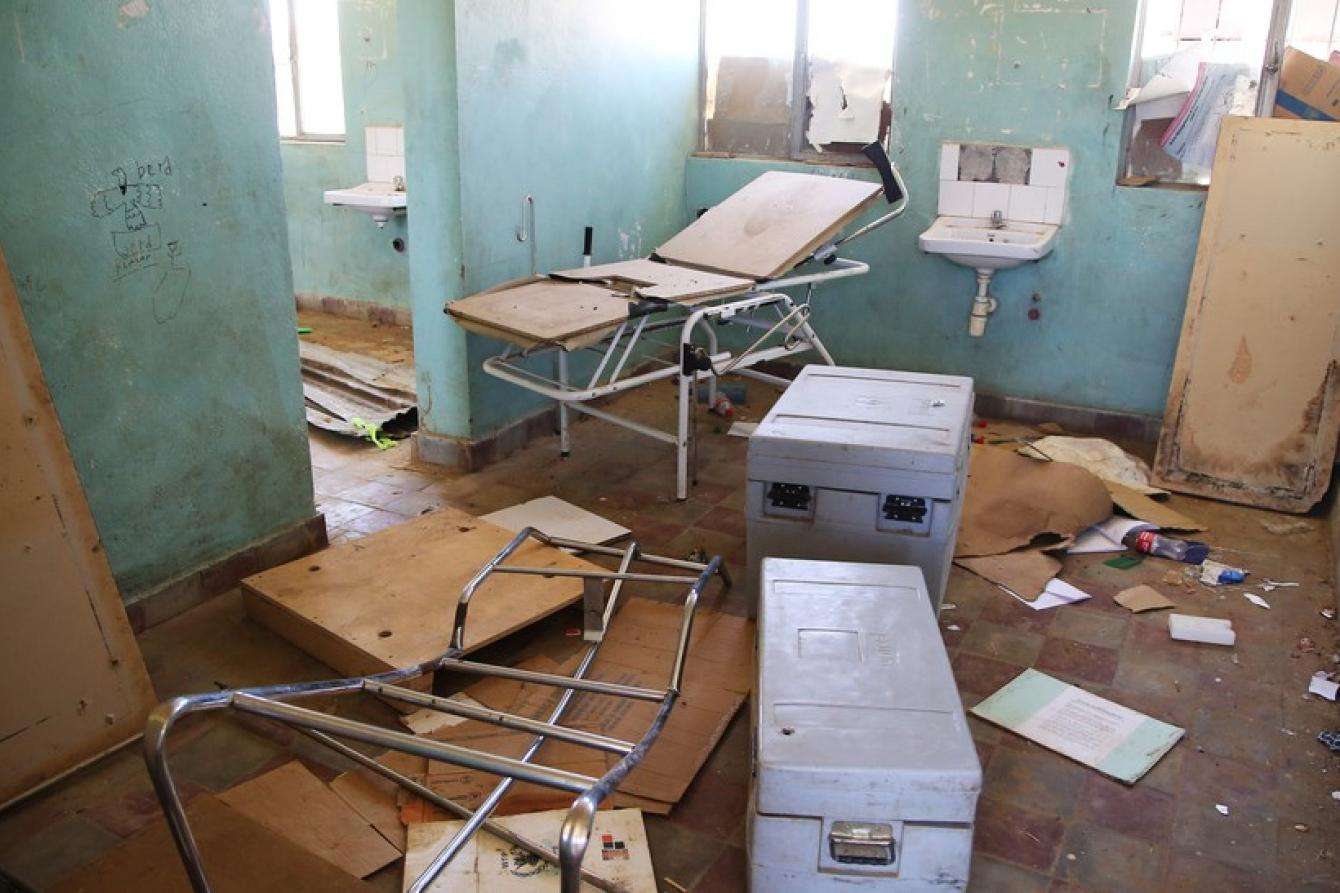
When a small Doctors Without Borders/Médecins Sans Frontières (MSF) mobile team reached the Ethiopian village of Adiftaw for the first time in mid-March, they found the health post had been looted and partially destroyed. Medical files, broken equipment, and torn medicine packaging were strewn across the floors of every room. None of the beds had mattresses, and no medical staff were present.
Adiftaw is a town of 10,000 people in the conflict-hit Tigray region of Ethiopia, three hours north along hilly dirt roads from the regional capital of Axum. What the team found there was part of a shocking pattern, mirrored by their experiences on almost every visit to a new place anywhere across this region. Many of the six million people who call Tigray home live in remote, mountainous areas that are extremely difficult to reach. Unable to access medical care and other essential services, they are bearing the brunt of the conflict that has convulsed the region for six months.

The MSF team had come to care for children, pregnant women, and those in need of emergency care. But soon people of all ages were arriving, seeking treatment they had been unable to reach for months. Young men came carrying an elderly man, apparently sick with malaria, on a wooden chair attached to an improvised stretcher. Several elderly women appeared, seeking treatment for chronic conditions. About an hour after starting triage, the MSF team had no choice but to announce they could not let any more patients in that day. The medics did not have the capacity to see anyone else in the three-hour window before the regional curfew went into effect.
The impact of violence
The violence that has gripped the region has had devastating impacts, and not only on people’s health. Some of Adiftaw’s farms were still occupied by soldiers, the town’s mill was not functioning, and the water system was broken after the pumps at the boreholes had been deliberately shot. As a result, people had to walk for hours to fetch water from a river, which they said was a source of diseases like diarrhea.
At the time of the MSF team’s visit, more than 100 houses had been burned or damaged as a result of shelling and other violence. Dozens of people had reportedly died or gone missing, with some believed to still be hiding in the mountains. In recent weeks, some had come back only to find their homes in ruins and people from other parts of Tigray, such as Humera and Sheraro in the west of the region, occupying the town after being forced to flee their own homes.
“When we arrived in Tigray in late 2020, we found that the health system had almost completely collapsed,” said MSF emergency coordinator Tommaso Santo. “Once we had set up support in hospitals in big towns such as Adigrat, Axum, and Shire, it seemed essential to us to reach the more remote areas where people’s needs are greater.”
Over recent months, MSF emergency teams gradually expanded activities to outlying areas across Tigray and currently run regular mobile clinics in about 50 different locations. “Every time we get access to a new site, we send in a small team that can provide a minimum package of medical services,” said Santo. “We are finding people with very little access to drinking water and food distributions, and who cannot make a living due to some markets being closed. Many people are still living in fear in a situation of insecurity.”
There is also a clear need in rural areas for care for survivors of sexual violence, which has been a recurrent issue during this conflict. Over recent months, MSF-supported hospitals in cities have been admitting rising numbers of women seeking assistance to cope with traumatic experiences and terminate unwanted pregnancies.
Our teams are seeing large numbers of pregnant women with medical complications, some of whom are malnourished, which can increase the risk of diseases and death during pregnancy and childbirth. While child malnutrition rates vary from place to place, moderate acute malnutrition has been on the rise in general across Tigray in the last months, said Santo, as the quality and quantity of food available has fallen sharply, with many families eating just one meal of bread a day.

Some areas are already showing levels of severe acute malnutrition well above the emergency threshold, like pockets in the outskirts of the city of Shire and in Sheraro. And with the rainy season looming, the outlook for the coming months is grim, as the fighting has left farmers unable to get to their fields.
Well-functioning rural clinics now stand in ruins
Prior to the conflict, Tigray had a well-functioning and well-equipped health system that was among the best in Ethiopia. Health centers and health posts in rural areas covered people’s basic needs and were connected to the main hospitals through a fleet of ambulances that transported patients in need of specialist treatment.
One such rural health center was in the town of Sebeya, near the Eritrean border. From the outside, the complex of buildings, which used to serve a catchment area of around 17,600 people, looks impressive, with its solid, well-spaced concrete buildings and various demarcated areas.
“Services here were good,” said Fatimah*, a 27-year-old woman from Sebeya. “I gave birth to all my four children here. If the health staff didn’t have the capacity to do something, they’d send you to Adigrat. I never had to go, but other patients would be taken there in the health center’s ambulance.”
Currently, the ambulance is missing and Fatimah, who is seven months pregnant, will not be able to deliver her fifth baby at this health center. Just meters from where she was waiting for a prenatal consultation with MSF medics, the health center’s delivery room—where 40 to 50 women used to give birth each month—lay in ruins.
In mid-November, during the fighting, a number of rockets hit the building and an administrative structure. The two delivery beds and a radiant warmer for newborns were now covered in dust, plaster, and splinters of wood, and the floor was a mess of papers, damaged pressure gauges, broken instruments, and dirty clothes. The harsh light of the dry season shone through a big hole in the wall and multiple smaller ones in the ceiling.
“These days women are delivering at home,” said Solomon*, a health worker. “Even if the birth goes well, newborns face the risk of dying. People with chronic conditions such as HIV, tuberculosis, or diabetes are suffering due to the interruption of their medication. Children are dying due to pneumonia and malnutrition.”
Fear and loss of livelihoods
For the residents of Sebeya, the partial resumption of medical services through a mobile clinic is a positive step, but the needs are immense. Most people here have lost their livelihoods and experienced months of harsh conditions, if not direct violence.
“I was a merchant before the crisis,” said Mariam*, as she waited for her prenatal check-up. “I had a shop selling coffee, sugar, and cleaning materials, but now it is closed. It was looted after we fled the town to seek refuge in my in-laws’ village. I was in hiding for four months and, even now, I am not yet back here permanently. I used to have a good life and my only concern was improving the business,” she said. “We never thought the conflict would hit us. I never thought I’d find myself without food and having to hide in the bush.”
Close to 300 medical consultations were carried out in Sebeya and Adiftaw by MSF’s mobile clinic teams. Apart from sexual and reproductive health issues, the most common conditions seen, particularly among children, were malnutrition, pneumonia, diarrheal and skin diseases related to poor living conditions and little access to clean drinking water.
Insufficient aid beyond towns and cities
“We try to prioritize the areas where we should continue responding,” said Santo. “And we try to increase the package on offer: it might be family planning, prenatal consultations, vaccinations, or other services, none of which have been available for months.”
Much remains to be done to expand people’s access to sexual and reproductive health care and other critical support services. While humanitarian organizations have sent teams to Tigray, especially since February, the response on the ground is still extremely limited, and hardly ever extends beyond the larger towns. There are still rural areas in Tigray that neither MSF nor any other organization has been able to reach. We can only assume that people living in these areas are also without access to health care.
“Rural areas are often left without any kind of assistance, and in recent weeks access for humanitarian organizations to various parts of Tigray has been further constrained,” said Santo. “There is an urgent need to scale up humanitarian assistance and to expand its reach.”
MSF currently runs medical projects in the cities and towns of Adigrat, Axum, Adwa, Abi Adi, Shire, Sheraro, Humera, and Dansha. Since early 2021 MSF mobile teams based in these locations have progressively expanded their activities to rural towns, mountainous areas, and villages in parts of the region where the health system is not functioning.
Over recent months, our mobile teams have visited more than a hundred different locations, either to run temporary mobile clinics or to train health staff and resupply looted health centers.
*Names changed to protect anonymity.





