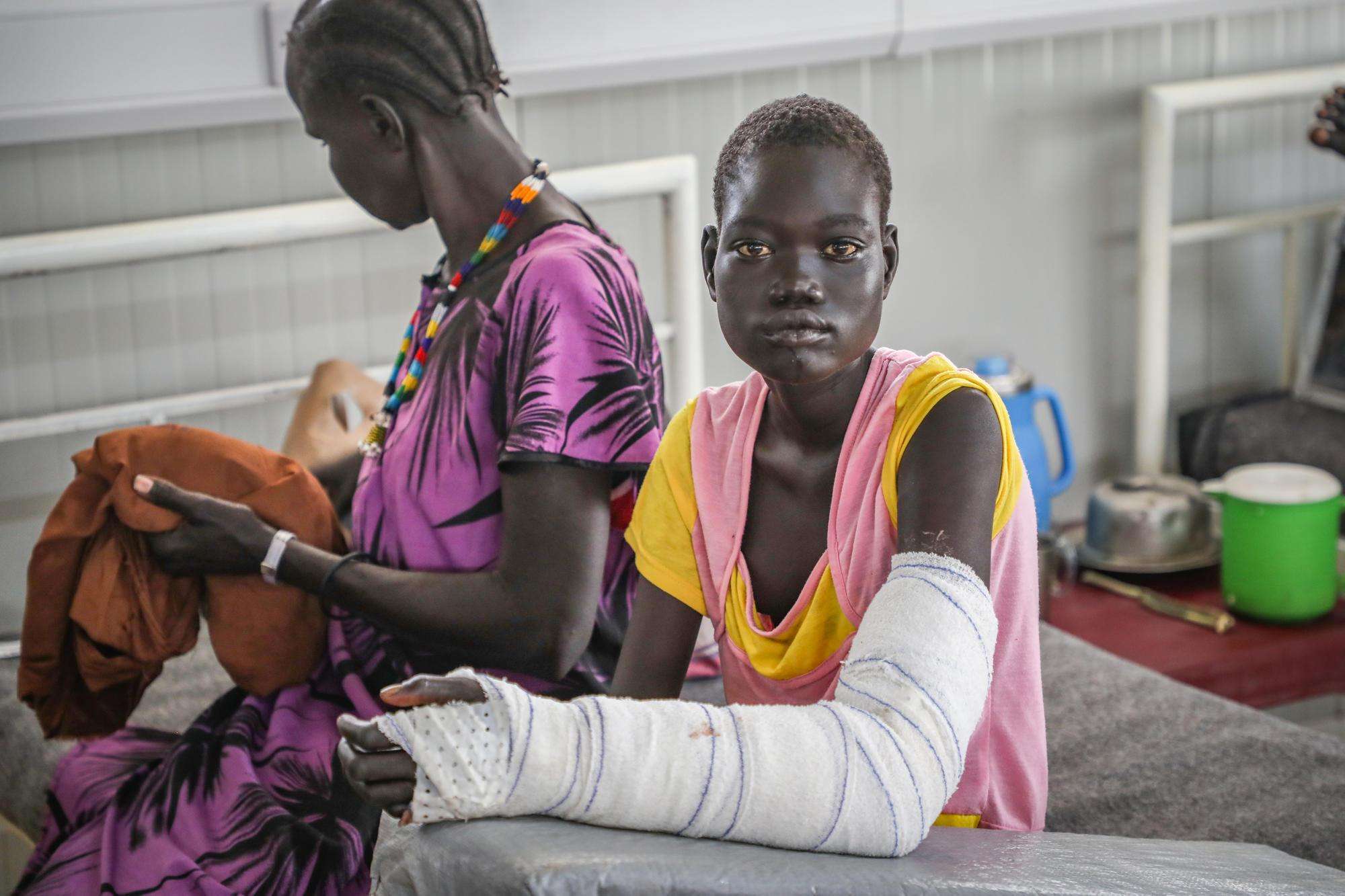
The first sign of a snake bite is the bite itself, often on the victim’s arms or legs, and showing two distinct puncture wounds from the snake’s fangs. It is important that the correct type of snake is identified, since this helps in choosing the appropriate antivenom. At MSF’s clinics, patients can often do this using photos of local venomous snakes. Many patients are understandably stunned immediately following a snakebite, however, and often cannot recall its shape or markings.
If the patient and medical staff are unable to identify the snake based on recall or wound appearance, they may rely on the symptomology of the patient, since the symptoms, described above, vary from snake to snake. This approach has its own difficulties, however, since the composition of snake venom can vary within species and even within generations of the same species. This variation thus potentially produces different symptoms than may be expected.
A final diagnostic approach is through laboratory analyses, which many low-resource settings lack the capacity to carry out. A patient’s blood can be tested for various clotting patterns and abnormalities, which can give clues to both the type of snake and the severity of the envenoming.