Outside Nsanje district hospital, the only public hospital in this part of southern Malawi, there is a steady stream of people seeking care for HIV/AIDS. According to government estimates, some 25,000 people in Nsanje district are HIV positive—that’s about 12.5 percent of the local population, and significantly higher than the national average of 9.2 percent.
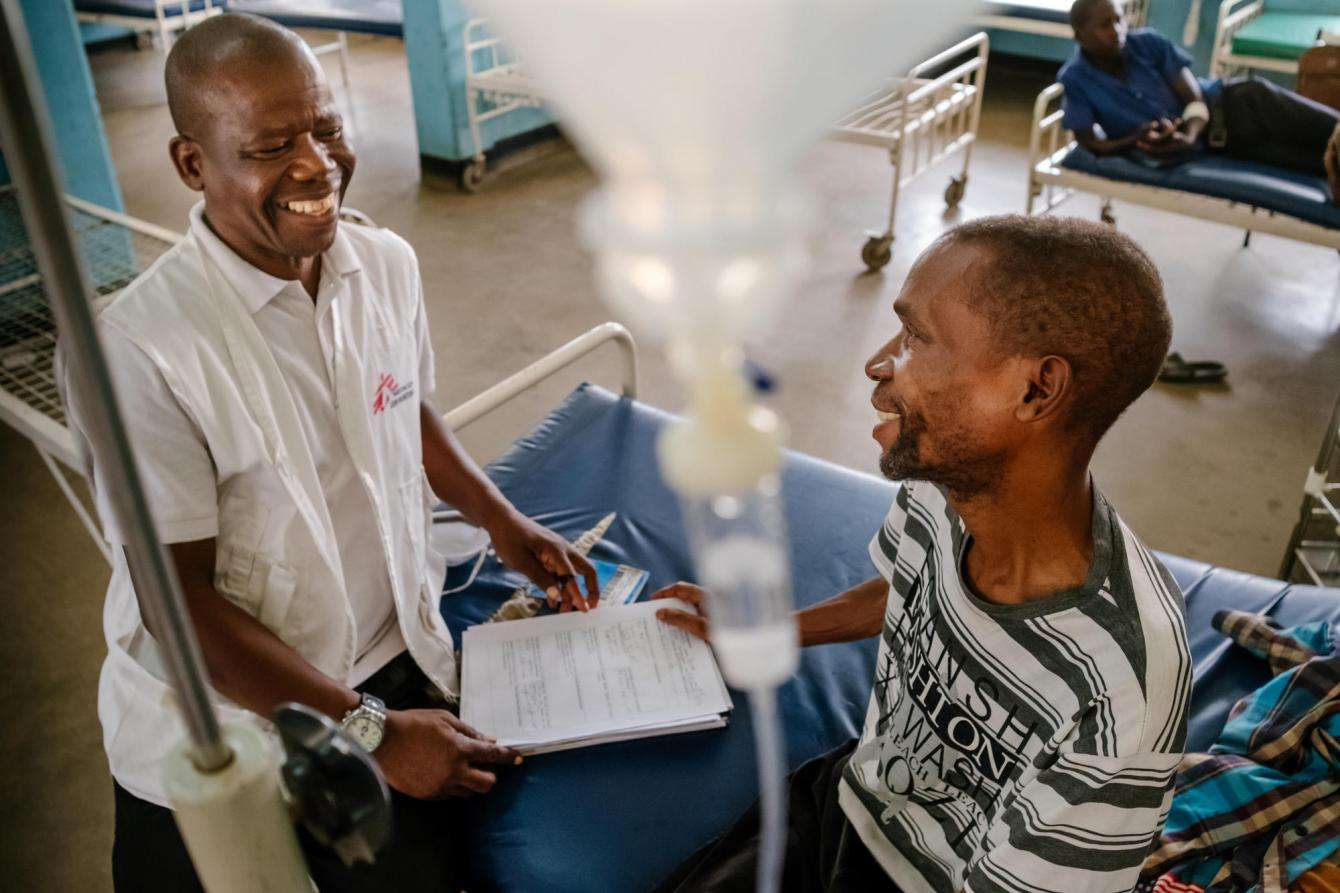
One of these patients is Austin, who was brought in by ambulance and admitted to Nsanje hospital in October. He had lost a lot of weight and was urinating frequently. He tested positive for HIV in 2016 and had been receiving antiretroviral (ARV) treatment. His health quickly deteriorated when he stopped taking his medication. “I quarreled with my wife,” Austin says. “I told her it would be better for me to die. I stopped taking my medication for three months and soon got worse.”
Since MSF began working in Malawi, staff have noticed that many people struggle to maintain their ARV treatment programs for a variety of reasons. “Some believe that it is better to go and seek help from a traditional healer,” says Brains Kamanula, who provides psychosocial support and mentorship at Nsanje district hospital.
Other issues include distance and economic challenges. The nearest health facility can be far away, and the transportation to get there can be expensive. Instead of going to the hospital, many people have to prioritize working to survive and support their families.
“People also lack basic knowledge about the warning signs of HIV. Even though MSF has health promoters that go to communities to raise awareness about the danger signs, we can’t reach everyone,” says Kamanula. “In the end, by the time they come to the hospital, many people are already very sick.”
Circle of care
Malawi has long struggled with a high prevalence of HIV/AIDS, which causes an estimated 13,000 deaths a year. In recent years huge investments have been made by international initiatives such as the Global Fund and PEPFAR to treat people with HIV and reach the UNAIDS 90-90-90 target by 2020. This target commits a country to ensuring that 90 percent of people living with HIV will know their HIV status, 90 percent of people with a diagnosed HIV infection will receive sustained ARV therapy, and 90 percent of people receiving ARV therapy will have viral suppression. Lately, however, progress toward reducing the number of HIV-related deaths has stalled.
In an effort to improve care for people with advanced HIV in Nsanje district, MSF and the Ministry of Health have established a new operating model called the circle of care. This new model of care could help communities spot the symptoms of HIV more quickly and speed up the referral process.
“The circle of care model aims to reduce mortality among HIV patients through early detection and strengthening the referral system within the circle, [including] the community, health center, and the hospital,” says Jomah Kollie, medical team leader for the Nsanje project. “This is achieved by enabling communities to identify sick patients, ensuring efficient diagnosis and initiation in the health centers, and in-depth assessment and quality care in the district hospital.”
When a patient arrives at the Nsanje district hospital, they are brought to the rapid assessment unit where they can be quickly stabilized and assessed. Once this is done, the patient can be put on the right treatment and admitted to the ward.
“It will not happen again”
25-year-old Lita is sitting with her parents in the shade outside the female ward at Nsanje district hospital. For her it all started when she wasn’t feeling well at the beginning of the year. Her family brought her to the hospital, where she tested positive for HIV. Lita was advised to start taking ARV drugs. But after she was discharged, she stopped taking her medication, and, as a result, she started to get sick again.
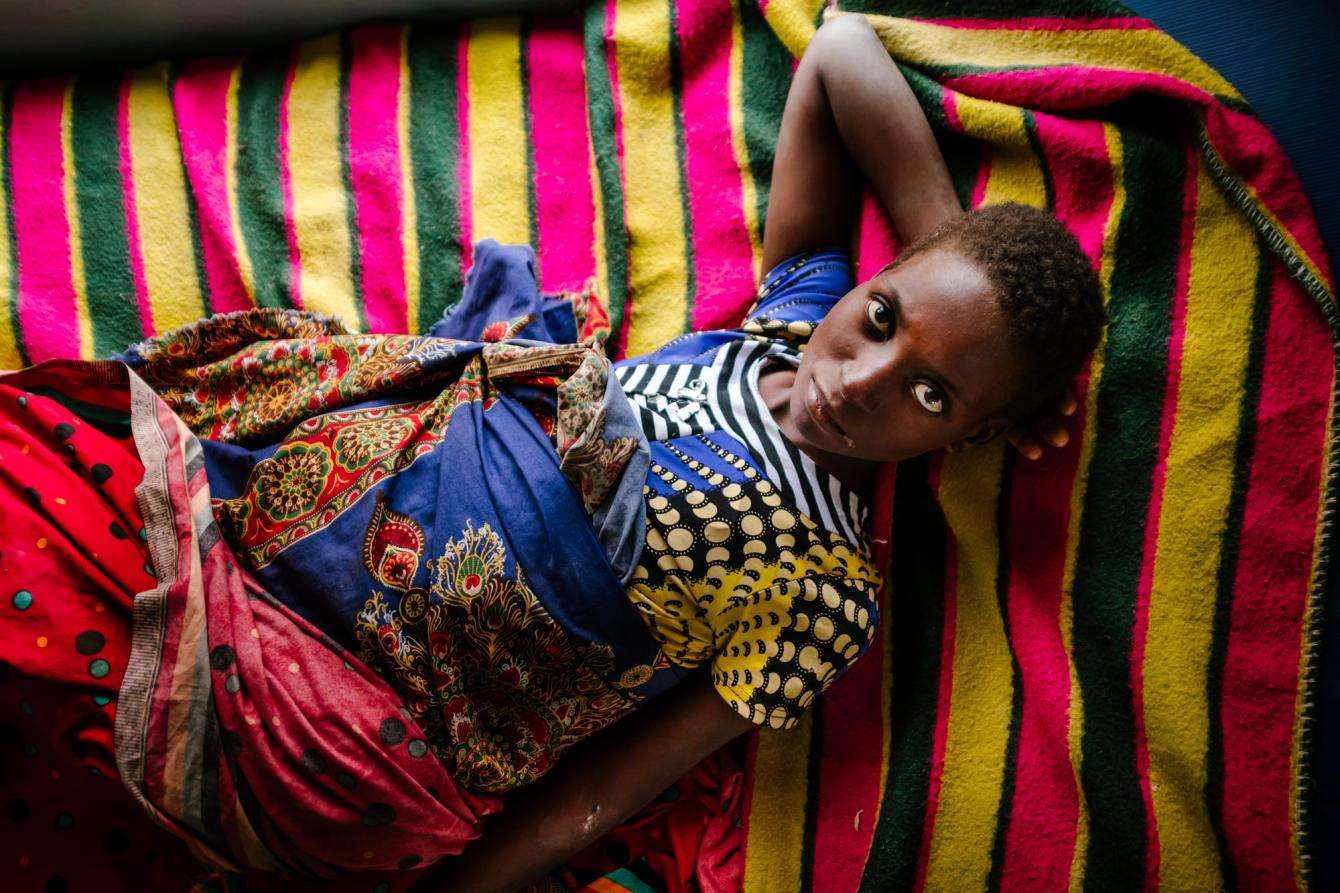
Lita was readmitted to Nsanje District Hospital in October with a fever, bloated stomach, and leg swelling. This time, her father is determined to make sure his daughter follows her treatment program. “It will not happen again, as I will be around,” says her father, Gerrald. “I will be there making sure that when she wakes up, I am there, and she takes her drugs. The same with the evening dose, I will make sure that before she goes to sleep, she has taken her drugs.”
Not many days ago, Lita was unable to walk without support. Now she is feeling better, but she misses her three-year-old daughter. The next step for Gerrald is to get his granddaughter tested as well. “I want to bring her here for testing so that we get to know her status – if she is HIV positive or negative,” he says.
Working with the community to help people with HIV
The circle of care starts at the community level. In Nsanje district, MSF community health workers coordinate with traditional authorities, patient groups, and local associations to reinforce existing community structures and identify those who are sick and need more care. They also help raise community awareness of the symptoms and danger signs.
“Previously, most HIV/TB [tuberculosis] activities were done at a health facility level and not much in the communities. As a result, people who defaulted [from treatment] had no proper follow-up,” explains Moses Luhanga, information and education manager.
When someone is identified as requiring further treatment, they are then referred to a nearby health center. In Nsanje, MSF, working with the Ministry of Health, has instituted a package of care which begins with a very quick assessment and some tests: CrAG for cryptococcal meningitis, a CD4 count, and a test of blood sugar levels and urine. If the patient has a condition requiring advanced management, they are referred to the district hospital.
"I want to be the voice of change"
Back at the hospital, Austin is getting ready to be discharged. He and his wife are carefully wrapping up their belongings in chitenges, brilliantly colored fabrics used in Malawi. After 12 days at the hospital, they are happy to go home.
To make sure that Austin and other HIV positive patients being discharged stick to their treatment programs and don’t get advanced HIV, MSF has a post-discharge procedure involving visits from the counselors. Although Nsanje district is close to meeting the 90-90-90 targets, the next challenge will be to make sure people on HIV medication continue their treatment and receive quality care if they fall sick.
Getting people to know their status and start the treatment are steps in the right direction. Before the circle of care was implemented in the district, statistics from Nsanje district hospital indicated that 27 percent of people entering the hospital with advanced HIV would die. But since the system was implemented, there has been a gradual reduction in the mortality rate of hospitalized patients with advanced HIV; over the last year, the mortality rate was under 15 percent.
For people like Austin, getting the care he needed not only made him well, it also inspired him to make sure other people who are HIV positive get to know their status, and then start and stay on the lifesaving treatment.
“I want to be the voice of change in my community. I want to find people who are suffering from HIV and change this community to be disease-free,” says Austin. “After being looked after, I cannot just stand here while someone is suffering.”




