In the Doctors Without Borders/Médecins Sans Frontières (MSF) clinic in Abdurafi, northern Ethiopia, a young woman with a swollen face sits on a bed, awaiting the results of a blood test for snakebite envenoming. Workey Mekonen was bitten on her forehead by a small snake while sleeping on the ground in a farm shed.
The remote region of Amhara in northern Ethiopia is known for its fertile land and its vast commercial farms cultivating sesame, sorghum, cotton, and other crops. It is also home to some 20 species of venomous snakes endemic to this part of Africa. In search of work, almost half a million daily laborers migrate every year from the highlands of Ethiopia to the lowland farms surrounding the town of Abdurafi. They usually arrive in August for the start of the harvest season. Most leave in October, but others stay on until early January for the sorghum harvest. During the peak of the harvest season, farm workers in the fields come across snakes almost every day.
Snakebite is a neglected killer
Snakebite envenoming is overwhelmingly an affliction of the rural poor in agricultural and herding communities and kills more people than any other disease on the neglected tropical diseases (NTDs) list of the World Health Organization (WHO). An estimated 2.7 million people are bitten by venomous snakes worldwide every year, resulting in death for more than 100,000 people and life-long disfigurement and disability for 400,000 more.
“Workey soon felt better and, after five days in our clinic, she could be discharged fully recovered,” says MSF’s Dr. Ernest Nshimiyimana. “She was lucky that she was brought to us in good time and treated with effective antivenom.”
Unfortunately, in most parts of the country, effective antivenom is either unavailable or is too expensive for the communities most affected by snakebite.
Dr. Ernest Nshimiyimana
Immediate treatment is essential
Since her husband died four years ago, Workey has earned a meager living for herself and her four children by cooking for farm laborers in the fields. She leaves her children with her sister in Tigray, half a day’s journey from Abdurafi, while she works.
The previous night Workey awoke with a sudden piercing pain in her forehead. When she caught sight of something slithering away across the floor, she realized she had been bitten by a snake. She had been sleeping on the ground of an open shed where crops and other farming materials were stored. Relieved at first that it was only a small snake, the pain and swelling soon made her fear for her life.
Fellow farm workers took her to her uncle, who lives nearby. He had heard about the MSF clinic in Abdurafi town, which treats people for snakebite free of charge, and took her there. By that time, Workey’s face was so swollen that she was unable to see. She was immediately admitted to the clinic for close monitoring.
Ten minutes later, Workey’s blood test result is ready. It shows no blood clotting, a clear indicator that the snake has injected its venom and that she needs to be treated with antivenom. MSF Clinical Officer Degifew Dires prepares the infusion and administers it intravenously, a process that will take 140 minutes.
“The first ten minutes are critical and need close monitoring to ensure that she has no harmful reactions to the antivenom,” says Degifew. “Over the coming hours, we will regularly check her physical condition and vital signs.”
Migrant harvest workers among the most vulnerable
Not everyone bitten by a snake in Ethiopia is so fortunate, as the antivenom to treat snakebites is out of many people’s reach.
“Unfortunately, in most parts of the country, effective antivenom is either unavailable or is too expensive for the communities most affected by snakebite,” says Dr. Nshimiyimana.

Migrant workers are particularly vulnerable to snakebite. They often work barefoot in the fields at night, and use their bare hands to harvest crops. The sesame fields are particularly hazardous. Sesame does not grow very high but it does grow thickly, making it an ideal hideout for snakes. To harvest the crop, workers must crouch down, making both their hands and feet vulnerable to snakes.
“In the peak months we often have up to 20 patients with snakebite in our close monitoring room,” says Dr. Nshimiyimana. “Having been bitten, many have to travel for hours, especially those working in the remote fields, to reach medical facilities. Timely treatment of snakebite is crucial.”
Unknown numbers of victims
The number of snakebite victims arriving at Ethiopian health facilities is not recorded, making it impossible to know the national health burden of snakebites. But MSF figures give an indication of the scale of the problem. In 2017, MSF treated 609 patients in different projects in Ethiopia, 322 of them from Abdurafi. In 2018, the number has increased; by the end of 2018 MSF treated 647 patients in Abdurafi alone. These include so-called dry bites (warning bites) and bites with mild, moderate, and severe poisoning.
Antivenom is just one of a range of treatments, depending on the type and severity of the envenoming.
“In October, for example, we treated 115 patients for snakebite,” says Dr. Nshimiyimana. “Only 22 of these patients required antivenom administration, while 93 could be treated clinically. We can manage many bites conservatively with intravenous fluids, pain management, blood transfusion, and leg or limb elevation. We also treat associated infections and give wound care if needed.”
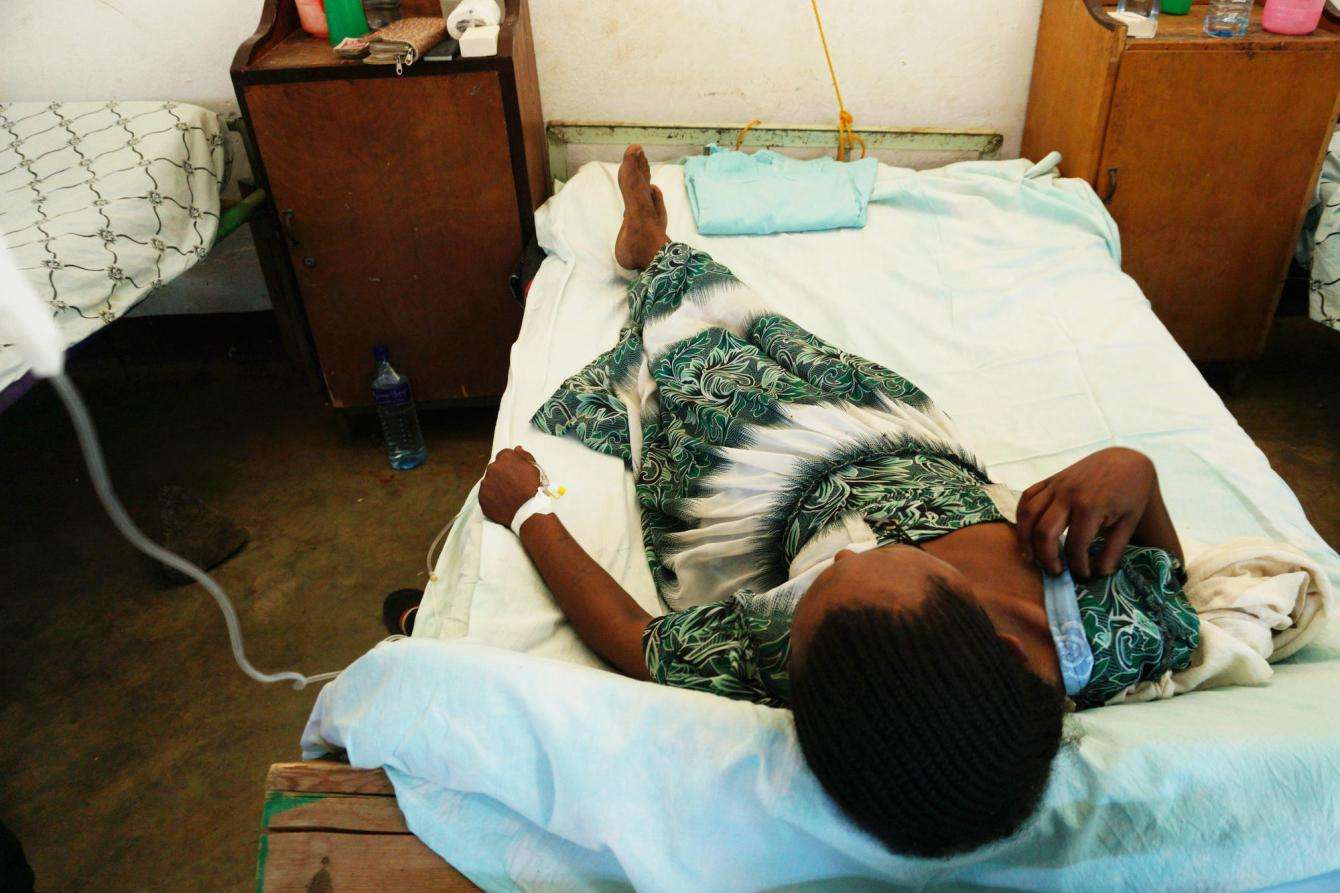
As he speaks, Dr. Nshimiyimana is doing the morning ward round in the close monitoring room. He stops to talk to a young man who was bitten by a snake on his foot while working on the family farm the previous night. The man did not require antivenom administration, and the doctor is satisfied that the development of the swelling is being monitored and documented and that he will make a good recovery.
Lack of access to effective care and antivenoms
Many more lives could be saved if all snakebite victims in Ethiopia had access to such timely and effective care. For patients like Workey, the envenoming could have been life-threatening if she had not been able to reach a clinic providing free and effective antivenom treatment.
But with almost no funding currently coming from donors for snakebite prevention and treatment, the availability of effective and low-cost antivenoms remains a bottleneck to access.
WHO has started helping countries select safe antivenoms that are effective against the bites of local snake species, but a number of manufacturers have stopped producing some antivenom products, further limiting access for the victims of snakebite.
While MSF provides treatment free of charge in our facilities, elsewhere treatment can cost upwards of US$100, making it unaffordable in rural areas, such as northern Ethiopia, where most people at risk live.
The need for quality, low-cost antivenom
Quality antivenoms that are effective against local snake species and safe when administered need to be made available, free of charge or at a price that everyone can afford. At the same time, more health care workers in remote farming areas must be trained in how to treat snakebite.
We hope that donors and governments will support the implementation of WHO’s forthcoming snakebite roadmap, an ambitious strategy to help overcome the barriers people face in accessing treatment. (WHO outlined the strategy in an article for the medical journal PLOS.)
MSF is cautiously optimistic that the WHO roadmap could be a turning point in tackling snakebite. In the coming months, we will continue to work with governments, treatment providers, donors, and communities affected by snakebite to help ensure that the roadmap is implemented and leads to real change for snakebite victims everywhere.




