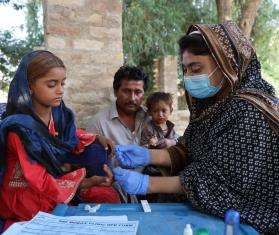
Last year, scorching heat waves broke records across South Asia. The unusually violent monsoon that followed triggered floods that killed over 1,700 people in Pakistan and ravaged communities. After the devastating weather events, which were attributed to climate change, Doctors Without Borders/Médecins Sans Frontières (MSF) set up a community-based malnutrition program in a remote part of Dadu district, Pakistan. A total of 1,236 children under the age of two and 224 pregnant women and lactating mothers were admitted to the program.
“I only used to hear about world hunger on TV and in the newspaper, but I never got to feel it on a soul level,” says MSF psychologist Vardah Ahmed. She’s originally from Karachi, four hours south from rural Dadu, where the average wage is the lowest in the country.
Dadu district is no stranger to floods, whether they’re caused by monsoon rains, melting glaciers, the Indus River overflowing, or a combination of all factors. Large parts of the region were completely cut off from the rest of the world between June and October 2022. Not one, but two harvests were lost. For many, no harvest means no income to buy nutritious food. And ongoing high inflation added to people’s woes.

MSF had been managing a program in Dadu before the floods to support local authorities with treating the neglected disease of cutaneous leishmaniasis. Once the floods hit, regular activities halted and MSF teams shifted to an emergency response. By December, two months after the water levels had receded, the medical team noticed an increase of malaria cases, while the rates of severe acute malnutrition among children tripled between September 2022 and February 2023. They then switched gears and designed a program to treat people sick with malaria, as well as nutrition activities targeting children under five, pregnant women, and lactating mothers.
Treating malnutrition in hard-to-reach areas
Malnutrition remains a public health issue in Dadu district, mainly affecting mothers and their children. Maternal and child malnutrition are interrelated and caused by multiple factors such as the unavailability or lack of access to adequate health services like pre- and postnatal care, vaccination, basic sanitation, and mental health. These issues are magnified for the most vulnerable during extreme weather events.
“Once, a man brought his malnourished child to us,” Vardah recalls. “She was severely anemic, on the verge of death, and we convinced the father she needed to be hospitalized. But the elders of his house refused, arguing that they don't have money to pay for food and accommodations for an adult to accompany the child while she is hospitalized in the city. So they didn't go, and I don't know what happened to the baby. I cried a lot that day.”

MSF treated 127,400 severely malnourished children at inpatient feeding centers (ITFC) across the world last year. But in Pakistan, ITFCs are managed by the Ministry of Health, so MSF focused on outpatient care. Each morning, teams climbed aboard MSF vehicles and drove a couple of hours in the scorching heat until they reached the location of one of the 10 MSF ambulatory therapeutic facilities (ATFC), usually set up in local health posts, which are often little more than four walls and a roof. There, patients received nutrition support alongside health promotion advice and psychological help.
“After exchanging with local health authorities and in close collaboration with them, we decided to focus on hard-to-reach areas where there was no one else proactively seeking severely malnourished patients in the most remote and destitute parts of the district,” explains Rinako Uenishi, MSF’s project coordinator in Dadu.
Though activities were set up as close as possible to patients, the population is so spread out in this huge district that some of patients live over 10 miles away from the closest ATFC. In a region with no public transport apart from the few motorcycle taxis, it meant those patients needed to walk the equivalent of a marathon round trip just to get access to therapeutic food.
“It is obviously not sustainable for vulnerable people, and we didn’t want to add yet another burden on them. So patients living in the most remote areas were given two weeks’ worth of supplements,” says Rinako.
The challenges of food provision
“We can’t just tell people to include meat, fish, and these type of expensive things in their meals,” says Anis Bibi, the manager of MSF’s health promotion team, who is originally from the city of Hyderabad. “They know what is good, but they can’t afford it. Once, a woman was patiently listening to us giving her advice on which nutritious foods to eat. And at the end she just said,’ I don't have one meal to eat.’”
Three-quarters of the children admitted to ambulatory feeding programs were under two years old. This could be due to maternal undernutrition during pregnancy and struggles with breastfeeding. Lactating mothers require extra support—273 pregnant and lactating women were admitted to the program—ensuring that, through breast milk, young children can receive the nutrition they need.
“Mothers who work in the fields can’t breastfeed their children because no mother will take their child in the field in 120-degree heat. So they give bottles of water and a bit of sugar to the eldest child or the mother-in-law to give to the baby during the day,” Anis explains.

The provision of therapeutic food, a cornerstone of malnutrition response, is not as simple a task. “At the start of the nutrition program, we were alarmed because the ratio of cured patients remained very small,” Anis recalls. “But soon we discovered that some of the people were thinking that the therapeutic food we distributed was like a candy that anybody can enjoy. So we organized a small group of health volunteer committees in the hamlets to explain that [therapeutic food] is a medicine for severely malnourished children only. The impact of those health volunteer committees was very, very, fruitful and our program cure ratio increased.”
The toll of malnutrition on mental health and families
Vardah recalls one story that especially moved her. “A woman was telling us that her husband was not letting her feed the therapeutic food to their malnourished child; he was giving it to his other, healthy children, from his first wife who had passed away,” she says. Through couples counseling, they were able to discuss how his wife’s mental health was also important. “If she's not happy, “if she's not in a good state of mind, she won't be able to take care of your home,” says Vardah. “Three weeks after this session I saw the mother again. She was taking care of herself, her child walked better, and her weight had also increased.”