This article is part of the Winter 2018 issue of Alert—2018: The Year in Photos—featuring some of the most striking images and stories from our work around the world.
Emergencies like conflict and natural disasters can inflict both visible and invisible wounds. People seek mental health care for many reasons—the loss of a family member in an earthquake, the trauma of violence suffered or witnessed, or the stress of forced displacement. MSF teams provide mental health care and psychosocial support through both individual and group sessions to help people cope with extremely difficult situations.
Bangladesh

In Bangladesh, where hundreds of thousands of Rohingya refugees have settled after fleeing targeted violence in Myanmar, MSF psychologists work with patients who have survived horrific abuses. Teams provide care for victims of sexual violence, creating a “place of peace” for women to talk about their experiences and support each other. Mental health services are integrated into MSF’s medical facilities, enabling teams to reach patients who might not seek out psychosocial care due to lack of awareness or stigma.
Terrible living conditions in the camps in Bangladesh and limited prospects for the future also contribute to high levels of stress and domestic violence. “Many people are on edge, not just because of the recent trauma but because of the long-time trauma of witnessing horrific things [in Myanmar],” said MSF psychologist Cynthia Scott. Many patients say they have difficulty sleeping, paralyzed by the fear that someone might come into their homes and haunted by memories of attacks by Myanmar security forces.
Iraq

In Iraq, where years of conflict have forced millions to flee their homes, MSF teams work in camps for internally displaced people, providing counseling to help them process their experiences and cope with the difficulties of their daily realities. Though the city of Mosul was retaken from the Islamic State (IS) group in 2017, the local health system remains decimated and many people are living amid the rubble of ruined homes. They carry with them the psychological scars inflicted by years of life under IS and the fierce fighting when US-backed Iraqi forces retook the city.

Many people remain displaced elsewhere in Iraq. MSF works in six locations around the camps for internally displaced people near Mosul and Erbil, providing mental health services including both psychological and psychiatric consultations, group therapy, psychosocial counseling, and therapy for children.


Mexico
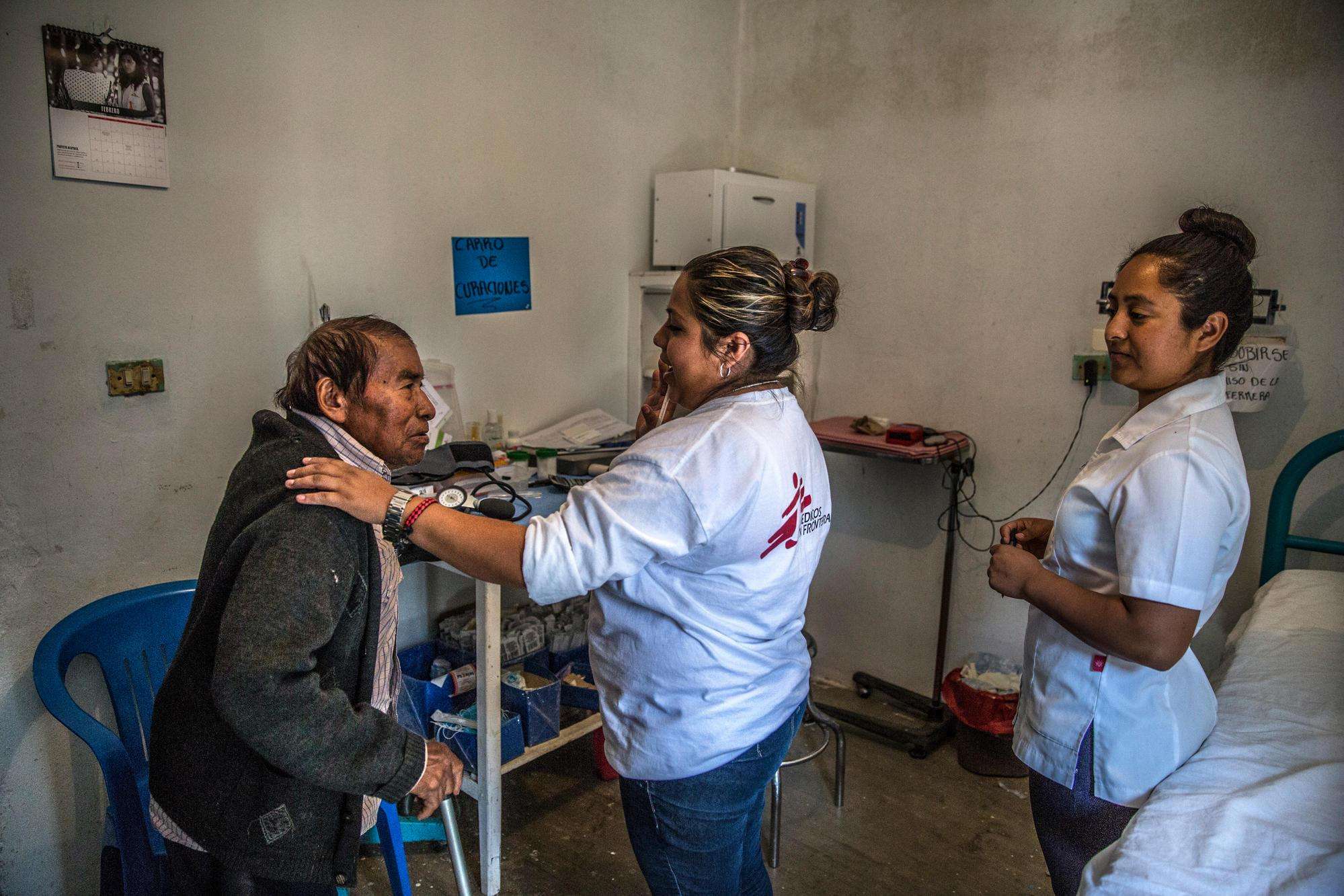
In Mexico, MSF psychosocial teams care for refugees and migrants from Central America traveling the dangerous route north and for local communities trapped in places gripped by criminal violence. In Guerrero State, for example, where territory is fought over by organized criminal gangs vying to control trade, extort communities, and force recruitment, we run mobile clinics to provide both primary and mental health care in isolated communities and in the city of Acapulco.

The constant threats and violence take a heavy psychological toll, especially on those living in rural regions far from care. “We treat people who have been through very traumatic experiences,” said Laura Moreno, MSF mental health activities manager. “People in Guerrero are tough, but if the fear and violence persist, the fabric of society could be torn apart. That’s why providing mental health care is so important here. The support we give helps to strengthen people’s coping mechanisms, so that they can manage their emotions in times of uncertainty and violence.”









