Leaders of wealthy nations, pharmaceutical corporations, and COVAX must act now to prevent more suffering and deaths
NEW YORK/JOHANNESBURG, FEBRUARY 18, 2021—As COVID-19 continues to sweep across Southern and sub-Saharan Africa, the international medical humanitarian organization Doctors Without Borders/Médecins Sans Frontières (MSF) is calling on wealthy states and pharmaceutical corporations to ensure that all countries can access effective vaccines quickly and affordably before more people die. The situation in Southern Africa is dire, as a highly infectious variant of the novel coronavirus, 501Y.V2, continues to spread, further straining fragile health care systems.
Equitable access to and distribution of COVID-19 vaccines is more critical now than ever. It’s also vital that countries are receiving the appropriate vaccine—one that’s effective against the coronavirus strain they’re battling. The latest initial data indicates that some COVID-19 vaccines may be less effective than others against the South Africa strain. The region has been forced to halt and adapt its planned vaccine rollout of one particular vaccine, produced by Oxford-AstraZeneca, due to findings indicating decreased efficacy against the dominant 501Y.V2 variant.
“The emergence of new COVID-19 variants should be a major consideration in determining the allocation of vaccines to countries around the world,” said Dr. Tom Ellman, director of MSF’s Southern Africa Medical Unit. “Truly equitable vaccine allocation and distribution should mean that countries are able to acquire not just any vaccines but the right vaccines—adapted to the presence of new variants and to contextual factors—at the right time and at the right price.”
After a scramble last week, South Africa—where the new variant was first discovered—acquired a different trial vaccine, made by Johnson & Johnson, to ensure its most at-risk frontline health care workers get protection in a limited rollout as part of an implementation study, starting this week. South Africa is now offering to share its initial unused vaccine consignment with the African Union for use in appropriate countries where the 501Y.V2 variant is not predominant.
It is clear that accessing vaccines for low- and middle-income countries will remain a serious problem unless systemic issues linked to agreements between wealthy nations and pharmaceutical corporations are dealt with.
“Unless the leaders of wealthy states and pharmaceutical corporations support this, and quickly, we risk generating new pandemics of vaccine-resistant COVID-19. Travel bans will not stop this, but equity and solidarity might,” Ellman said.
To date, more than 174 million people have been vaccinated globally, yet very few of these have been in Africa. Moreover, many wealthier countries, including the US, have ordered two to three times as many vaccines as are required for their populations. Some, such as Canada, are set to receive vaccines from the COVAX Facility—a mechanism established by Gavi, the Vaccine Alliance, and the World Health Organization—which many lower-income countries exclusively rely on for vaccine access.
“What we are witnessing right now is an unacceptable failure of humanity and the global response,” said Claire Waterhouse, MSF regional advocacy coordinator. “We denounce countries that hoard vaccines and that have started to immunize low-risk groups, since it comes at the expense of developing countries that haven’t even started vaccinating frontline health care workers in health facilities already stretched to the breaking point.”
To ensure equitable access to vaccines, wealthy nations that have immunized their frontline health care workers and high-risk groups should share with COVAX their surpluses for low- and middle-income countries. Additionally, pharmaceutical corporation leaders must pause or stop bilateral agreements that prioritize supply for high-income countries that can pay more at the expense of countries relying on COVAX. Lastly, COVAX leaders, Gavi, the Vaccine Alliance, the Coalition for Epidemic Preparedness Innovations, the World Health Organization, and donor states must provide speedy transparency on COVAX supplies so that low- and middle-income countries know the price, quantity, and delivery date of vaccines they will receive.
“While the COVAX mechanism is designed specifically for equitable distribution and vaccine development, it has yet to deliver a single vaccine to a country,” Waterhouse said. “It is clear that the global vaccine access system is inherently flawed, and we urge Gavi and donors to COVAX to acknowledge this and take steps to address it. Every day COVID-19 vaccines are delayed is another day that health care workers in Southern Africa and developing countries remain at great risk while they continue to care for the sick.”
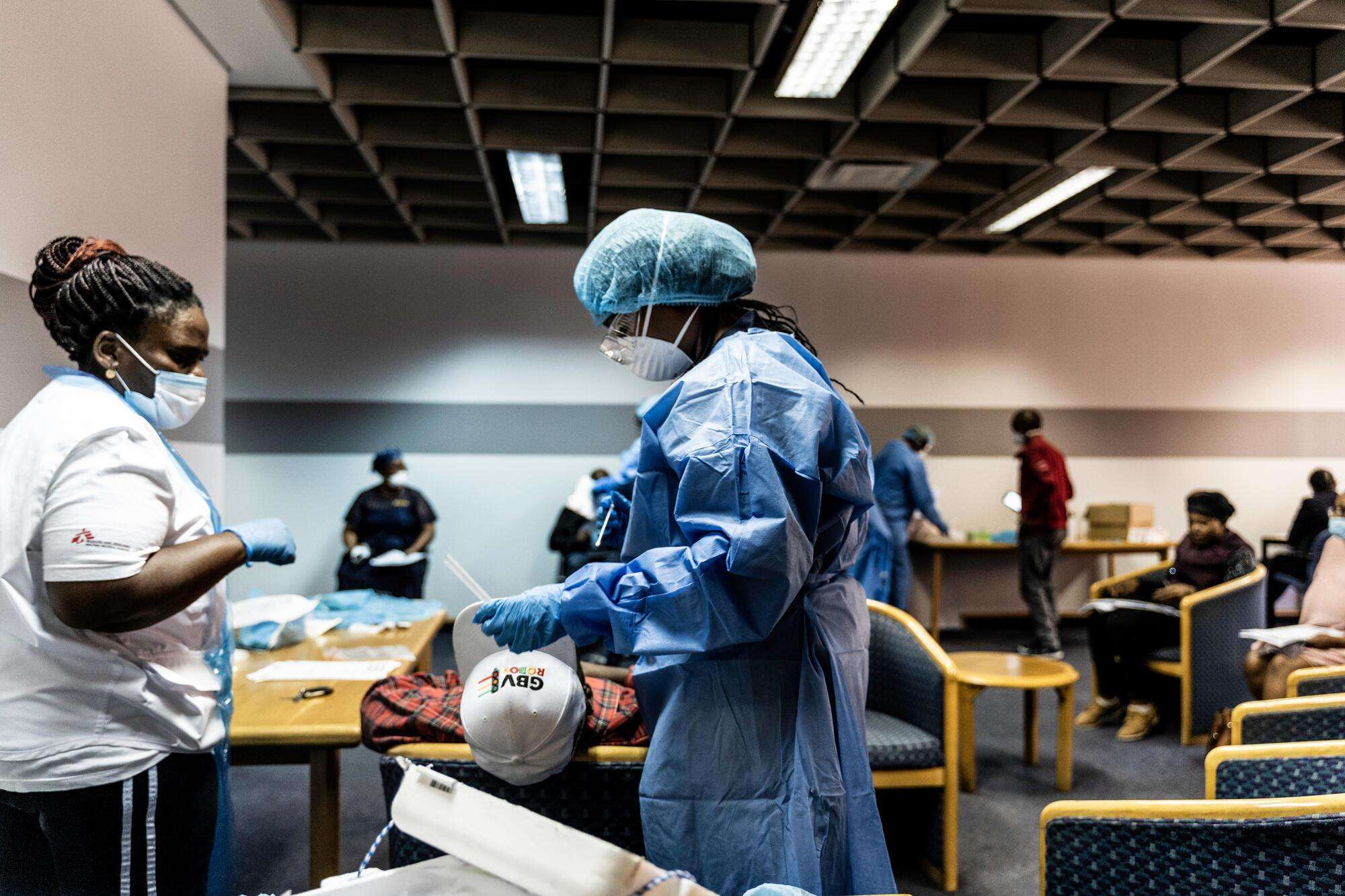
MSF teams have been providing COVID-19 treatment and prevention in different communities throughout Southern Africa—in Eswatini, Malawi, Mozambique, South Africa, and Zimbabwe—since the beginning of the pandemic. Following the holiday season, the region was shaken by a sudden ‘second wave’ of COVID-19 infections. Several Southern African countries recorded more new COVID-19 cases in the month of January 2021 than in all of 2020.
“In South Africa, there weren’t enough health care workers in many of the hotspots, and hospitals struggled to meet the demands for care,” said Philip Aruna, MSF’s regional operations manager in Southern Africa. “While the wave of new infections is starting to slow in some of these countries, we are now preparing for the possibility of future surges of COVID-19 infections as the virus continues to adapt and spread. A quick rollout of the most-effective-in-context vaccines would have a significant impact on reducing future infections and deaths among health care workers and most at-risk-groups.”