The SARS-CoV-2 virus affects different people in drastically different ways. Some have no symptoms at all, while for those who do develop symptoms—usually 2-14 days after infection—the severity of Covid-19 disease can range from mild to life-threatening. Severe COVID-19 is much more common in older people, with those over 65 accounting for roughly half of all COVID-19 hospitalizations.
About 80 percent of people with symptomatic COVID-19 have mild or moderate disease and recover without needing hospital care. The most common symptoms for this group include fever, dry cough and fatigue, and sometimes shortness of breath, headache, rash, and muscle aches. Some people also experience neurological symptoms, especially a loss of taste or smell, or gastrointestinal symptoms such as nausea, vomiting, or diarrhea.
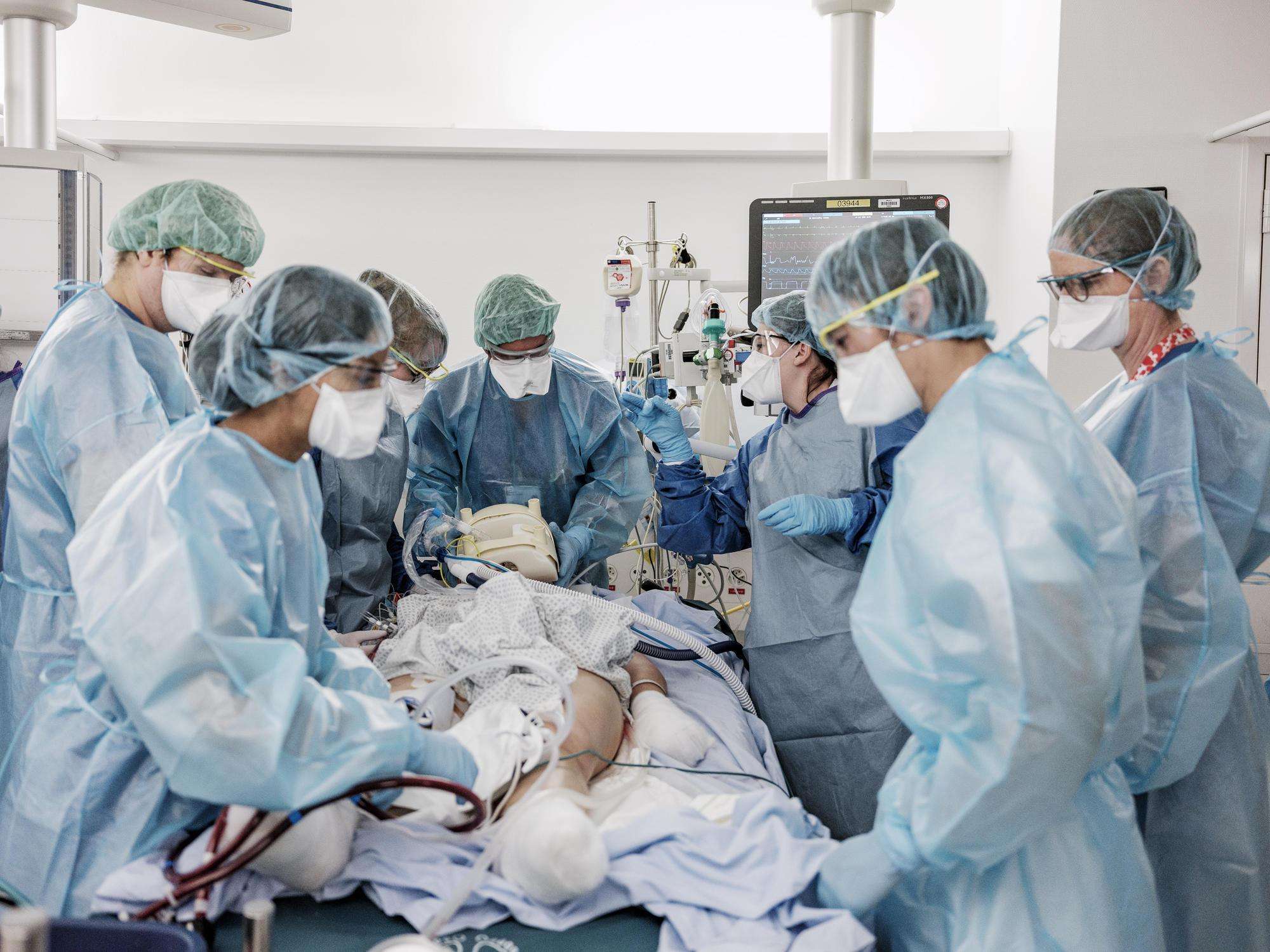
About 20 percent of symptomatic people develop a severe form of COVID-19 characterized by difficulty breathing or pneumonia. These patients require hospitalization and oxygen support, and about 25 percent go on to need intensive care to stave off or treat acute respiratory distress syndrome, a potentially fatal form of lung failure. Beyond its respiratory effects, COVID-19 can damage other organs, including the heart, blood vessels, and kidneys. It can also cause an excessive immune response called a cytokine storm, when the immune system attacks healthy tissue and occasionally leading to multiple organ failure.
While most people with COVID-19 recover within a few weeks or months, many have symptoms that linger for months more. This post-COVID-19 syndrome, also called "long-haul COVID-19," typically involves persistent fatigue, shortness of breath, joint pain, and sometimes problems with memory or concentration (“brain fog”). Long-haul COVID-19 occurs not only in people who had severe disease but also those who had only mild cases or were asymptomatic.
COVID-19 may also have more long-term health impacts, including residual damage to heart muscle and pneumonia-related scar tissue on the lungs. This is still not yet well-understood.