Fighting in Ethiopia’s Tigray region has displaced hundreds of thousands of people. Most of the people who have fled their homes are staying with host families in the region, while tens of thousands of others have taken shelter at informal sites or are still hiding in the bush or the mountains. Doctors Without Borders/Médecins Sans Frontières (MSF) is deeply concerned about the humanitarian situation of hundreds of thousands of people who have been deprived of medical care for months and have received little humanitarian assistance.
A risk of nutritional crisis
Thirty-year old Aster* sits in the waiting area of MSF’s primary health clinic at a site for displaced people in Shire. She is eight months pregnant and has come for a prenatal check-up. She fled with her husband and two young children from a village in West Tigray when fighting broke out in November, and now lives with a local family.
“I have not received any food aid,” she says. “We are getting some food from the people we are staying with, but it is not enough. Sometimes, I go out to beg. If they don’t give me anything, we sometimes sleep without having eaten. It is difficult to be dependent. It makes me empty inside. Before, the children had regular meals.”
Tens of thousands of people have arrived in Shire, a large town in North West Tigray, since fighting broke out in November. Most are from Western Tigray. The majority stay with the host community, but almost 20,000 people live in informal sites. They sleep in cramped and often unhygienic conditions in the classrooms of several schools and on the campus of Shire University.
People’s number one concern is a lack of food. There have been several food distributions so far, and more aid organizations are beginning to arrive, but people say it’s not enough. They also tell us the distributions are often unfair, leaving some people with less than others or even nothing at all. No authority is formally in charge of the sites, and displaced people appoint community representatives from their home areas to organize distributions and other matters. Some people sell food donations to buy blankets or other things they need.
So far, the only food that has been donated so far are bags of wheat and some cooking oil. This means most people in the displacement sites are eating bread every day, which is not nutritious enough, especially for children, pregnant mothers, and sick people.

Sixty-year-old Demsas* has Type 2 diabetes for which he recently received medication from nearby Shire hospital. “The doctor advised me to eat a variety of food—goat meat, milk, injera [flatbread]—but I can’t afford it,” he says. “Before, I was a farmer and a butcher and ate well, but when I came here, we just received some wheat.”
Most shops are now open in Shire and there is food available in the market, but most people have no money to buy it. The city’s civil servants have only recently begun to receive their salaries again since the fighting started, and even those who have money in the bank cannot access it because most banks are still closed. The price of food and other items has gone up as a result, and many of the displaced people did not bring any money.
An MSF nutritional survey of children under five in the sites found that, while the situation is worrisome, it is not yet an emergency. “What we saw was that the overall global malnutrition rate in the sites was about 11 percent,” says MSF medical team leader Juniper Gordon. “There was 9 percent moderate and 2 percent severe malnutrition, which is under the emergency threshold [of 10 percent]. There is food instability and there is definitely a risk for it to become a nutritional crisis. We have to keep a close eye on it.”

Poor conditions contribute to medical problems
Living conditions in the sites are dire. Dozens of people sleep in each of the former classrooms of local schools, between desks and chairs. Some have received mattresses and blankets from the community while many others just sleep on the floor or on plastic sheeting.
With insecurity still ongoing, displaced people continue to arrive in large numbers. Many of the newcomers have no choice but to sleep outside or in makeshift shelters in the sites. Most have fled with few possessions, many just with their clothes on their backs. Some still wear the same clothes they left their homes in more than three months ago. Some women say they had to tear apart their clothing to make sanitary pads, which is a source of humiliation.
On Shire’s university campus, hundreds of people are staying in former student dormitory buildings, sleeping in bunk beds. Those who have not found a place in the dormitories stay in an unfinished building on the campus. Families stack bricks around their sleeping areas to create some semblance of privacy. The air is filled with smoke from fireplaces and the constant sound of people coughing.
In the clinics that MSF has been running in the sites since January, respiratory tract infections are the most common ailment. Is it COVID-19? Nobody knows for sure. There are no tests available, and there is no way for people to keep a safe distance from each other in the overcrowded sites; no way to buy masks or wash their hands frequently. Compared to the many other issues people are facing, COVID-19 is low on the list of people’s worries.
Diarrhea is the second-biggest medical problem due to a lack of clean drinking water and sanitation and unhygienic living conditions. MSF has built latrines in a primary school where displaced people are staying and regularly supplies safe water. Our teams have also rehabilitated a large toilet and shower building on the university campus. Supplying safe water is a challenge in both the sites for displaced people and the whole of Shire town.

“Delivering a baby in these circumstances will be difficult”
The living conditions are particularly hard on pregnant women. Twenty-six-year-old Adiam* fled her village near Humera and now lives in the University site. She is eight months pregnant with her first child
“Delivering a baby in these circumstances will be difficult, but I am glad I am here with my family,” she says. “Many other families have been separated. I want to deliver at the hospital but I am worried what will happen if the baby is born at night, after the curfew. I don’t know how to get to the hospital then.”
After 6:30 p.m. people cannot leave their homes, and while ambulances are in theory allowed to operate, none are available. Until recently, there was also no staff in the hospital after dark, leaving patients on their own during the night. MSF is distributing safe delivery kits to pregnant women in the sites in case they go into labor after dark.
Adonay*, a health care professional from West Tigray who lives in the University site, says he has helped deliver three babies there. “I delivered them inside the dorms, in the women’s beds. There were many people around. There was no privacy. Fortunately, all deliveries went well. At that time, no health centers were open or staffed. We are several health care providers living in this site, and we have been able to help people before MSF and other organizations arrived.”
Patients with chronic diseases are going without medication
Patients with chronic diseases like diabetes or hypertension face some of the biggest challenges. They have not received any medication for months. “In the camps, some patients who have tuberculosis and HIV also have not had medication for months,” says Gordon. “Now, the central pharmacy board in Shire is up and running and they are trying to get medication to the facilities. For some medications like insulin that need [to be kept cold] it is a big challenge—there was no electricity until the beginning of February in Shire, and it is still not reliable. In the majority of regions outside of Shire there is still no electricity.”
Dr. Berhane Tesfamichael is the medical director of Shire hospital. He says the lack of insulin had a severe impact on several of his patients in the period after the fighting started.“Five patients died at the hospital because of a lack of insulin. We sent the patients’ attendants to Adwa and Aksum hospitals. They went on foot; they took the risk to save their relatives’ lives. Unfortunately, there was no insulin available there either. We reported it to the regional health authorities, but the problem was the transport and the security.” Even though insulin recently arrived in Shire’s central pharmacy stock, it is still not possible to distribute it to health facilities and patients in need in the rural areas.
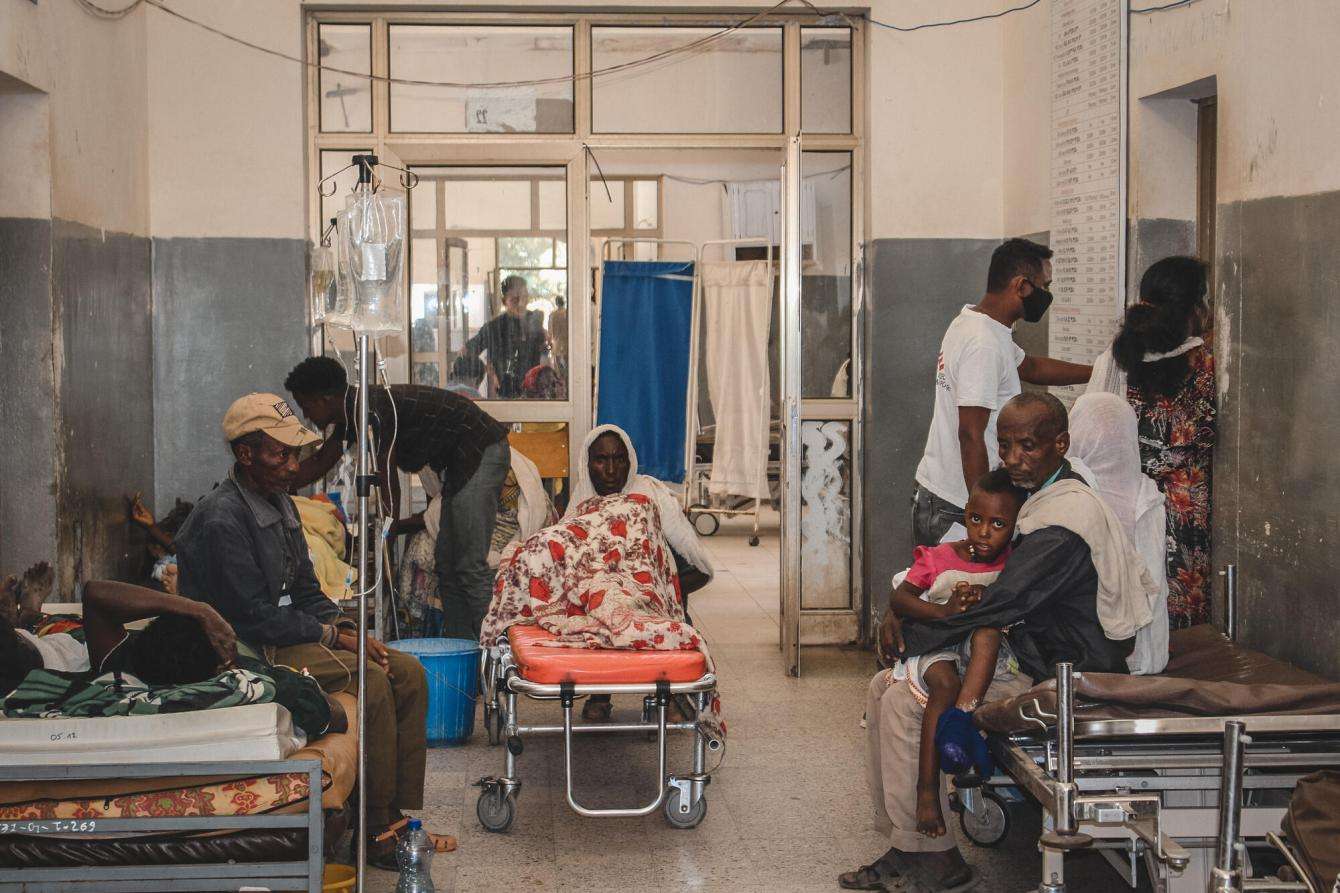
Shire hospital serves a population of more than one million people in the area. After fighting broke out in the city, many staff members did not return to work for a long time, some out of fear for their safety, others because they stopped being paid. Both staff and patients had no food at the beginning, and when MSF arrived, we supplied the hospital kitchen with food and cleaned the facility, as no cleaners had come for weeks. The hospital was not badly looted, but there have been many robberies at night in the past few months because no staff was present. MSF now supports the pediatric ward, the inpatient therapeutic feeding center, and water and waste management activities at the hospital.
Most of the staff has now returned and Shire hospital is almost fully functional. But many issues remain, including a lack of supplies, power cuts, and security issues for patients, especially at night. Apart from the emergency unit, the wards are not busy. Unlike before the crisis, few patients now come to the hospital from rural areas. The referral system has collapsed and the lack of ambulances, widespread insecurity, and high transportation costs to reach the city, many find it impossible to get to the hospital.
Stigma around sexual violence
Dr. Tesfamichael is particularly concerned that few survivors of sexual violence are seeking help. “Many women get raped but they don’t seek help. They want to go to the hospital, but the stigma and social norms prevent them. We have emergency contraceptives, prophylaxis—the problem is, we can’t get to the patients. We need to increase health education, community mobilization, and home visits.”
MSF initially faced a similar situation in our clinics in the sites. Our staff hear many stories about sexual violence from the community, but very few women were coming for care. The number of survivors seeking care is now increasing, possibly because more people are now aware of and trust MSF’s services. From February 15 to 22, 10 survivors of sexual violence received treatment and psychosocial support from our teams.
We offer counseling and psycho-education sessions in the sites. Many people have been deeply traumatized by the violence they have experienced, by their displacement and poor living conditions, and by being separated from family members, often without knowing their whereabouts.
“We all have trouble sleeping,” says 43-year-old Tesfaye*, who lives at the high school site with his family. “We are all thinking about our houses, our businesses, our children who are not going to school. My eldest daughter, who is 14, was one of the best students in her class. She has not been in school for about a year, first because of COVID-19, then because of the fighting. She is very upset.”
The health system in rural areas has collapsed
While the situation for displaced people in Shire is difficult, it is even worse for people living in areas outside of Tigray’s main towns. Birhane* is a 58-year-old farmer who came to MSF’s primary health clinic at the University site. With his weathered face, traditional white headscarf and stooped, thin body perched on a walking stick, he looks much older. He walked two-and-a-half hours from his village to get medical care.
Birhane says that the health center that served his farming community of 2,500 people has been closed since November, and that all six staff have left. “We are suffering from a lack of medical care. We don’t have any medication; the village’s two ambulances were taken. Many people are sick. Three pregnant women have died during childbirth in the past three months,” he says. “There is no food in the village. Our fields have been looted. Some of our women have been raped. We stayed for two months in the forest and we are still scared.”
Berhe*, a health professional working with MSF, says that the region used to have a well-functioning health system before the fighting started. Villages had health posts and there were health centers in smaller and hospitals in bigger towns. Health extension workers visited communities and there was a referral system equipped with ambulances.
“Now, the health structure is completely destroyed,” he says. “When we visit rural areas, mothers say: ‘My child is three months old. He has not been vaccinated yet.’ Maternal and child health is very difficult now. During one of our mobile clinics, we heard that a delivering mother died because she could not get assistance from health professionals. In the rural areas there are no health structures, no ambulances.”
Since the end of January, MSF has been sending mobile medical teams to care for people in villages and towns north, east, and southeast of Shire. We also support some health facilities with medical supplies and recently opened a base in the northwestern town of Sheraro, from which we provide care for people from the surrounding rural areas.
Most of the health facilities our teams have visited are not functional. Many were vandalized and looted and most staff have left. Most people in the region have not received any medical care since November.
As access to towns and villages along the main roads in northern Tigray is getting easier, we are now trying to reach people who are living in the bush, says Gordon. “These are the people who really cannot access any kind of health care. We try to get there and give a bare minimum of care and see their condition. We hear of people who have been in the bush for months and still don’t feel safe enough to go to the clinic.”
*Names changed to protect anonymity.





