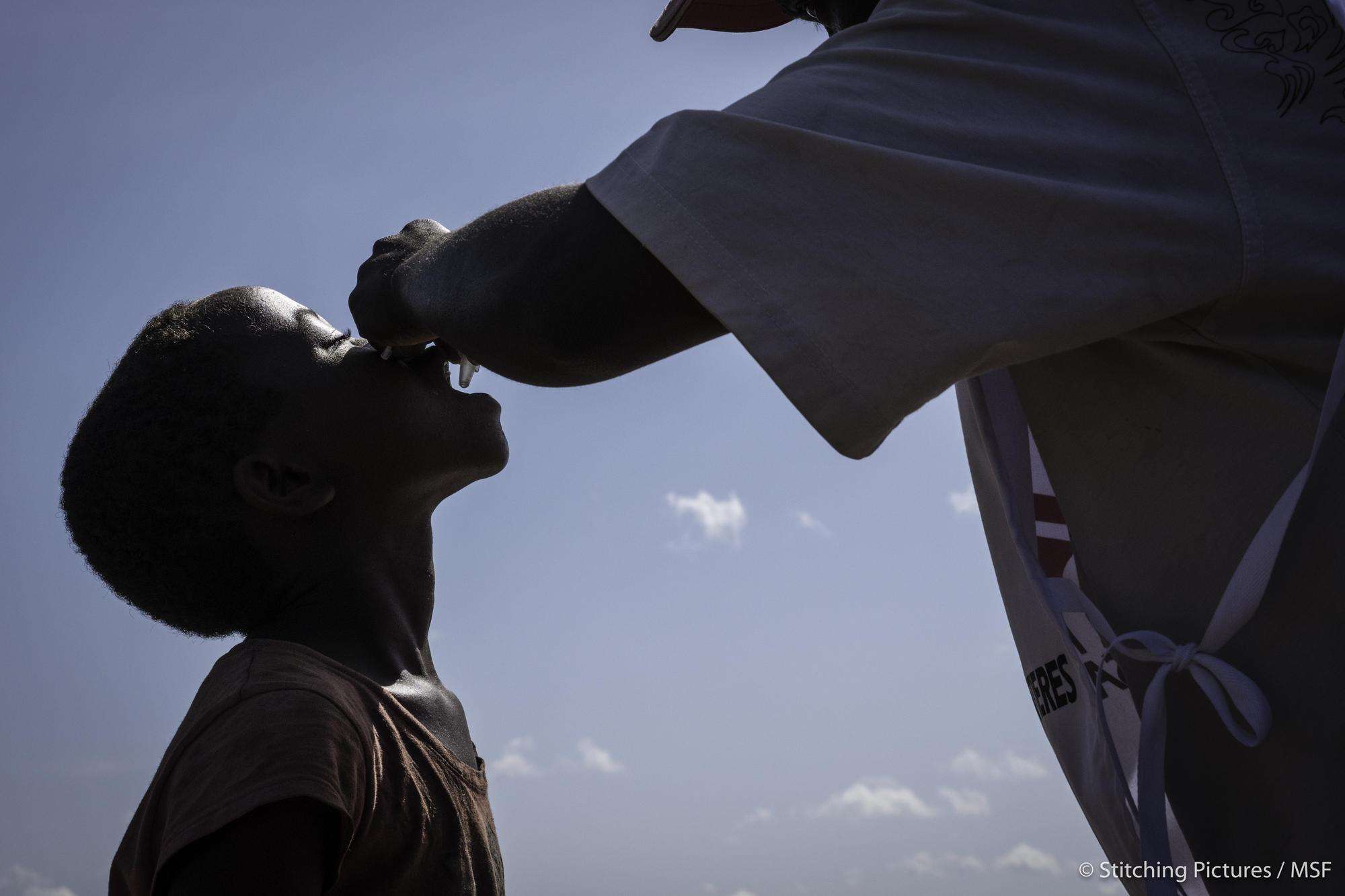
The growth of the anti-vaccine movement in many developed countries—including the US—seems absurd to Myriam Henkens, international medical coordinator for Doctors Without Borders/Médecins Sans Frontières (MSF). Henkens points out that such views are rare among communities in many countries where MSF works. “When you see the disease, you will never forget to get vaccinated,” she said. But in countries where people don’t regularly die from preventable diseases like measles or whooping cough, it can be easy to forget the vital importance of immunization.
During MSF immunization campaigns in response to epidemics, it is common for people to walk for days at a time to get themselves or their children vaccinated because they know the important role vaccines play in keeping them healthy. Preventing disease outbreaks is especially important in places where health care is limited or hard to access. And as the pandemic of coronavirus pushes even the most well-resourced health systems to the brink, the whole world is waiting on a vaccine.
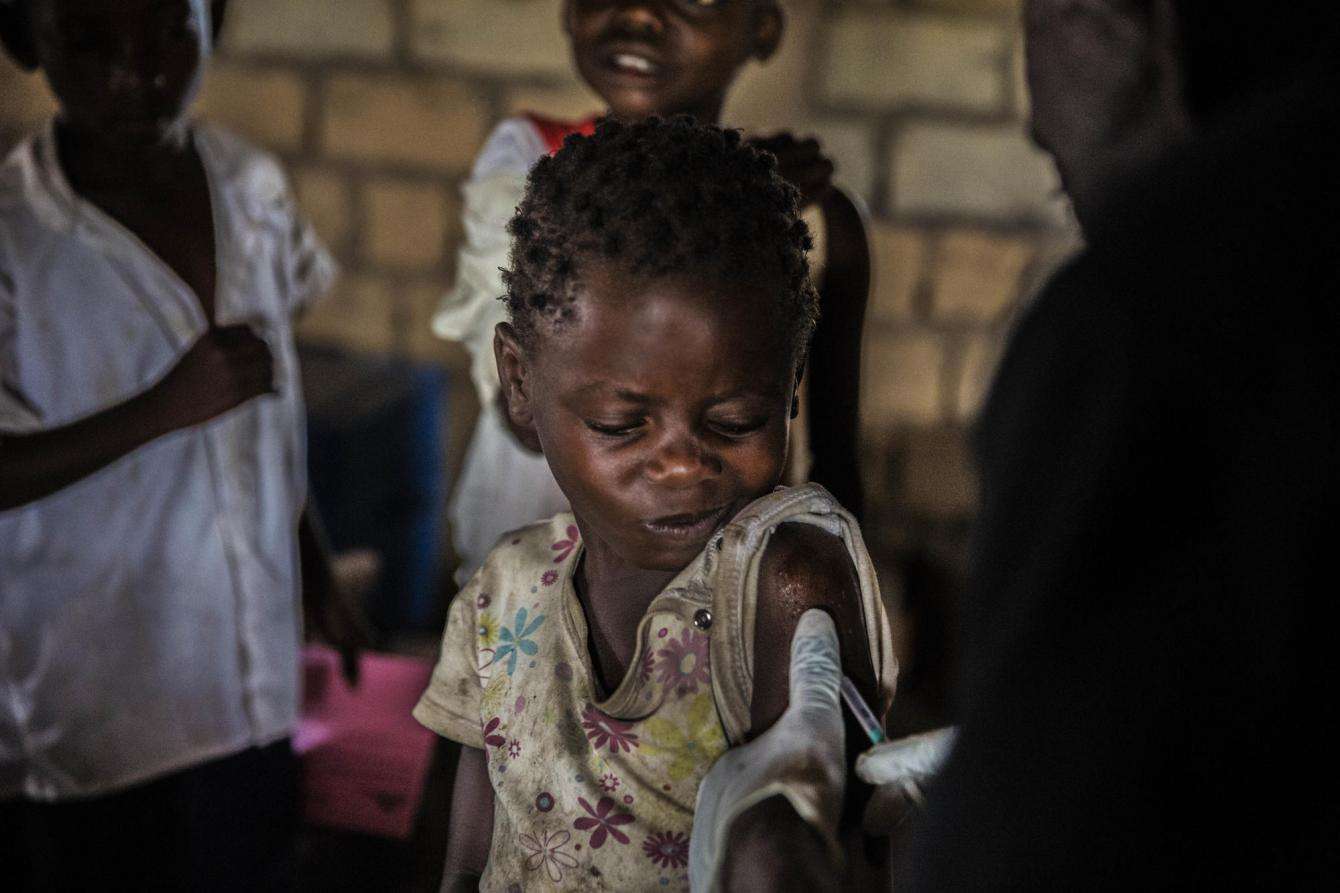
Vaccination can be an emergency response to curb the spread of disease—as is the case right now with measles in the Democratic Republic of Congo, where an epidemic has infected almost 300,000 people and killed more than 6,000 in just over a year.

However, protecting individuals is not the only function of vaccination campaigns. Vaccines can also help to eradicate a disease completely, so people no longer need to be vaccinated.
In 1980, the World Health Organization (WHO) announced the eradication of smallpox worldwide, three years after the last natural case of the disease was registered. It took an additional two decades of worldwide effort to eliminate the disease completely from the map. Smallpox is the first, and only, human disease to be successfully eradicated. Thanks to this, future generations no longer need to be vaccinated against the disease, as there is no risk of being infected.
Though many diseases can now be prevented by vaccines, and some could even potentially be eradicated following the same smallpox model, MSF continues to witness patients—mainly children—dying from them on a daily basis. Even diphtheria—a disease that has been eradicated in most of the world to the point that companies have stopped seeing the need to invest in manufacturing drugs to combat it—has reappeared in countries such as Yemen due to the disruption of routine vaccinations by years of war.
The collapse of public health systems due to conflict is one of the major contributors to disease outbreaks and epidemics. When routine vaccination programs can no longer be guaranteed, diseases that were previously eradicated reappear. And in countries gripped by war, this happens at a time when little or no medical care is available for the epidemic’s victims.
But it is not just wars that impose barriers to routine vaccination. The lack of transport, infrastructure, and electricity can make it very difficult to carry out vaccination campaigns in remote locations. Vaccines usually need to be kept cold in ice boxes or refrigerators to remain effective, which can be a challenge in many of the locations where MSF works. But still, in 2018 alone, our teams managed to vaccinate more than 1.4 million people against measles alone in response to outbreaks of the disease.
There is another huge obstacle to people getting vaccinated: High prices. Pneumonia, for example, kills more children than any other infectious disease, yet it can be easily prevented with the pneumococcal pneumonia vaccine. But for years, this vaccine was inaccessible to millions of children who needed it.
In 2016, MSF’s Access Campaign, which fights to make medicines affordable and available for those who need them most, delivered a petition with more than 400,000 signatures asking the two pharmaceutical companies that produce the vaccine to lower the price to $9 per child for developing countries and humanitarian organizations. While these two companies lowered the price for humanitarian organizations, they can still charge governments high prices even as some have cited those prices as the reason they can’t include the pneumonia vaccine in their standard vaccination package for children.
The world is now feeling the impact of a disease that threatens everyone and has forced us to take unprecedented measures. What will we do if a vaccine for COVID-19 is developed but is sold prices so high that most people can’t afford to benefit from it? How many elderly people, people with pre-existing medical conditions, and health workers will lose their lives before companies and governments put public health before pharmaceutical profits? Governments must be prepared to suspend and override patents and to take other measures, such as price controls, to ensure availability, reduce prices, and save more lives from COVID-19. Companies must also do the right thing and not enforce patents on any new medicines that hit the market for COVID-19 as they stand in the way of generic manufacturers ready to create more affordable versions of medicines.