The availability of affordable rapid tests for HIV and successful antiretrovial (ARV) treatments have made a long, healthy life possible for many. Even so, an estimated 60 percent of people living with HIV are unaware of their status, and those who are diagnosed still face a broad range of challenges to accessing treatment, especially in sub-Saharan Africa.
For World AIDS Day, we’re sharing stories from some of the countries with the highest prevalence of HIV in the world, where Doctors Without Borders/Médecins Sans Frontières (MSF) is working to break stigma and increase access to testing and treatment to communities who would otherwise be cut off from lifesaving care.
Delayed diagnosis or interrupted treatment is devastating for people living with HIV. It leads to increased levels of the virus in their blood, which weakens the immune system and leaves people even more vulnerable to deadly opportunistic infections, such as tuberculosis.
Higher virus levels also put the community at risk, increasing the likelihood of transmission. Across communities where it is common for people to default on their treatment or remain undiagnosed, our teams witness widespread infection that can roll back years of progress made on tackling the epidemic.
HIV can be controlled—it is not a death sentence. When treated correctly, patients can live a long and normal life.
Myanmar
When the Myanmar military seized power from the country’s democratically elected government in a coup on February 1, 2021, doctors and nurses were among the first to protest—walking out on their jobs just days after. The strikes, coupled with widespread insecurity and threats against health care workers, have severely impacted the public health care system, including the National AIDS Program (NAP), which provides medication, consultations, and counseling to more than 150,000 people living with HIV.
The political turmoil has wreaked havoc on Myanmar’s public health care system, and many hospitals have shut down or only offer a limited range of services, which means there are few facilities where we can refer HIV patients when their condition is critical and they need more advanced care than what we can offer.
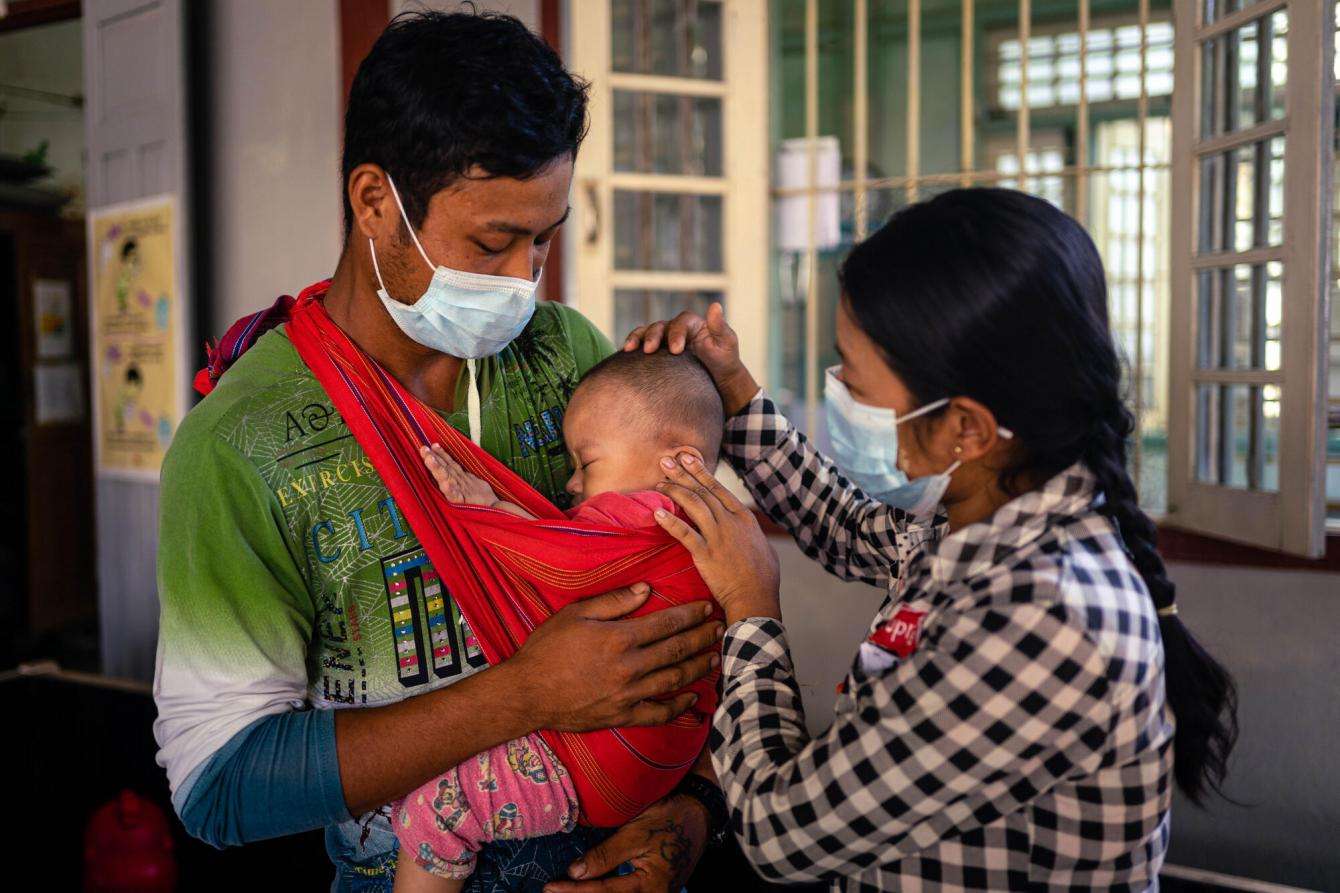
The NAP is slowly recovering, but the facilities that are functioning only offer limited services and are unable to accept patients from MSF into its program—transfers will likely not resume until at least 2023. Instead of downscaling HIV activities this year as initially planned, MSF has scaled up services. We are now diagnosing and starting treatment for hundreds of new patients for the first time since 2019. Our teams have provided 7,200 consultations to NAP patients in Shan, Kachin, and Tanintharyi states.
This spike in patients, alongside interrupted drug imports, has threatened MSF’s medical supplies. For months, we could only offer shorter prescriptions of ARVs—which means people must travel to the clinic more frequently. We are now running low on medications to treat opportunistic infections, such as fungal meningitis, and equipment needed to diagnose HIV in infants. If supply issues are not resolved, many people could die.
At MSF’s clinics in Myanmar, 2,929 appointments were missed between February and October this year—an 89 percent increase from the same period in 2020. Many people visiting our clinics must travel a long way. Not only is there a curfew that makes it difficult for some people to travel, but these journeys are now fraught with challenges that may deter them from making the trip—assassinations, targeted bombings, and battles over territory are commonplace across the country.
“The road between Chipwe and Myitkyina [in Kachin state] has been closed for months,” said Brang Seng*, a patient who was diagnosed with HIV in April. “There are many check points and few drivers dare to come. I am worried about conflict escalating, which would stop me from being able to travel, and then missing my appointment. I can only come when there is a taxi. They are not [available] every day.”
Affordable inter-city trains are not running, and bus routes are not reliable—meaning people have to use more expensive private cars or motorbikes. The economic impact of the political crisis on top of the COVID-19 pandemic means many people cannot afford to get to a clinic. To help overcome these financial barriers, MSF provides these patients with medication via public transport. In Shan state we have made 270 such deliveries since February. But this is not a long-term solution and means that patients who need to see doctor or receive services like blood tests—which can only be done at a clinic—are not getting the care they need.
Democratic Republic of Congo
Nearly half a million people are living with HIV in the Democratic Republic of the Congo (DRC) but access to testing and treatment remains a challenge, causing thousands of preventable deaths—17,000 in 2020 alone. According to the United Nations, almost a quarter of people living with HIV in DRC don’t know they have the virus. Not only does fear and stigma prevent people from getting tested, but access to voluntary testing is almost impossible, and many health facilities do not provide free testing for people with symptoms.
Others stop their treatment because of a lack of available drugs, psychological support to help them stick with treatment, or because of the cost of treatment—even though ARV treatment is supposed to be free. Consequently, many patients develop an advanced stage of the disease.
“I arrived at the hospital in critical condition,” said Sara, a patient at the Luyindu Hospital Center (CHL)—one of six facilities in Kinshasa that MSF supports. “I was hospitalized here for two months. Today, I am back on my feet. I was able to leave the hospital. But I now live in the parish because my family have disowned me. Fortunately, the medical team is here to encourage me and follow my treatment properly.”
“The stigma surrounding HIV in this area is having serious consequences,” said Dr. Adolphe Byakausa Matondo, CHL's medical director. “We did a lot of awareness raising in the hospital and community. Today, fortunately, things have changed a lot.”
According to UNAIDS, between 13,000 and 29,000 new HIV infections occur each year in the DRC, which highlights the need for free and rapid access to testing and treatment to avoid developing potentially fatal complications. But there is still a lack of national and international resources to make this possible.
Mozambique
Mozambique has one of the highest HIV burdens in the world. In Beira, a port city on the east coast of the country, 4,390 people tested positive for HIV in 2019, and 2,766 in 2020. Unfortunately, stigma makes it difficult to convince patients to start treatment. As a result, MSF’s teams treat many people with advanced HIV (commonly known as AIDS).
“Our main aim is to recognize cases in advance by screening patients and to clinically manage these patients in the early stages in order to reduce the mortality rate,” said MSF’s Dr. Shehezady Cruz. “It’s important that patients know that HIV/AIDS can be treated and that it’s possible to lead a normal life—as long as the treatment is followed.”
However, people face many challenges in accessing or staying on treatment, including socio-economic barriers, lack of family support, access to a balanced diet, living far from health services, and stigma. MSF addresses these challenges by providing psychosocial support, following up with patients with serious illnesses, and providing outpatient consultations and referrals in collaboration with the local health centers.
“Every month, like clockwork, [the MSF staff] would call me to check on my treatment,” said Santos Estrela*, who is receiving treatment for advanced HIV from MSF in Biera. “The counselors, the nurses, and the clinical care I received motivated me to keep going. I felt that I mattered.”
Estrela was diagnosed with HIV more than five years ago after his wife fell ill. She was diagnosed with meningitis and HIV and died shortly after. “I became depressed,” said Estrela. “I started drinking and smoking. I didn’t tell my family I had HIV and I didn’t follow the treatment. And it made my condition worse.”
In 2020, Estrela was admitted to Beira’s Central hospital. After starting treatment, he got better. “At that point, my family members found out I had HIV and supported me to continue following the antiretroviral treatment. The support I received from my family members and those closest to me helped to improve my situation. My family made sure I had good, nutritious food to keep me healthy. I felt strong. It was a strength that came from within, and it motivated me to fight.”
* Name changed for privacy.

