Nogood Mohammad Ahmed Shamsan was lying under the covers of her bed, exhausted. She rested her left hand on her belly as she drew long, slow breaths. Her mother sat beside her, making sure that her daughter was comfortable and tending to her needs. Under Nogood’s right arm, one-day-old Ahmed slept, nestled in blankets.
Nogood was admitted to the post-operative ward after delivering Ahmed through caesarean section at the maternity unit in the Al-Jamhouri hospital, in Taiz city, Yemen. Doctors Without Borders/Médecins Sans Frontières (MSF) and the ministry of health have been running maternal and neonatal services in the hospital together since May 2021. MSF provides technical support, financial incentives to the ministry of health’s staff, and medical and logistical supplies to run the maternity unit including services such as caesarean sections, prenatal and postnatal care, family planning, vaccination, and neonatal care. After MSF began supporting the maternity unit, between August 2021 and August 2022, the neonatal mortality rate reduced from approximately 24 percent to 10 percent. Prenatal and postnatal consultations also increased.
A health system on the brink
More than eight years of war in Yemen have taken a devastating toll on people in many ways, including inhibiting access to quality and timely health care. Fewer than 50 percent of health care structures in the country are functioning. Most primary health care centers are only partially functioning due to a lack of equipment, medical supplies, or medical staff. Since 2016, health care workers haven’t received a regular salary, forcing many to find alternative employment to make a living. Women often must travel far to reachfree health care services.
“I come from Bani Oman, a village,” said Nogood. “My financial situation is not that good, so I came to Al Jamhouri hospital to have my caesarean section, because it is free-of-charge. There is only one health center in the village, but there is no necessary equipment there.”
Accessing proper care at Al-Jamhouri hospital is a harrowing journey for many. Taiz is still divided in two: Taiz city—controlled by the administration of the internationally recognized government of Yemen—and the suburb of the city Al-Houban—which is in the Ansar Allah-controlled part of Taiz governorate. The front line that runs through the city is littered with landmines and guarded by snipers.
To reach Taiz city, people must make the long, perilous trek through the mountains to avoid crossing the front lines. Prior to the conflict, it took 10 minutes to reach Taiz city from Al-Houban—now it can take five to eight hours to get there. This is the route many people have to take to reach free, quality health care at the MSF-supported Al Jamhouri hospital.

“We live on a mountain, so after the rain the road becomes worse and worse,” said Bushra Khaleed Abdualrahman,* who is eight months pregnant. Abdualrahman’s brother brought her to the hospital for emergency medical care from the Sabr Al Shaqeb area. “I was in pain and due to the arduous journey, I became so unwell.”
Pregnant women living in rural areas come to the hospital with high-risk or complicated pregnancies, conditions that could have been avoided with consistent prenatal and postnatal monitoring. But this basic care is nearly impossible to access when local facilities lack services or the necessary medical specialties and basic equipment, like ultrasound machines, to perform the necessary monitoring. Between August 2021 and August 2022, MSF’s team in Al Jamhouri hospital assisted 6,739 deliveries, out of which 4,184 were normal deliveries. Almost 29 percent required caesarean sections—an indication of the high number of complex pregnancies arriving to the hospital.
“The first time that I had pain I went to a doctor in my area, and they just gave me first aid,” said Abdualrahman. “There is no equipment and no machines so that’s the only thing they were able to do.”

The importance of community health promotion
According to Mduduzi Chandawila, MSF's medical team leader in Taiz city, most of the women that come to Al Jamhouri hospital from remote locations have rarely attended prenatal care consultations. “It’s a challenge,” said Chandawila. “Some of the high-risk pregnancies that come to Al Jumhouri hospital are coming for the first time. Some of them are already in their eighth or ninth month of pregnancy.”
“Most of the women that are seen attending our services, for prenatal care, for example, are presenting late or they are patients that are at high-risk pregnancies” said Chandawila. “These are women that have had some surgery before, like a Caesarean section, some that have done the procedure two or three times. Others arrive with pre-conditions like eclampsia or pre-eclampsia—serious complications that need to be monitored closely and we need to carefully tend to patients that will not do normal delivery.”
MSF provides health promotion to spread awareness about the importance of prenatal and postnatal care. An MSF health promotion team shares information in the waiting areas of the maternity ward while and conducts broader community outreach.
“Through prenatal care, health conditions can be identified early in terms of the way to deliver or the mode of delivery, what support they need, and what medication or treatment they need before they deliver,” said Chandawila.
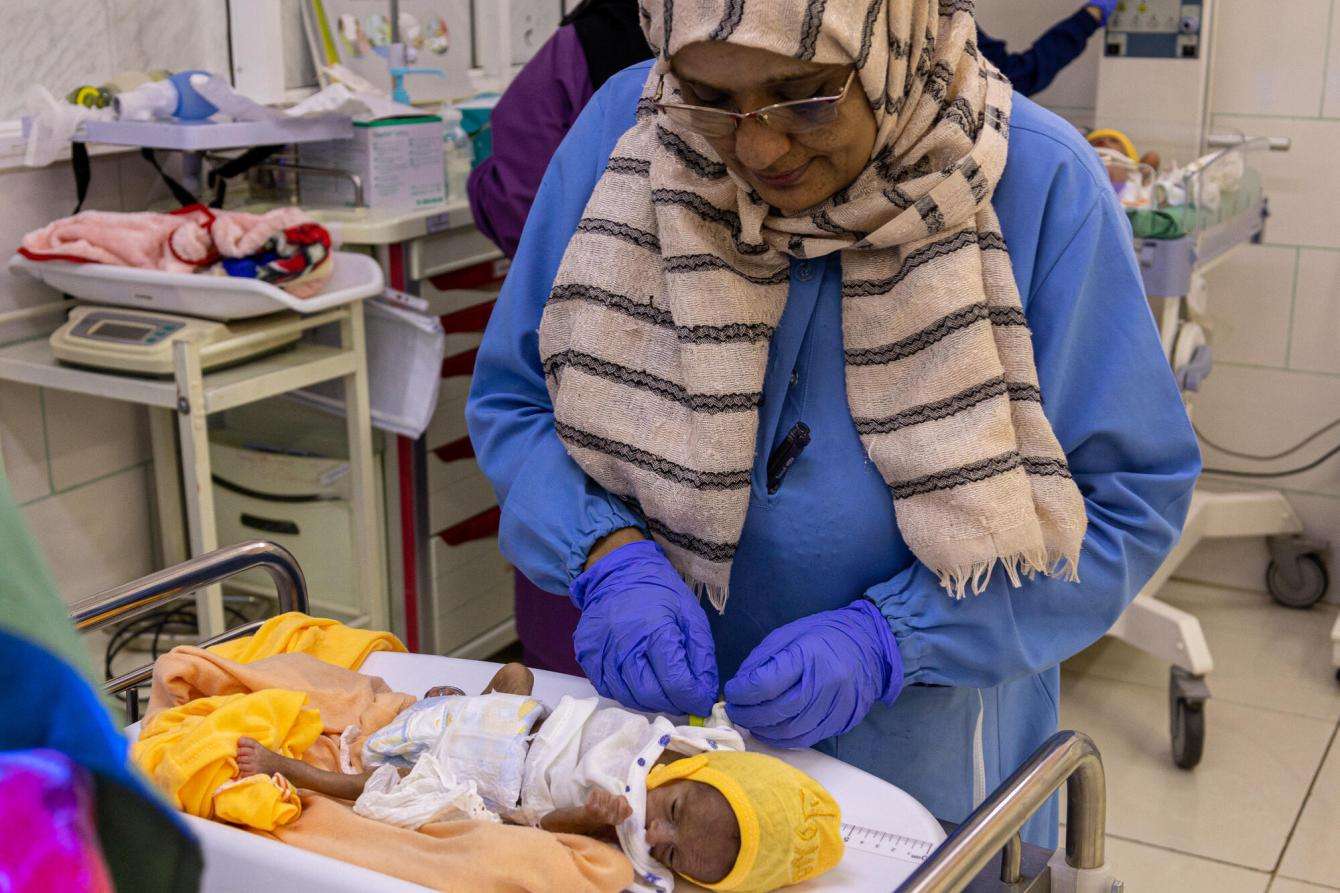
“Postnatal care is also very important so that we can monitor the progress of the post-delivery period, we can monitor the surgical side, infections and other complications that may develop.”
The maternity unit at Al-Jamhouri hospital assists approximately 520 deliveries per month. In August 2021, MSF in Al-Jamhouri hospital conducted 1,364 prenatal consultations and 86 postnatal consultations, whereas in August 2022 it remarkably rose to 1,795 prenatal consultations and 527 postnatal consultations.
While these numbers are encouraging, gaps remain. Timely access to primary health care is vital but remains a challenge, especially for pregnant women who should be consistently monitored from the beginning of their pregnancies to avoid medical complications for them and their babies’ and to prevent maternal and neonatal deaths.
*Name changed to protect anonymity





