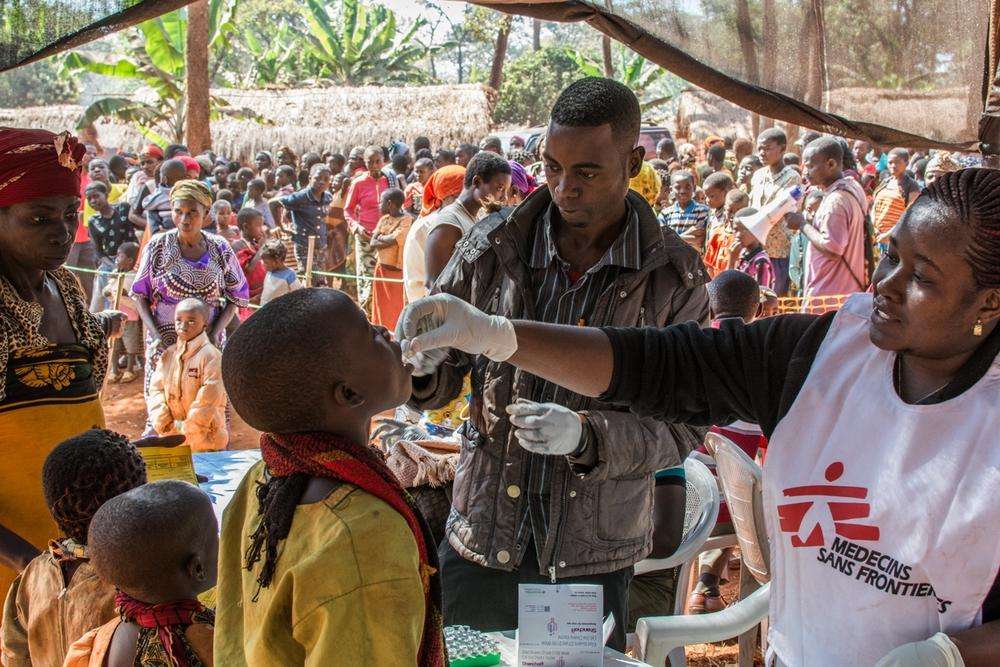
Erwan Rogard/MSF
Cholera
Cholera is preventable and easily treated, yet it infects millions of people each year and causes up to 143,000 deaths worldwide.
Global cholera vaccine stockpile runs empty as 16 countries report outbreaks
February 26, 2024—Doctors Without Borders/Médecins Sans Frontières (MSF) is extremely concerned about a recent announcement that the global cholera vaccine stockpile has been exhausted, at a time when there is very little capacity to manufacture more vaccines. As a high number of countries are reporting outbreaks, more manufacturers—existing and new—must urgently help boost the global supply.
Read more
Putting cholera in context
Cholera is a highly contagious disease that occurs in settings without clean water and proper sanitation—from poor, remote villages to overcrowded cities, refugee camps, and conflict zones. It causes profuse diarrhea and vomiting, and without treatment can quickly lead to death by intense dehydration. In recent years we responded to dozens of outbreaks, including massive epidemics in post-earthquake Haiti and war-torn Yemen.
patients treated by MSF
for cholera in 2022
cholera patients admitted
in 2022 to MSF facilities in Haiti
people immunized in 2022
by MSF staff in Lebanon
Facts about cholera
Cholera is a bacterial infection that causes cells lining the intestine to produce large amounts of fluid. It spreads when someone ingests food or water contaminated with vomit or feces from a person carrying the disease. Contaminated food or water supplies can rapidly cause massive outbreaks.
Cholera symptoms typically appear within 2-3 days of infection and vary widely, from mild to severe. In severe cases, people have profuse watery diarrhea, vomiting, and leg cramps, leading to dehydration and shock that can become fatal within hours if patients don't receive care.
Drinking and using safe water, using clean latrines or toilets, washing hands with soap, and ensuring good food hygiene are all ways to avoid the disease–but are often difficult or impossible for individuals in settings where cholera occurs. Prevention and control require measures at the community level, especially in making communally-supplied water safe for drinking.
Oral vaccines are another powerful tool being used more and more to help prevent cholera and to contain outbreaks. But vaccination alone cannot end cholera–improvements in sanitation and hygiene systems are also essential. Protection with current vaccines may not last beyond 3-5 years, and despite recent increases in vaccine production, the global supply still falls short of meeting today’s needs.
Definitive cholera diagnosis requires a laboratory test. For field settings without access to lab facilities there are rapid tests available, but they are less reliable. Declaration of an outbreak therefore requires laboratory confirmation. Diagnosis of individual patients during outbreaks is typically made without these tests, based on a patient history and symptoms and on clinical examination.
Most cases of cholera are simple to treat, and treatment is highly effective if patients receive it promptly. Mild and moderate cases of cholera are treated by having patients drink large amounts of oral rehydration solution—a mixture of sugars and salts in water. The sickest patients may need intravenous fluids and antibiotics. Without treatment, patients may die within hours, but with proper care the death rate usually drops to 2% or less.

How MSF responds to cholera
At MSF we started responding to cholera epidemics in the 1980s, and are gradually working to improve the effectiveness of our response. More recently one of our larger responses was in Haiti, where a cholera epidemic that began shortly after the devastating 2010 earthquake has so far caused over 800,000 cases and nearly 10,000 deaths. Thankfully there have been no new cases since February 2019, thanks to years of intensive efforts by Haitian health authorities and international organizations. Among our current projects, we are active in Yemen, which continues to face the world's largest cholera epidemic since modern record-keeping began in 1949. Amid ongoing full-scale war that caused the country's infrastructure and health care system to collapse, over 2 million people in Yemen have suffered from cholera since the outbreak's start in 2016.

Everything you need to know about cholera
People should not be dying of cholera in 2024. We need to act quickly to prevent more deaths.
More news and stories
Learn about MSF’s journalistic roots and our commitment to bear witness and speak out about the plight of the people we treat.

News Oct 24, 2022
Increased aid and vaccinations needed for refugees in Kenya's Dadaab c...
Read More
News Oct 19, 2022
MSF responds to change in global cholera vaccine strategy amid unprece...
Read MoreLearn about MSF’s journalistic roots and our commitment to bear witness and speak out about the plight of the people we treat.




