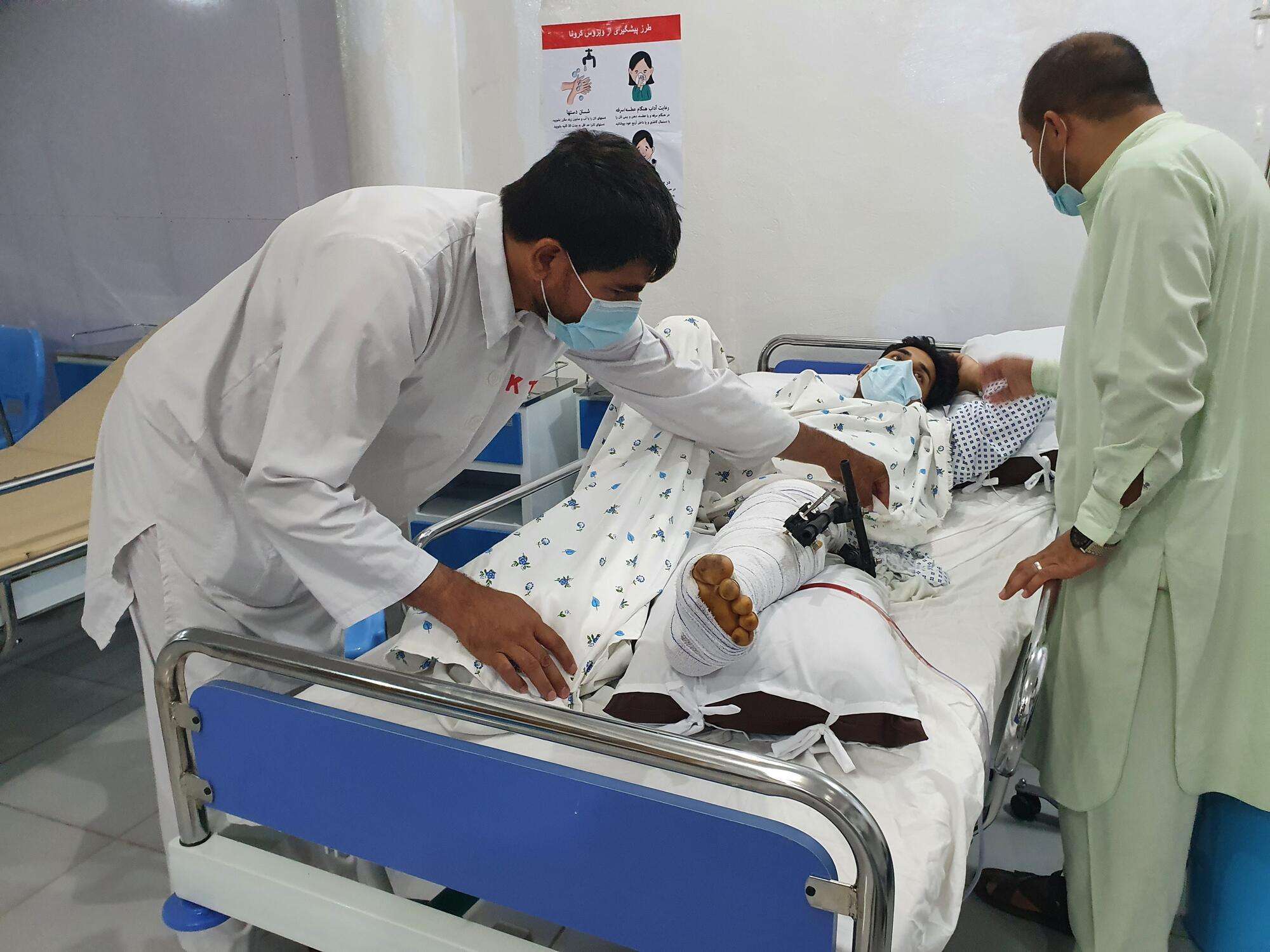
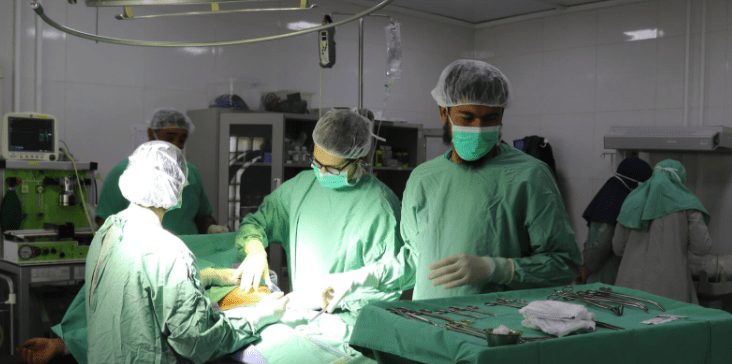
In 2015, the Doctors Without Borders/Médecins Sans Frontières (MSF) hospital in Kunduz, Afghanistan, was destroyed by US airstrikes. Forty-two people were killed, including patients, MSF staff, and caretakers. For the last few years, we have been working to rebuild a new trauma center in the city, even amid escalating conflict between the Islamic Emirate of Afghanistan (also known as the Taliban) and Afghan government forces.
During the intense clashes last month, MSF transformed its Kunduz office space into a temporary trauma unit to care for wounded people. On August 16, these patients were transferred to the nearly-finished Kunduz Trauma Center. This facility will employ 300 Afghans when it is fully operational, including staff members who survived the initial US attack six years ago. Many local people still need significant trauma care. Here, a medic on MSF’s Kunduz team describes his experience during the recent fighting and the work that is taking place now.
Today it is busy but calm. We’re recruiting new staff, and the final steps of the construction process are taking place all around us.
The first evening we opened, there was continuous bombardment and shooting. We had to rush to the bunker, and we stayed there all night, without any sleep. Patients were not able to reach the trauma unit at that stage, on account of the non-stop fighting in the streets.
The following morning, we got news of multiple victims arriving in the unit, but we could not get there because there was fighting in the street between where I was staying and the unit. Our colleagues were asking for our help very urgently, because they had a patient who had gunshot wounds in his chest and stomach that required immediate surgery.
A moment came when the guns were finally quieter, and it was possible to move. Three of us ran to the other side of the road to the operating theater. The patient had just lost his pulse, so we started chest compressions while the anesthesiologist looked for an airway.
I cut two holes in the chest to make sure blood could drain out and to allow the lungs to expand. Meanwhile, another colleague was trying to stop the bleeding below the sternum. We could tell pretty quickly that the bullet had probably hit part of the heart, and it rapidly became clear that there was no way that we could save him.
Hard days
That was the start of our day of hell. And the first moment of our team being completely overwhelmed. There were a lot of other victims who came in and had to go to surgery: many had gunshot wounds, others were injured by bomb blasts or were caught in the crossfire.
Much of our staff could not reach the trauma unit. The night-shift staff worked through the day. Some would take naps and sleep while others worked so we could keep staff going from morning and into the night.
At about 6:30 a.m. the next morning, an ER doctor called me on the radio, saying “I need your help now.” As the fighting receded, I ran with the surgeon across the road. The hospital unit was crammed.
Four patients urgently needed emergency surgery, all at the same time. We started doing lifesaving surgery on two patients while also doing everything possible to keep the other two alive. We eventually proceeded to operate on them too. In the end, one patient died, but three survived, which is quite remarkable—they all had very severe gunshot wounds and bomb blast injuries. While waiting for space to open up in the operating theater, and trying to keep the other two alive in the emergency room, we still needed to assist other patients who had come in and needed care.
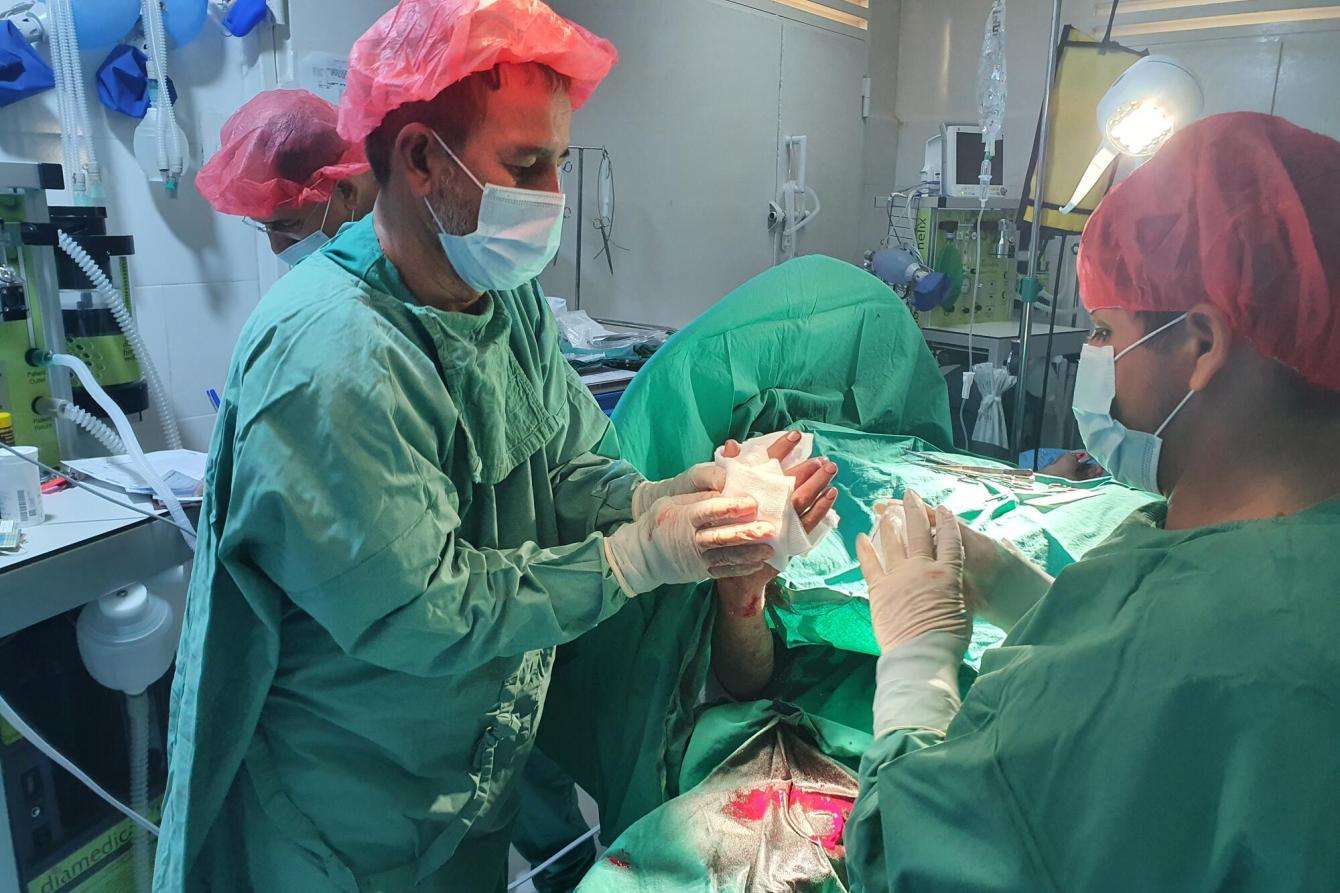
An unexpected case
One of our patients was a young boy. He was brought in to the ER by his father with a bandage already on his arm. He wasn’t crying and was just silently looking ahead. I was supervising the ER along with the Intensive Care Unit nurse. The boy looked comfortable and very much okay. There seemed to be no immediate urgency.
Because the fingers sticking out of the bandage looked well circulated and warm, I took my time in demonstrating to the staff how to do a proper investigation of the hand for nerve damage. Strangely enough the boy didn’t seem to feel anything on his whole hand, which suggested all three different nerves were cut.
I gently unwrapped the bandage and saw a gaping hole in his forearm. There was more hole than actual tissue! The father told me that a stray bullet had hit the child while he was playing.
Their expressions on the staff’s faces said: Well, I didn’t expect that! Nor had I. So, we packed up the wound again and tried to stabilize the hand. The only salvaged part was the artery going all the way to the fingers, but the nerves were all damaged.
Medically, we all agreed that amputation was probably the best option. The father didn’t agree with this. He wanted to give it a chance. We did our best to clean the wound and keep the tissue alive. We attached an external fixator, a metal bracket to hold the bones in place while mending, to try and let it heal for as long as possible. Up until today, the boy’s hand is still there. He will never have a good hand again, that’s for sure. But the hand is still there and we didn’t expect that.
The father has been very friendly, but the little boy knows that if a doctor is coming close, that means there is going to be pain. He hasn’t smiled at any of us, but we see him smiling at his father.
Doing all we can
After the fighting lessened, we began to see more patients coming in. Many of them had already received some sort of emergency treatment. When they got injured, they went to the nearest hospital they could to be taken care of and the staff there did what they could.

We are seeing an increase of patients being referred to us from provincial hospitals, where patients had multiple surgeries. Quite often we go into surgery and realize that we don’t have too many options—there is not much more we can do to try to save the person. We still try though; try to stabilize; try to get things in order with some surgery.
Moving to the new hospital
Here in Kunduz, the rebuilding of our hospital has been going on for quite a while. The community has been waiting for the hospital to open. Two weeks ago, we transferred the patients from our temporary clinic to the hospital for the first time. It is a huge step to open the new hospital, although it is not completely finished yet.
We’re seeing a shift from the very active gunshot and bomb blast injuries to complications with the war-wounded who need follow-up from previous treatments. We’re also seeing more road traffic accidents, which are increasing sharply as society opens up again. Everyone here drives on their motorcycles without a helmet; when they fall, they suffer head traumas, which is not the best thing for us to treat as we don’t have neurosurgeons, so sometimes there is little we can do.
Making it work
In the Kunduz Trauma Center we’re doing our medical work while construction is still going on. But the speed at which all the construction teams and others are fixing things is quite amazing. They have a real approach to solving problems.
We saw a stretcher bearer going to get a patient and having problems passing the stretcher over the uneven ground because there was too much rubble. In no time, there were people putting concrete over the rubble. It’s incredible how the crew is working so hard to fix all the problems the medical staff encounter.
We have the same support from the team that is responsible for the hospital compound. One of them is always on a bicycle, cycling from one department to the other, fixing things rapidly. Same for supply fixes—you see medical items and supplies suddenly appear at the front step of the departments, followed by other packages for us to treat our patients.
We’re also increasing our recruitment efforts. We have ongoing exams for staff, and we’re hoping to start recruiting mental health officers, which is something that we badly need.
That’s how it feels for the moment—all the teams are helping each other, together, trying to just make it work.