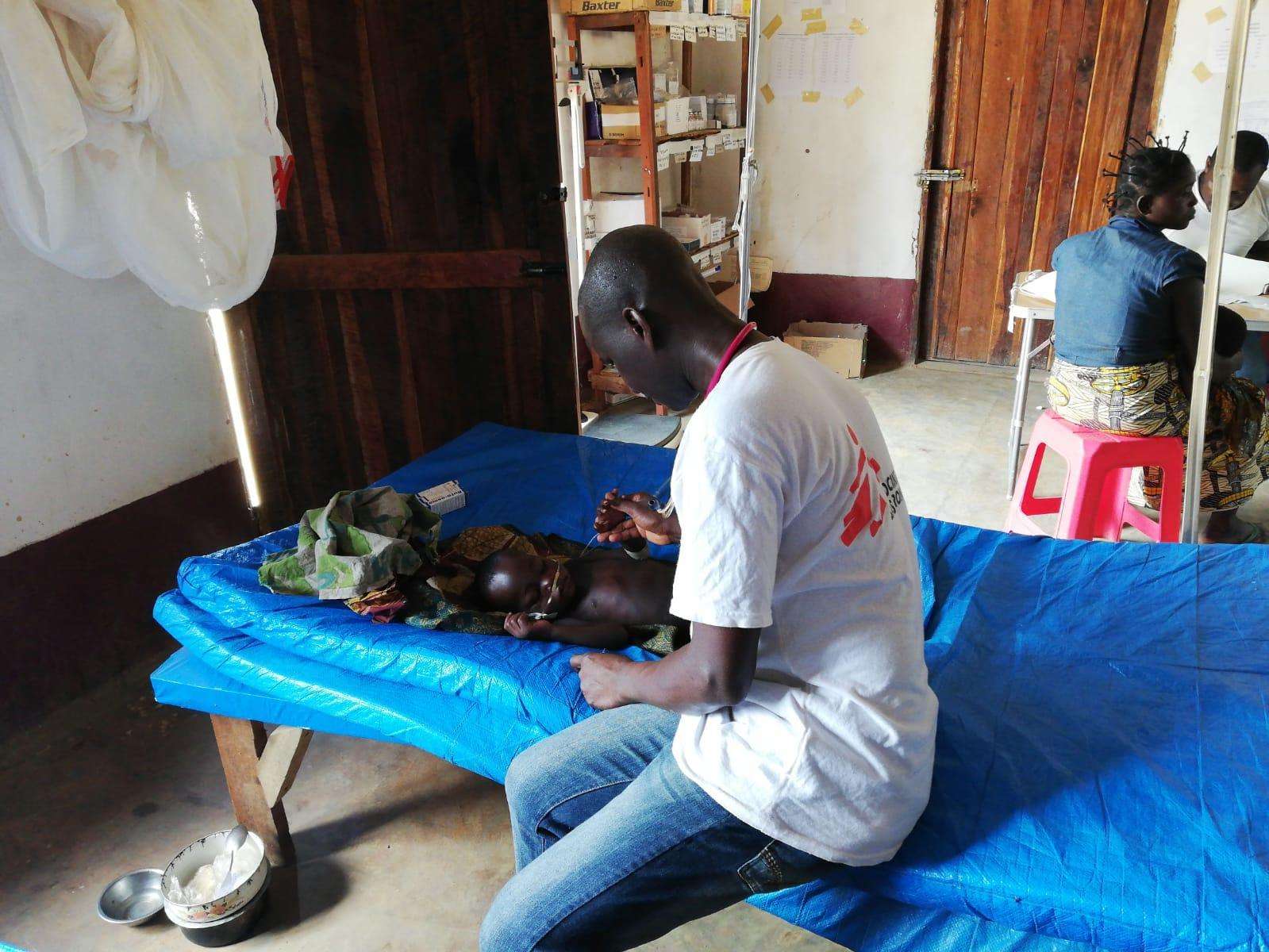
Doctors Without Borders/Médecins Sans Frontières (MSF) emergency operations coordinator Dr. Natalie Roberts describes the challenges of responding to the measles epidemic currently affecting the Katanga region in southeastern Democratic Republic of Congo (DRC). Measles, a highly contagious viral disease, is one of the leading causes of death among young children worldwide.
What is the situation in Katanga?
A measles epidemic was declared in March 2018 in the provinces of Haut-Katanga, Haut-Lomami, Lualaba, and Tanganyika, which together previously formed the province of Katanga. The epidemic spread over the course of the year and, by December, every health zone across the four provinces had declared either suspected or confirmed cases. Moreover there are enormous pre-existing health needs throughout the Katanga region—an area the size of Spain—where people are scattered across remote villages.
Since 2011, Katanga has had a large-scale measles epidemic every two or three years. The Ministry of Health faces the same constraints that we do: a lack of supplies in the health zones because of the difficulties of transportation, a lack of electricity for vaccine refrigerators, and difficulties in reaching communities. Routine vaccination coverage is therefore inadequate in many locations, and epidemics are recurrent. MSF has regularly carried out emergency measles vaccination campaigns in the region. Although our goal is to respond early in the epidemic, we still often fail to meet this objective due to the challenges we face. We are constantly trying to find new or different solutions to this recurrent problem.
How does MSF respond to a measles epidemic on this scale?
Measles epidemics take hold in areas where not enough people have been vaccinated. To protect a population, 90 to 95 percent of people—and ideally 100 percent—must be vaccinated.
By vaccinating populations as soon as measles cases are reported, we aim to prevent children in the area from contracting measles and to stop the spread of the disease. To have the greatest impact through mass vaccination, we need to target areas where the epidemic has just begun, as we are now doing in Lualaba province. But sometimes it’s already too late and this isn’t possible.
In areas which have already experienced a major epidemic over several months, a mass vaccination campaign is not necessarily the most appropriate response. Even detecting the epidemic early enough is difficult, as the only validated laboratory in the country is in the capital, Kinshasa.

Then the delivery of vaccines and other supplies to these remote locations can be massively time-consuming and complex. When the disease has already taken hold in a community, mass vaccination alone has limited impact—the vaccine is not a treatment for children already suffering from measles. However, if an effort is made to access these areas, sick children can be treated as soon as they are identified. Even when a measles epidemic is already widespread, we can still save lives by treating children suffering from measles and other diseases by isolating patients and treating complications from the disease.
Why does measles have such a high mortality rate among children?
Measles infection puts children at a high risk of developing other serious illnesses, such as severe malnutrition or respiratory tract infections, while children in this region also frequently suffer from malaria. It is very difficult to ensure that children in remote areas can access the necessary basic health care—which is why they arrive very late to hospitals.
We suspect that many children in this region never get medical care and never get vaccinated. Information from local communities suggests the mortality rate of children under five is extremely high in certain areas of Haut-Lomami Province, where their deaths are not always reported.
What is the status of efforts to contain the epidemic?
In March [2018] MSF began its response in Haut-Katanga province. By September, MSF teams had vaccinated 231,646 children and treated 3,334 measles cases in different areas. Then MSF deployed significant resources in Haut-Lomami province, primarily in the health zones most affected by the ongoing epidemic. In collaboration with local Ministry of Health staff, we treated 393 children with severe measles in local hospitals and 2,957 milder cases in outpatient health centers from December 2018 to February 2019. We also vaccinated 64,629 children in Malemba-Nkulu (Haut-Lomami), and continue to vaccinate in other areas.

Our priority is to use mobile clinics to try to reach children living in the most severely affected areas, with the aim of treating them in their local communities and vaccinating those previously not vaccinated. But we face huge logistical constraints. Paved roads don’t exist in the region and travel can be extremely difficult, particularly in the rainy season. It can take days to move between different areas, even in four-wheel drive vehicles. To reach more remote locations, we must use motorbikes and even canoes, which makes it impossible to transport large quantities of medicines, vaccines, or therapeutic food to treat malnutrition."
In November and December 2018, MSF ran a preventive mass vaccination campaign against measles in Kamonia health zone (Kasaï Province) and vaccinated more than 42,600 children. Last year, MSF also vaccinated 461,611 children and treated 10,736 children in the provinces of Tshopo, Maniema, and Ituri, and has supported the Ministry of Health in responding to measles epidemics affecting the regions of Kivu and Maniema. Other operations are planned in Tshopo, Ituri, and Haut-Uélé.
In addition to measles intervention, MSF is also responding to a cholera outbreak in Lubumbashi. More than 2,100 cases of cholera have now been recorded in the city, where MSF is supporting the Ministry of Health in treating patients, ensuring access to oral rehydration treatment in the community, and reinforcing water supplies, sanitation, and household hygiene in the most at-risk areas of the city.
In North Kivu Province, MSF is responding to DRC’s largest ever Ebola outbreak. In collaboration with the Ministry of Health, our teams are caring for patients, reinforcing infection prevention and control protocol, and vaccinating frontline medical staff, among other activities.