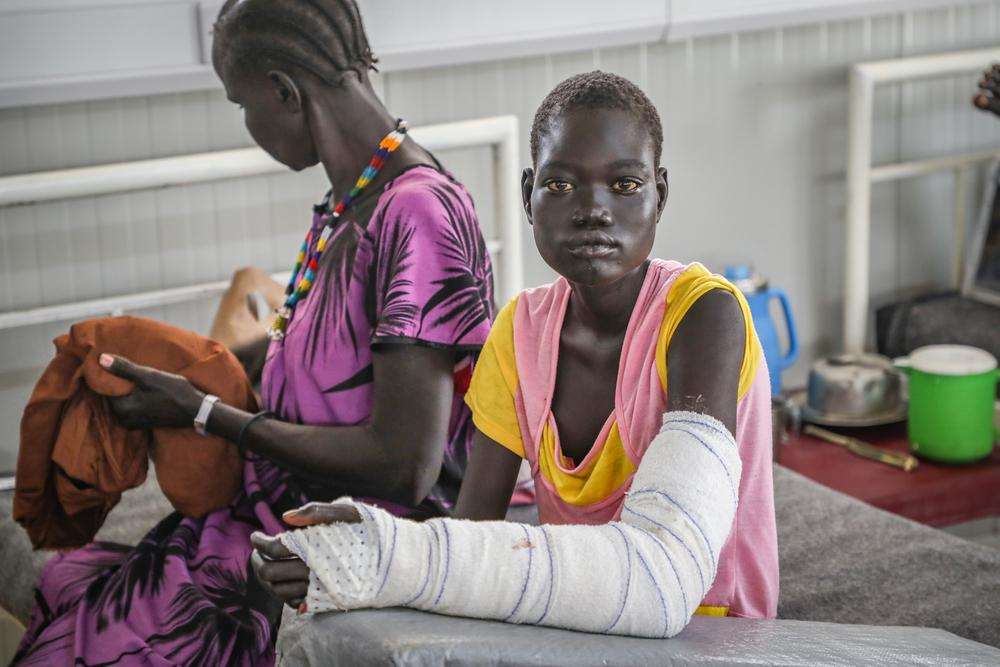
For the nineteenth time, 10-year old Awien is being taken into the operating theater. Her right arm, damaged beyond repair, hangs limply in a sling around her neck. But at least she still has it. And, most importantly, she is still alive.
Two months ago, Awien was bitten by a snake as she slept at night. Like many other snakebite victims across sub-Saharan Africa, reaching medical treatment in time is not easy. She lives in a small village in South Sudan, far from the nearest road and even farther from the nearest hospital.
In rural areas like this, people’s first reaction to a snakebite is usually to treat it with traditional remedies. Awien’s family tried several: a frog was cut in two and put on the bite to remove the venom; she was given raw egg to drink, and then a mixture of seeds and leaves to make her vomit so as to get the venom out of her body. None of these remedies helped, so her uncle decided to carry her on his back to the nearest hospital. It took him a whole night to walk to Agok, where Doctors Without Borders/Médecins Sans Frontières (MSF) runs the only hospital in the region.
A big problem with few solutions
In Agok, MSF treats around 300 snakebite victims each year, most during the rainy season when snakebites are most common. To escape the water, snakes often enter people’s houses, which is where about half of victims are bitten. Children playing outside and people working in fields are also at risk. But wherever they are bitten, everyone has the same problem: how to get treatment?
Most snakebite victims live in remote areas and have to travel long distances to seek care. During the rainy season, when roads in South Sudan can become impassable, people may have to travel for several days to reach a hospital.
In the village of Rumdong, a few hours by foot from Agok, the local leader, James Kuol War, recalls how a man died this year after being bitten by a snake because he did not reach hospital in time. Two other people in the same village, including a 13-year-old girl, have been treated for snakebite at MSF’s hospital in the past year.
Sixty-year-old Nyandeng Goch from Wungden was bitten on the foot by a Puff Adder snake during the night. She didn’t kill the snake, because, according to tradition, the villagers believe their ancestors live within the snakes. Instead, with the help of her neighbors, she followed a traditional healing method to stop the venom from spreading and dug a hole in the soil and waited. Not feeling any better, she decided to walk to the MSF hospital in Agok—which is about four hours away by foot—where she received treatment for the snakebite.
Globally, some five million people are bitten by venomous snakes every year, and around 100,000 die. Thirty thousand of those deaths happen in Africa. In fact, the true numbers could be even higher, as many deaths are likely not reported. “Some people come too late and some don’t come at all, so we don’t actually know the full extent of the snakebite burden in the area,” explains Jacob Chol Atem, an MSF clinical officer in South Sudan. “But we do know it is a big problem and that people lose their lives because they can’t get treatment.”
Antidotes priced out of reach
Snakebite envenoming—the medical condition resulting from a snakebite—needs to be treated with antivenom in most cases. But antivenom is expensive and unavailable in many health facilities. Treatment can cost several hundred US dollars per patient—more than a year’s salary for many people, especially those in rural areas where most snakebite victims live. Additionally, governments don’t provide much support for this disease since it predominantly affects those who aren’t in a position to demand attention.
Snakebite is a poor person’s disease, and pharmaceutical companies don’t create medicines for the poor; they create products that will be lucrative. Previously, MSF used FAV-Afrique, an all-in-one antivenom, to treat envenoming from ten different snake species in sub-Saharan Africa. But the manufacturer stopped producing it because of a lack of profitability and the last batch expired in June 2016.
With no equivalent available, MSF had to find suitable alternative treatments. Two years down the line, MSF medical teams are now successfully using two new antivenoms in South Sudan: EchitabPlus and SAIMR-Polyvalent. “Before it was more straightforward: we could give the same antivenom even if we didn’t know which snake the patient had been bitten by,” says Atem. “Now, the treatment has become more complex and we administer antivenom depending on the patient’s symptoms. But overall, it works, and we are glad to have found an alternative.”
While this is good news for MSF patients in Agok, this approach is not the solution for all snakebite victims, as determining which of the two antivenoms to use based on symptoms is difficult for non-specialists. High prices keep antivenoms that are effective against venomous snakes in any given area out of reach of the people who need them most. It is a vicious circle in which countries don’t buy antivenoms for their hospitals because they are too expensive and pharmaceutical companies don’t produce them because so few buyers are purchasing them.
Antivenom is not always enough
Even with antivenom, treatment for snakebite is much more difficult when victims arrive late to hospitals. Delays can cause further damage, including “compartment syndrome,” which occurs when swelling caused by the venom increases pressure within a muscle compartment, to the point that blood cannot supply the muscles and nerves with oxygen and nutrients.
If left untreated, compartment syndrome can cause muscles and nerves to fail and eventually die. Once acute compartment syndrome has occurred, surgery is the only option. In the most severe cases, the damage may be so extensive that patients lose the use of their limbs or need amputations. An estimated 400,000 people globally are maimed or disabled every year as a result of snakebite.
The long road to recovery
Awien has been at the hospital for two months now. She was in critical condition when she arrived and was treated with three doses of antivenom. She was unconscious for the first five days, but eventually she came to and her condition began to improve.
She has since had multiple surgeries to remove dead tissue, as the muscles in her arm were damaged beyond repair as a result of compartment syndrome. Nineteen surgical procedures is an awful lot, but her family did not want her arm amputated and asked the medical team to do all they could to save it. Though the road to recovery has been long and difficult, Awien is lucky. For countless others, treatment for snakebite remains out of reach.