An interview with MSF doctor Hermann Reuter
MSF doctor Hermann Reuter works in a tuberculosis (TB) project in a rural district of Swaziland called Shiselweni.
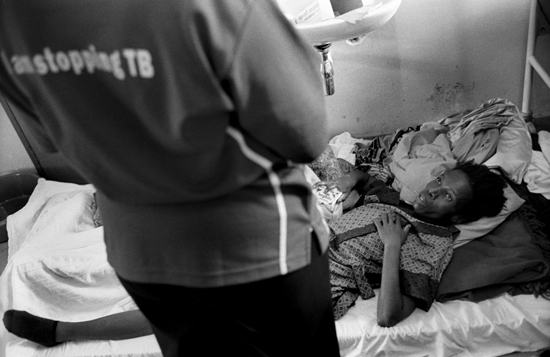
Swaziland 2007 © Alexander Glyadyelov
MSF medical staff examines a patient at an HIV- TB treatment center in Shiselweni region.
Doctors Without Borders/Médecins Sans Frontières (MSF) doctor Hermann Reuter works in a tuberculosis (TB) project in a rural district of Swaziland called Shiselweni. MSF is present in 17 clinics and three health centers here and Dr. Reuter rotates between the health centers, where most of TB patients are managed. Here, he explains the situation on the ground.
What do you see at the health centers?
On a daily basis, nurses manage the TB patients and refer the most severely ill to me. The cases I see are usually infected with multi-drug resistant TB, which means they would have already been treated with standard TB drugs without success. Other patients I treat have HIV/AIDS-related complications.
What are the main obstacles facing people with TB or HIV/AIDS here?
As Shiselweni is a rural district, distance is always a huge problem. Patients live on farms away from towns, many of them have to travel for hours to get to a health facility and they can spend their whole monthly earning on just one trip. This is unsustainable for them.
A patient needs multiple visits just to be diagnosed, and then they undertake a treatment regimen of 6 to 8 months for drug-sensitive TB or up to two years treatment for drug-resistant TB. MSF's strategy, which is to provide decentralized care, is not rocket science. It is based on what many other countries do to manage TB and HIV. We focus on providing treatment and follow-up in local health clinics, as close as possible to the patient's home.
In addition to the challenge of treating patients in a rural community, there is also a significant shortage of doctors. At the moment in this country the HIV/AIDS protocol demands that a doctor initiates patients on antiretroviral (ARV) treatment. MSF believes that the initiation of treatment could easily be managed by an appropriately trained nurse.
We need to work with the authorities to try and adopt a protocol that allows nurses to start ART for HIV positive patients.
How have HIV/AIDS and TB combined into what is being called a dual epidemic here?
About 83 percent of TB patients in Swaziland are co-infected with HIV. The country has the highest level of HIV infection in the world, affecting one out of four adults. This complicates the clinical picture of TB—diagnosis becomes more difficult and there are more severe side effects to the drugs.
Why is MSF calling for an emergency response to this crisis?
In most of the conflicts or natural disasters where MSF intervenes around the world, the number of people dying is significantly less than what we are seeing today in Swaziland.
One out of four sexually active adults has HIV/AIDS and life expectancy has fallen to 32 years of age. Currently, 18 percent of people infected with TB will die in this country. This is an extremely high figure.
Most of the patients die in the first two months, because they are also infected with HIV and were not put on ARV treatment fast enough or because they are infected with drug-resistant TB and were not diagnosed early enough.




