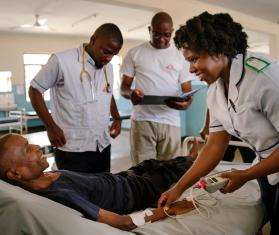
For over 20 years, Doctors Without Borders/Médecins Sans Frontières (MSF) has been providing people with HIV/AIDS in Arua, Uganda with treatment free-of-charge. MSF and Arua’s District Health Services have worked together to care for the most vulnerable people living with HIV/AIDS and to introduce various innovations in disease management, such as antiretroviral (ARV) care, specific care for children and adolescents, peer support groups, and point-of-care laboratory analysis. MSF can now hand over the program to Ugandan health authorities and partners, thanks to improved living conditions for people with HIV.
In 1999, MSF started supporting local health authorities and the hospital management team of Arua Regional Referral Hospital in northwestern Uganda to prevent mother-to-child HIV transmission. Three years later, MSF established one of the first ARV therapy programs in the country, initiating ARV treatment for all HIV-positive patients in need in Arua District, which has a total population of some 830,000 people.

Uganda 2023 © Sophie Neiman
“In 1990, when I was diagnosed, the stigma was too great. There was no medicine for the virus, it is only death. So, you go and prepare yourself with your church people. I bought a goat. I bought a duck. I told my children, ‘They are saying there is no medicine for HIV so this goat I have bought—when I am dead, share it with the community, for the reverends who will come to bury me’.”
At the time, there was no free-of-charge treatment accessible to people with HIV, which meant medicines were unaffordable for most of the population. Coupled with widespread lack of knowledge and misconceptions about the disease, this resulted in a high level of stigma and exclusion from communities for HIV-positive people. An HIV diagnosis was often equivalent to announcing a near and certain death.
The introduction of free ARV treatment in Arua was a game-changer in patient’s lives. MSF teams were also involved in the treatment of opportunistic infections such as cryptococcal meningitis, tuberculosis (TB), and multi-drug resistant TB.

Uganda 2023 © Sophie Neiman
“At that time, the Ministry of Health did not have ARVs. MSF was the only organization actually providing everything—even the normal drugs for other diseases. The Ministry had very few. Sometimes you get shortages here and there, but MSF was actually filling the shortages.”
To complement the medical assistance provided through diagnosis, treatment, and follow-up, MSF started providing extensive psychosocial support, including peer counseling, outreach, and home visits to help patients and inform their family members about HIV and the necessity of their continuous support, which is key to survival.
Several patients were then recruited by MSF to become health educators or peer counselors in communities. They also played a role in helping other patients fight stigma and meet up to support each other and exchange information on therapeutic education.

Uganda 2023 © Sophie Neiman
“The psychosocial support MSF gave to patients is even more than the medication they gave us. Without psychological support, the medicine you are taking is useless. We used to be in HIV support groups. You’d go to a person’s home, and if the person is sick, you fetch water for them, bathe and feed them”
It was only in 2004 that free ARV treatment became available through health authorities, but with limited access and supply. At the time, only doctors were able to prescribe ARV medicines in large hospitals. The objective was to enable smaller health centers, closer to the patients’ homes, to provide treatment and management of HIV.
From 2005 to 2010, MSF promoted the decentralization of HIV care, including training and mentoring health staff in Koboko, Adjumani, Nebbi and Yumbe in collaboration with District Health Services. In 2013, MSF introduced the first point-of-care viral load blood-testing to be performed at the site of patient care, as opposed to sending samples to a central laboratory and getting results months after. Same-day results allowed for the rapid detection of treatment failure and swift medical response.
Support of critical cases and youth groups
As ARV treatment became more accessible in the country, and diagnostic and treatment facilities developed, MSF gradually transferred patients to their closest peripheral health center and focused its support on the most critical patients. This included those suffering from second-line treatment drug failure, who needed an expensive genotyping test and eventually a third-line treatment not yet available in Uganda. MSF also kept caring for children and adolescents, as well as patients with advanced HIV diseases.

Uganda 2023 © Sophie Neiman
“’Safe Haven was created for the orphans—children who were diagnosed with HIV as early as six months old. They grew with MSF in the program. As part of the different social networks among the different age groups, we thought we should have a group for children.”
Former young patients created and implemented this approach for children and adolescents—first with Safe Haven and then in collaboration with the organization Maisha—to encourage better adherence to treatment.
Teenage patients were invited on Saturdays to attend activities including football and other games, icebreakers, free food, and health education with peer counselors.

Uganda 2023 © Sophie Neiman
“That is when I started knowing that we are not alone. We have a group of people who are like us. Hope started coming in slowly. Mostly it has helped in dealing with acceptance, which is the biggest thing a person with HIV faces every day. Without acceptance, you will not see the use of medication. Without the use of medication, you will not see the use of life.”
Reaching the UNAIDS 95-95-95 goal post
More than 20 years after initial MSF support to people living with HIV in Arua, huge progress has been made in HIV medical treatment. Increased knowledge and improved clinical management, along with greater acceptance both from the patients and the community—even if some stigma remains—has enabled significant progress towards the UNAIDS 95-95-95 strategy which aims for 95 percent of the people who are living with HIV know their HIV status, of whom 95 percent are on lifesaving ARV treatment and 95 percent who are on treatment are virally suppressed.
According to the latest Uganda population-based HIV impact assessment in 2020-2021, 80.9 percent of the Ugandan population knew their HIV status, 96.1 percent of whom were on ARV therapy and 92.2 percent with suppressed viral load. At this stage, the patient's immune system is strengthened, and the risk of transmitting HIV infection is considerably reduced. More people now live with HIV in Uganda: 1,400,000 people in 2022, according to UNAIDS, while there were 530,000 in 2003. This is due to greater awareness about the disease, more testing and lower mortality from the disease. Approximately 14,000 people died from HIV/AIDS in 2022 versus 78,000 in 2003.

Innovations mainly in models of care and support brought by MSF, in collaboration with the Ministry of Health, to Arua district over the years are now part of the general national strategy for diagnosis and medical care of people living with HIV in the country.
Even while MSF ends its support to this HIV program, we remain present in the country to respond to emergencies (epidemics and internal displacement), and also in the district of Kasese, where we run a specialized center for adolescents aged 10 to 19 years old, since 2015, in collaboration with local health officials. This project enables adolescents to benefit from medical care adapted to their specific needs, particularly in terms of sexual and reproductive health, with a particular focus on pregnant adolescents, HIV treatment and care, sickle cell anemia, social support, and mental health.