More than 10,000 nurses work with Doctors Without Borders/Médecins Sans Frontières (MSF) projects worldwide, making up the majority of our force of health care professionals providing critical services to people amid crises of all kinds. In honor of National Nurses Week, we're highlighting the vital role nurses play in our projects around the world, from war zones to places struck by natural disasters and weather events caused by climate change. Here are their stories.
Central Mediterranean Sea
Niamh
Niamh Burke is an Irish nurse aboard MSF’s rescue ship, Geo Barents, in the Central Mediterranean. In May last year, she described a rescue months prior.
In near total darkness on the first evening of 2023, we approached a flimsy craft bobbing on the dangerous waves of the Central Mediterranean, many miles from the safety of shore.
From my position at the bow of one of the two MSF high-speed rescue boats, it was hard to see how many people were onboard. I wondered what condition they may be in; likely hungry, tired, and traumatized as well as soaked with sea spray in the ocean winds.

Conakry, Guinea
Aïcha
Aïcha Camara is a nurse working with MSF's HIV project in Conakry, Guinea. She shared the testimony below in September 2023.
I joined Conakry’s HIV project at its inception in 2003. At first, I would do at-home HIV testing. I had to stop traveling to patients’ homes by car because they were worried that their neighbors would discover they had potentially contracted the virus. I have personally witnessed levels of stigma fall in this country and watched knowledge about HIV grow amongst the population.

Abyei Special Administrative Area
Nur
Nur Mawein is a nurse activity manager at Ameth Bek Hospital in Abyei, a region claimed by both Sudan and South Sudan. He shared the testimony below in November 2023.
I went to Sudan with my family when I was only 4 years old. It was 1986 and the civil war was terrible at that time, we were refugees. I was born in Abyei, near the oil fields in the north.
MSF really helps people by engaging with the communities. Having the hospital means a lot to the community. People feel safe there. But simply having a hospital is not enough—it is having a hospital that runs well and serves everyone.

Gaza, Palestine
Mohammad
Mohammad shared the testimony below on October 31, 2023, when he was working at Al-Shifa Hospital in Gaza City, Palestine, which has since been destroyed.
The situation inside Al-Shifa is unbelievable. Every day, every hour, every moment—we receive casualties. Hundreds of casualties every day.
When people first come to the hospital, we receive them in the triage room. We try to stop the bleeding, cover the wounds, and keep them alive. Most of the patients are children and women. The types of wounds are unbelievable: shrapnel wounds on their faces, all over their bodies; bones exposed; internal bleeding after being under the rubble for hours; deep burns—40 to 70 percent of the body. Most of the wounds are infected. It's terrifying to express.

Kunduz, Afghanistan
Diana
Diana Pereira de Sousa is a nurse who worked at the MSF hospital in Kunduz, Afghanistan. She shared the reflections below in January 2023.
‘Can you come to the ER? It’s urgent.’ The call was from Boyd, one of our doctors. When I got there I saw some of our senior medics talking fast. Five burns patients had been rushed to the ER.
In the red zone [where patients in critical condition are treated] there was a woman and four young children, all with second and third-degree burns. The complexity and severity of the burns required a higher level of care than we could offer.

Massakory, Chad
Soldongar
Soldongar Ngaro is a nurse specializing in treating malnourished children in Massakory, Chad. He gave the below testimony in August 2023.
The day before yesterday, I had a very difficult shift in intensive care.
My shift started at 4:30 p.m. Our intensive care unit has five beds, and this is where we take care of the most seriously ill children. At the start of the shift, it was clear that there were three children on the unit who were particularly ill, including one baby only a few months old.

Port-au-Prince, Haiti
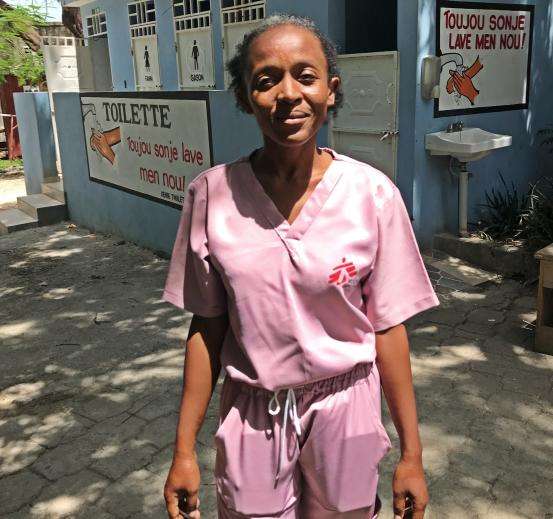
Claudia
Claudia is an MSF nurse in Port-au-Prince, Haiti. She gave the below testimony in June 2023. The violence has since escalated.
Every day is unpredictable; this morning, for example, I arrived and everything went relatively smoothly. There were no problems on the road, it was just routine. Why did I say routine? Every time there's a bus on the Martissant road, we have to stop to give money to an armed group, and then they let us go. We shouldn't have to adapt to this kind of life, but unfortunately, we're in Haiti, trying to survive.
I arrived at the emergency center at 7:45 a.m. and, as a nurse supervisor, I had to organize the day. Like all week, there were a lot of children in the waiting room, because we're overwhelmed with pediatric cases.