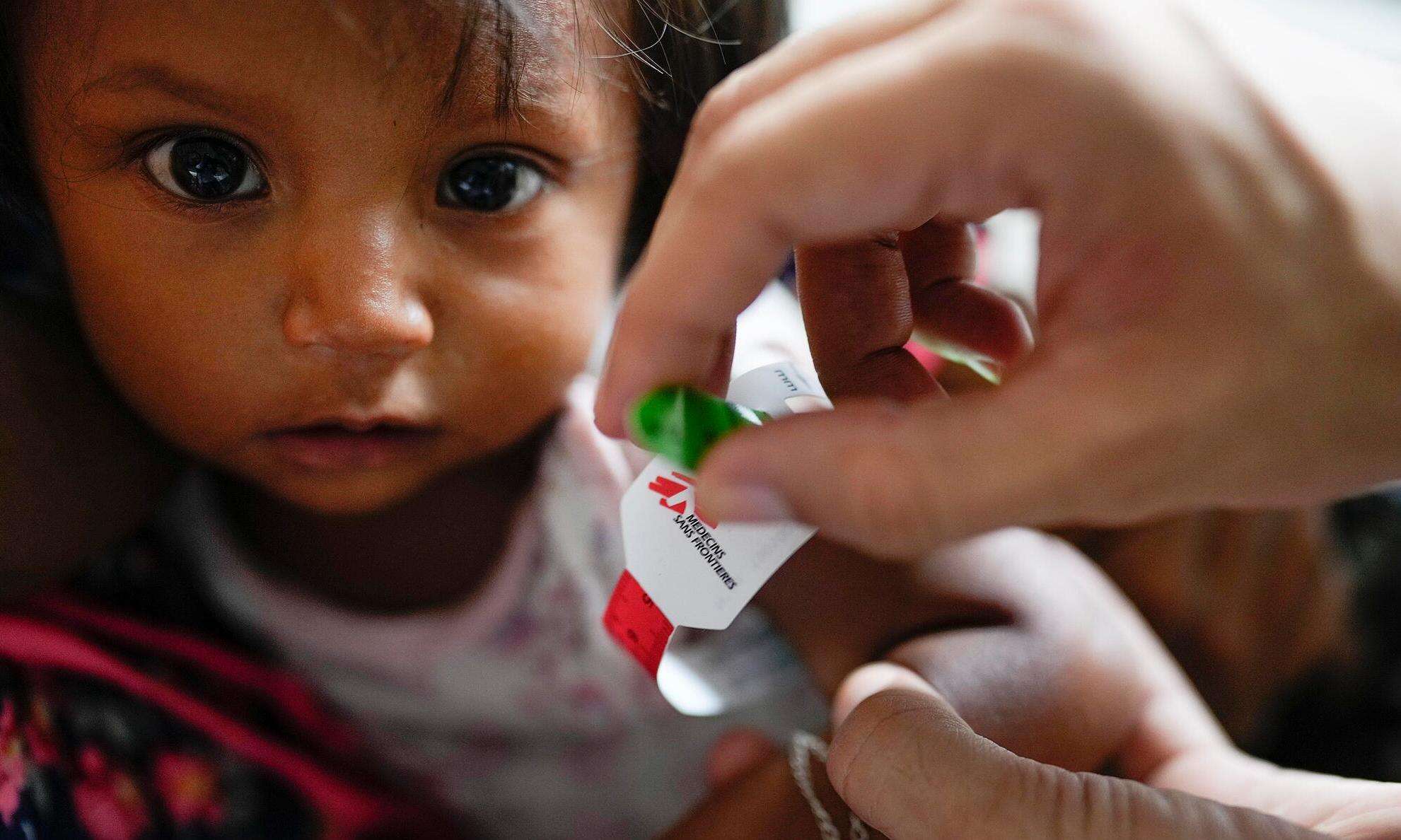
This year marks the halfway point toward reaching the UN’s Sustainable Development Goals (SDGs), which it aims to achieve by 2030. Universal health coverage (UHC) is an important component of the third SDG: Ensure healthy lives and promote well-being for all at all ages. UHC is defined as “all people have access to the full range of quality health services they need, when and where they need them, without financial hardship.”
Today, Doctors Without Borders/Médecins Sans Frontières (MSF) released a report highlighting the lack of access to health care among the world’s most vulnerable people, and how the current agenda set by the UN neglects this issue. Here, MSF’s senior advisor on health policies, Dr. Mit Philips, explains what needs to be done to ensure universal health coverage for those who need it most.
UN member states have committed to achieving universal health care coverage by 2030. How do you measure progress toward that goal?
Access to essential care today varies widely depending on where a person lives, who this person is, and what their health need is. A citizen in a well-equipped city has a completely different experience than someone from a vulnerable background when they need lifesaving surgery, prenatal care, a reliable supply of medicine for HIV or malaria; or when they need to pay for drugs for diabetes. In that sense, health coverage today is nowhere near universal. MSF teams witness every day what human tragedies are caused by a lack of access to health care.
People who face the largest barriers in accessing care include those who cannot afford to pay for essential care, people facing a crisis situation, and people excluded or discriminated against because they’re migrants, refugees, or socially marginalized.
Little attention is paid to the most vulnerable in the current UHC agenda and country plans. The focus is on long-term plans and system change, but the crucial link to the direct response to patients’ health needs is missing. Vulnerable people cannot afford to wait for theoretical plans to bear fruit.
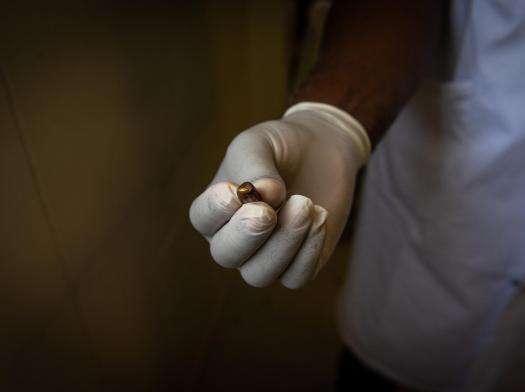
Haiti 2022 © Johnson Sabin/MSF
“I didn’t come to the hospital because there was fighting in the neighborhood. The gangs didn’t allow anyone to pass. I contacted a nurse to have my wounds treated, but it was expensive, 1,250 gourdes [about $9], and I didn’t have money.”
Universal health coverage means that people should not suffer financial hardship to access health care. Has there been improvement in that regard?
There are more people today at risk of falling into poverty because they have to pay for health services than in 2000. Poor and vulnerable households are more at risk of the so-called “catastrophic health expenditure.” In order to access health care, they have to sell goods, borrow money, or reduce other important expenses for their family, such as food or education. This does not even account for the people who are forced to forgo care because they simply cannot afford it. Too many people have to choose between illness or even death versus their family’s economic survival.
MSF has already pointed to the increased burden of user fees. Today patients are forced to pay fees before they can get care, exemptions from payments are strongly limited, and in the UHC agenda there is still no concrete action proposed to make sure that those who need it the most can access health care free of charge.
Most UHC plans rely heavily on domestic resource mobilization. But countries with the weakest health systems also tend to have the smallest tax bases. In most contexts where MSF works, public budgets for health have been undermined and have suffered from austerity measures since the COVID-19 pandemic and the global economic crisis. Patients already face gaps in essential medical supplies and services. At the same time, there has been a reduction of international funding for health, with large cuts in countries like South Sudan, Sierra Leone, and others.
This undermines strategies to ensure essential care free of charge. How can countries with huge staff shortages and stockouts of essential medicines hope to provide universal health coverage to their population? To compensate for the losses in health care coverage and the increased precariousness of populations, UHC plans need to urgently address financial access barriers. User fees should be abolished for essential care.

Afghanistan 2023 © Nava Jamshidi
“We went to a public hospital and then to four private clinics, but my child was still sick. One of the private doctors gave us a prescription for 1,000 AFG [about $13]. The public clinic did not give us all the medication we needed. I live with seven people, it’s not easy to pay for what we need. It was difficult to pay for transport to the city, that’s why we went to private clinics. Now my child is worse, and we owe a lot of money.”
As in all SDGs, the underlying promise is to “leave no one behind.” Is this happening?
Most UHC plans not only neglect the needs and vulnerabilities of migrants, asylum seekers, non-residents, and marginalized people; they often deliberately exclude them from social protection schemes. In some provinces in South Africa, migrant women and children are required to pay out-of-pocket for essential services if paperwork cannot be shown immediately. In Belgium, asylum seekers are excluded from timely lifesaving hepatitis C treatment. Most European countries fail to provide preventive care such as vaccination and now epidemic outbreaks of vaccine-preventable illnesses are spreading among asylum seekers
Secondly, the aspiring narrative of UHC is not translated and adapted to respond effectively to the needs of people affected by emergency situations. For example, even when increased funding is provided by international donors, the requirement to suspend user fees or to take measures to reduce other out-of-pocket expenses is missing. It’s difficult to mobilize additional frontline workers and support them adequately.

South Sudan 2023 Paul Odongo/MSF
“We walked for five hours by foot to reach the closest place that offers hospital care. My nephew and I were alternatively carrying the child while walking to Lankien. The people here only take their children to the hospital when they are extremely sick. The hospital is far away, so many of them cannot even reach the hospital.”
Bureaucratic hurdles block the rapid supply of medical items. We recommend that each UHC country plan includes a specific chapter on what adaptations and extra interventions will be applied during crisis or emergency situations to ensure effective access to care.