Women’s health needs do not disappear during times of war or conflict—they become more critical.
In conflict settings around the world, women often struggle to obtain adequate food, safe drinking water, and basic sanitation while losing access to contraception, maternal care, and protection from sexually transmitted infections as the risk of sexual and intimate partner violence grows. As a result, women face a heightened likelihood of becoming sick or dying. That’s why any humanitarian response must prioritize dedicated, comprehensive health services and protection for women.
In contexts of conflict and war where Doctors Without Borders/Médecins Sans Frontières (MSF) teams work, the contributions of women in affected communities make it possible to establish and expand vital health services. Working as midwives, community health volunteers, intercultural mediators, and other roles, they share their skills, lived experiences, and local knowledge to help expand women’s access to medical care and social support, and avoid suffering in silence. Women are pivotal to our response.
Khadija Yahia Adam* is an experienced midwife and one of nearly 600,000 Sudanese refugees trying to survive in Chad. Most of the refugee women in eastern Chad prefer delivering at home, assisted by midwives in the community. However, in camps, midwives usually lack the necessary tools and hygienic conditions to do their work, which exacerbates the risks for the mothers and their babies. MSF trained Khadija as a volunteer to support much-needed prenatal and postnatal care and conduct referrals for safe delivery care at the MSF-run maternity facility.
Khadija
“I want to keep mothers and babies safe.”
“People come to me because they know I worked with [health] centers before. They come to me very often, asking for the care that used to be available for Sudanese. I tell them, ‘No problem’ and examine them. Whether old or young, I send them to the hospital so they can have a safe birth. This is the important thing.
I was settled with my kids and working, but then the war happened. Some people left and we do not know if they are dead or alive. No one from my [extended] family is with me. I am with my old neighbors. My kids' father left us a long time ago. I am the sole caretaker of my kids [and] for eight years I have been working and providing for them."

Our work in Adré
MSF opened a health care clinic in Adré in July 2023 that has since grown to provide prenatal care, postnatal care, and care for survivors of sexual violence, as well as a referral pathway for safe delivery care in maternity facilities. The MSF team also sought out experienced midwives from within the displaced community like Khadija, who are unable to join the formal health care workforce but are frequently consulted by pregnant women. The midwives receive training in prenatal and postnatal care, refer patients to MSF facilities in Adré, and encourage women to seek medical care and avoid the risk of staying at home.
Noura Arafat is an MSF intercultural mediator who has lived in Nablus in Palestine’s West Bank all her life. Since the current war in Gaza began in October, the situation across the occupied West Bank, including in Nablus, has continued to worsen as movement restrictions and violence by settlers and Israeli forces have increased. Noura helps women from her community cope and find hope in life through MSF’s mental health program.
As an intercultural mediator, Noura facilitates psychotherapy sessions between patients and MSF psychologists and briefs international psychologists about the situation in Palestine and its culture and history, along with unique insights into the community.
Noura
“These women know their strengths"
“We don’t feel safe, especially recently with the high number of checkpoints all around the city. We try to be inside the city as much as we can. Women in Palestine have all kinds of challenges, [such as] grief. Almost every day we lose a Palestinian. So we work with mothers every day. They grieve the loss of their sons, their husbands, their children, which is really sad. And sometimes it's a lifelong grief which has no solution.
[People] think it's just a conflict. To me, it's not. We are people who suffer every day since we were born. When you see people suffering psychologically with different disorders, obsessive compulsive disorder, for example, you think it's simple. But when you delve more into the history of the patient, it's because a father has been imprisoned for life or because the patient has never seen her father, for example. Every single aspect of our lives is affected by the occupation [in ways] you can never imagine."

Our work in the West Bank
MSF has been working in Palestine since 1989. Today, MSF teams are providing primary health care, mental health support, and training for medical staff and volunteers in Nablus, Hebron, Jenin, and Tulkarem, in addition to ongoing operations in Gaza.
The number of tents is growing in Kanyaruchinya and other displacement camps in eastern Democratic Republic of Congo (DRC), as another outbreak of violence in North Kivu has forced people to seek safety that is far from assured.
The conditions in the camps are dire. Tents are made of thin plastic sheeting and held down at the edges by the volcanic rock native to Goma. Basic needs such as food, water, and sanitation are unmet, and there is a critical lack of measures to protect people from further harm. The lack of security and means to survive has proven particularly dangerous for women, as evidenced by the high number of cases of sexual violence seen at Kanyaruchinya Health Center.
The actions of community members demonstrate their resilience in the face of conflict and displacement. Often, they, too, have survived direct violence, are grieving the loss of family members, and are the heads of households with children to care for and protect. For many, the future is filled with uncertainty.
Among the many people displaced due to surging conflict in eastern DRC, community health care volunteers like Henriette Mbitse are helping to increase safe and confidential access to care for survivors of sexual violence through MSF’s program in Kanyaruchinya camp. Maman Henriette, as she’s affectionately called, was a health volunteer in her home village before fleeing from Kibumba with her family. Now the mother of nine lives on the grounds of Mboga Primary School with others who survived the harrowing journey.
Henriette
“I am a displaced person … I’m also a health volunteer.”
“I began sensitizing women here in Kanyaruchinya about access to health care and about sexual violence, with MSF. [Sometimes] when women go into the forest to look for firewood, they are raped. When you don’t have soap or clothing ... you go into the forest to look for wood or vegetables that you can sell. This is a serious problem for a displaced person.
Our living conditions are difficult. Sometimes, some men wake up in the middle of the night, rip the plastic sheeting [of tents] with a razor and break through to rape women who are living alone. That’s [also] the problem we have.”

Clara* fled from Rutshuru territory, DRC, with eight children in her care. She was raped when she went to collect wood in the forest to sell as firewood. Although she had heard health promoters and community health volunteers’ messages about seeking care and what was available, she was paralyzed with distress until meeting a community health volunteer who took her to the health center.
Clara*
"She listened to me"
“Because of the lack of food, I decided to go into the forest to look for firewood. When I arrived there, I came across three bandits, Two of them asked me to choose either to be killed or raped. One of them ran away. When the two people finished their dirty work, they left. Then I left too, crying.
After that incident, I was staying in bed, crying, pitying my kids and those orphans who have no one to help them.
About three days later I met a community health volunteer. I recognized her by her outfit, stopped her, and told her I had a question. As she listened to me, I told her that I met bandits that raped me and that I was feeling bad. I asked her to lead me to the health center."
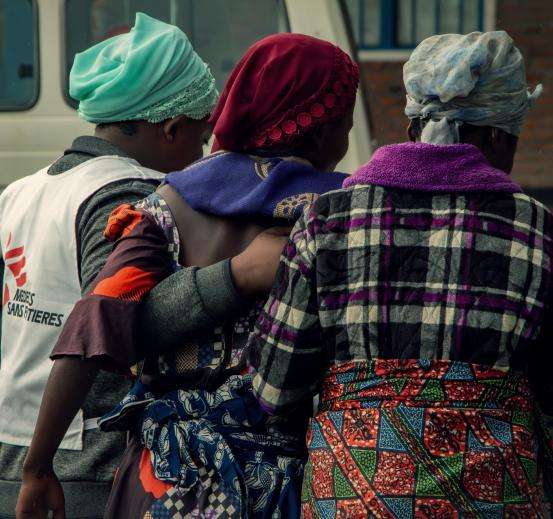
Délice Sezage Tulinabo is a health promoter in DRC who gives community talks, runs focus groups, and supervises health volunteers like Henriette. She is encouraged by the growing awareness of sexual violence and the importance of seeking care as quickly as possible. More women are seeking care within 72 hours of being assaulted, which is crucial for them to receive emergency care to prevent unwanted pregnancies and sexually transmitted diseases, especially HIV.
Délice
"I have learned many things from the women we assist."
“Before MSF started working here, we had many cases of post-rape pregnancies, for example. Now that MSF is here, there are us health promoters as well as community health volunteers... Now people come.
The services consist of medical care and psychological care. Therapists and psychologists offer follow-up, and we also guide women according to their needs to other services."

Our work in Kanyaruchinya camp
In addition to providing medical and psychological care for survivors of sexual violence, MSF teams offer women various methods of contraception, treatment for sexually transmitted diseases, and safe abortion care. MSF also supports the obstetric and neonatal care departments at Kanyaruchinya Health Center, where around ten women give birth every day, as well as primary health care and referrals of complicated cases to a hospital in Goma. Across DRC, MSF provides treatment for and vaccination against outbreaks of cholera and measles, water and sanitation infrastructure and services, health promotion, and nutrition care.
*Name has been changed




