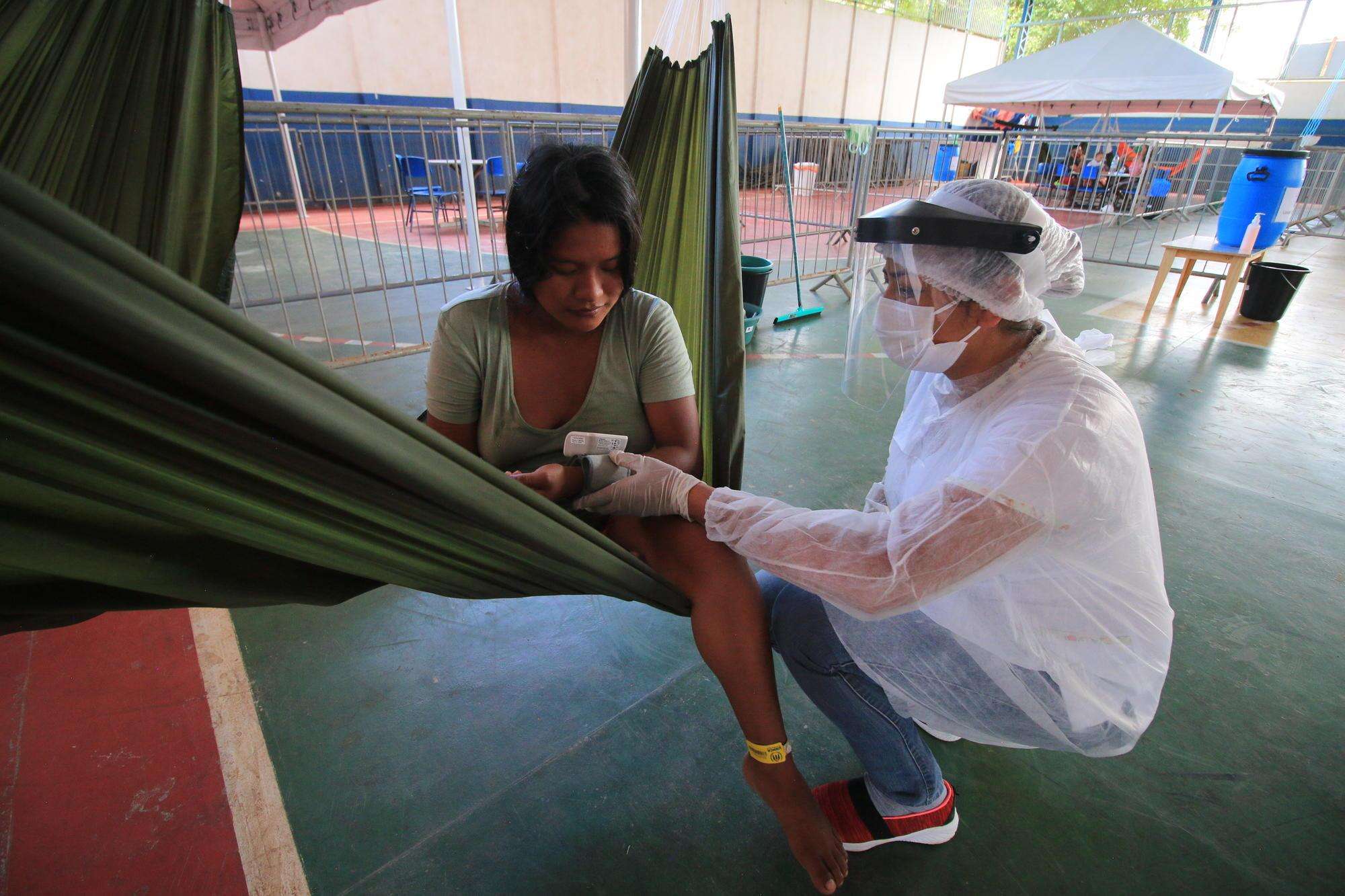
Every day between 15,000 and 30,000 people in Brazil are diagnosed with COVID-19 and hundreds of people die. The country has the second highest number of cases and deaths in the world—with more than 900,000 cases and 45,000 deaths recorded by the World Health Organization. Nurses are dying of COVID-19 at a higher rate than any other country: almost 100 nurses in Brazil die from the disease per month.
The outbreak has spread across the country from large cities, such as Rio and São Paulo, to remote areas, such as Amazonas state, threatening the most vulnerable and neglected communities, including those living in slums and favelas, homeless people, and indigenous and riverside communities.
MSF has launched six COVID-19 emergency responses in Amazonas and Roraima states—both in the greater Amazonia region—in Rio de Janeiro, and in São Paulo, but we are reaching our capacity. A more focused COVID-19 response is required from the central government, which must provide greater support to community leaders, local organizations, and staff on the front line of the epidemic. Local groups and health workers need direct assistance and essential tools—whether that support comes from inside Brazil or from other countries.
“It is not a coincidence that Brazil is suffering so acutely,” said Ana de Lemos, executive director of MSF Brazil. “We have long known that Brazil is a country with enormous inequalities, but COVID-19 is exposing a health system plagued with structural inequalities and exclusion from care for huge numbers of poor or homeless people, and for regions such as Amazonia that have been starved of proper health investment for decades. We have seen amazing efforts deployed at the state or local level to deal with the pandemic, but we also see a huge misalignment in guidelines, policies, and the general approach between the central government and the regions.”
Brazil’s capacity to respond to the COVID-19 outbreak is being stretched beyond its limit. Testing is not being rolled out fast enough. Brazil has reported 7,500 tests per million people—almost ten times less than the United States (which reported 74,927 per million). A stronger COVID-19 response from the central government is needed to prevent this outbreak from getting even worse.
Helping communities in Amazonia
Amazonas state has the highest mortality rate from COVID-19 in Brazil. Brazil’s Amazon region is vast and sparsely populated by indigenous communities. The area has suffered from mining, deforestation, and farming for years. There is chronic underinvestment in health care. When COVID-19 spread to the region from the larger cities, the health care system simply could not cope.
In Manaus, the state capital, the situation in the hospitals has been devastating. “COVID-19 moves fast, and sometimes unpredictably,” said Brice de le Vingne, MSF coordinator of COVID-19 response programs. “We shifted our attention from the coastal cities to the big Amazon city of Manaus when reports of high case numbers and mass graves started emerging. By then, the situation was already at disaster levels, and with a small team we had to rapidly identify where we could best assist.”
At the beginning of the outbreak, hospitals In Manaus were overwhelmed. There were not enough intensive care unit (ICU) beds or staff to treat the high number of people with very severe symptoms who need intensive oxygen treatment. For several weeks hundreds of people waited in hospital wards for an ICU bed to become available while their conditions deteriorated.
“The four main hospitals in Manaus were all full and the hard-working medical teams were dealing with extremely sick patients, [who] often arrived too late to be saved,” said Dr. Bart Janssens, MSF’s emergency coordinator. “A high percentage of the patients [admitted] into the ICU died, and [many] medics fell sick.”
To help ease the pressure on the hospitals, MSF team opened a 48-bed COVID-19 treatment unit with an ICU and a ward for patients with severe symptoms in the 28 de Agosto hospital to supplement their existing COVID-19 treatment capacity. MSF brought in specialist ICU staff—some with prior experience treating COVID-19 in other countries—and implemented new protocols for non-invasive oxygen treatment, providing a safer space for improved clinical care. Since the medical activities started on May 28, MSF’s wards have been at 80 percent capacity or higher. Although it is still too early to draw conclusions there are signs that an increasing number of patients will be cured, even those with very severe symptoms.
Manaus is a busy city of more than two million people, which makes physical distancing difficult. The markets have lots of traders coming from outside of town, making them potential hotspots for transmission of the virus. Manaus has a population of about 30,000 indigenous community members representing 30 different ethnicities and speaking 20 languages. They are often neglected by the health care system and were neglected in most COVID-19 response plans.
An MSF health education team is working with local organizations and community leaders to provide these communities with advice on how to protect themselves from COVID-19 and conduct active screening for potential COVID-19 patients.
In partnership with the municipality, MSF also runs a residential medical center for patients from the Warao indigenous community showing mild symptoms of COVID-19. Warao people have lived in shelters in Manaus for several years, after migrating to Brazil from Venezuela looking for economic opportunities.
There are signs that the peak of transmission may have passed in Manaus, but the situation remains critical. There is a huge need for psychosocial support for medical staff who were struggling to cope during the peak of the outbreak.
Outbreak peak moving to rural areas
The peak of the outbreak has moved on further into rural Amazonia, where the numbers of cases are on the rise. Indigenous communities are extremely vulnerable to this disease and have minimal access to standard prevention tools such as personal protective equipment and very few health care options. They often have to travel long distances to regional hospitals or clinics, which carries the additional the risk of transmitting the virus on crowded public transport.
It takes one-and-a-half days by boat to reach Tefe from Manaus. Tefe is a thriving port town on the banks of the Amazon river. When MSF’s team arrived, they were shocked by the situation. “When I visited to assess the situation, the hospital management team were telling me that almost 100 percent of their COVID-19 patients needing critical care had died,” said Dr. Janssens. “They did not have enough specialist staff to care for the very sick patients that were arriving at their door.”
While MSF plans how to efficiently and responsibly engage with remote communities in rural Amazonia we have launched an initial emergency response to provide moderate and intensive care in Tefe and São Gabriel da Cachoeira. The hospital in Tefe has requested MSF’s assistance. MSF plans run the ICU—where a high number of COVID-19 patients are dying—and provide medical care in six peripheral health centers. This will hopefully reduce the need for indigenous communities to make the long journey to Manaus to seek treatment.
In São Gabriel da Cachoeira, a city that lies further north on the Amazon river, MSF will open a treatment center to supplement the hospital’s COVID-19 capacity and partner with a local organization to spread health education messages to the community.
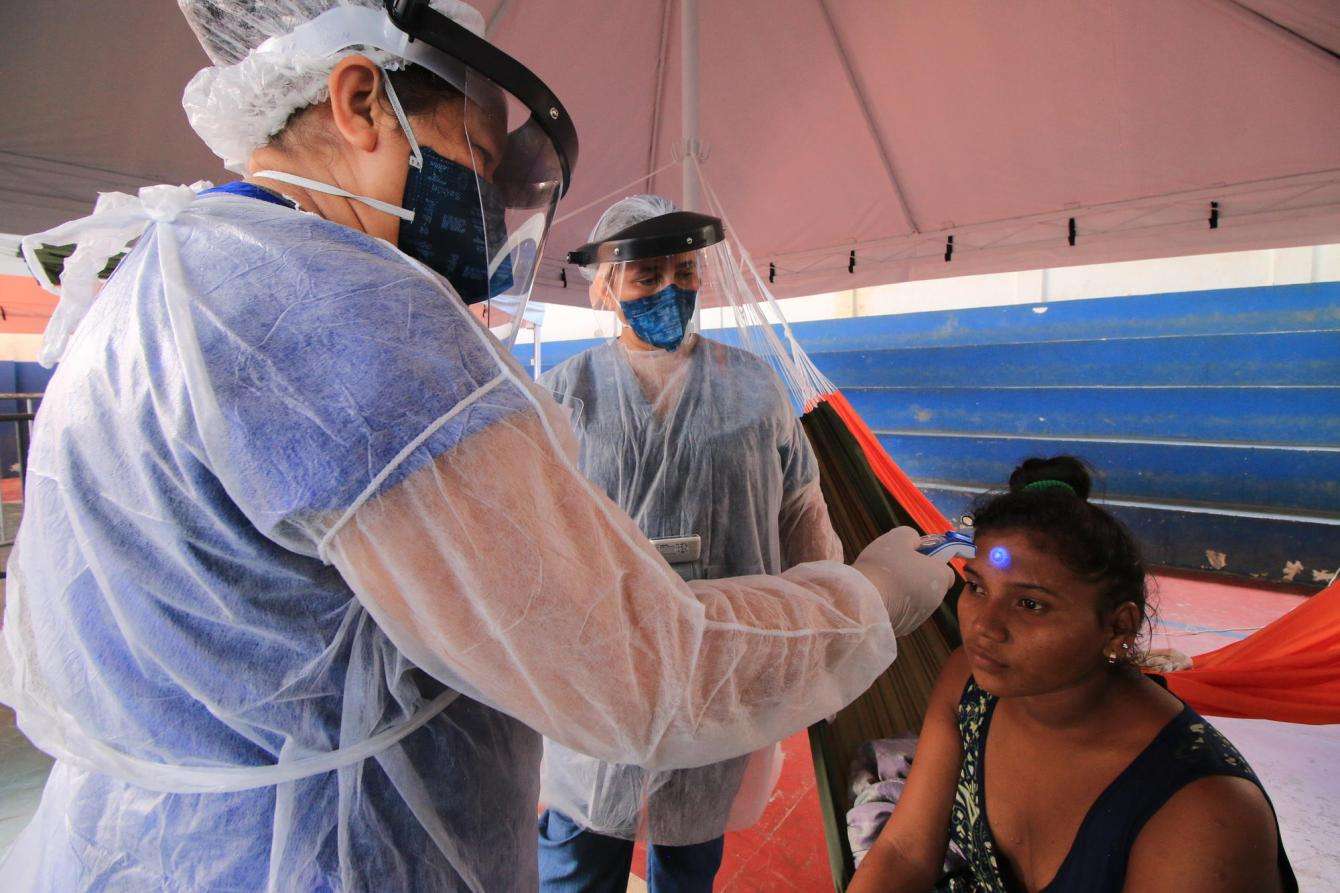
The highest new infection rate in the country
Boa Vista, the capital of Roraima state, currently has the highest new infection rate in the country—more than a quarter of the residents have been infected with the disease.
MSF has expanded its project for Venezuelan migrants and refugees in Roraima to include COVID-19 preparations and health promotion. The public hospital is entirely overwhelmed—patients are being treated in corridors or sent away with no treatment as the hospital is full. A new 700-bed field hospital has been set up to respond to the outbreak. MSF is supporting the hospital with training in the ICU and supervision.
“Right now, we are facing an acute phase in the COVID-19 crises in Boa Vista,” said Michael Parker, MSF field coordinator for the Roraima project. “MSF has responded by increasing our medical work beyond support to refugees—providing doctors and nurses for a field hospital and taking charge of training and supervision for severe cases at this very critical moment.”
Rio de Janeiro and São Paulo’s neglected communities
COVID-19 reportedly arrived in Brazil via wealthier communities who had travelled abroad and returned to major cities, such as Rio de Janeiro and São Paulo. For several weeks, the spread was contained to wealthier areas. But transmission gradually spread to poorer neighborhoods and had devastating impacts. Homeless people, drug users, the elderly in nursing homes, and people living in favelas and informal residential areas already faced barriers to accessing health care. COVID-19 has made the situation even more dire, putting these communities at risk of dying with little possibility of assistance.
“Like in many countries, the pandemic has resulted in many people losing their jobs,” said Dr. Ana Leticia Nery, MSF project coordinator in São Paulo. “But in São Paulo there were already 24,000 homeless people. With the health system stretched to its limits, the barriers preventing these extremely vulnerable population from accessing health care in Brazil have become even [worse]. The pandemic has thrown more people into extreme poverty, leaving them homeless. Drug use, addiction, and underlying medical concerns such as tuberculosis, heart disease, and HIV add to their vulnerability. Seeing people who are suffering and have difficulties accessing the normal health system is heartbreaking, but there are things we can do to help give these people access to the same treatment any other citizen would have.”
In São Paulo, MSF teams are assisting homeless people in the streets of downtown neighborhoods as well as people living in slums in the outskirts of the city where the disparity between wealth and poverty is striking. In partnership with local organizations and the São Paulo municipality, MSF runs medical activities in two isolation facilities for homeless people who have tested positive for COVID-19 and show mild or moderate symptoms. MSF is also running a health education and assistance program for people dependent on alcohol and drugs.
In Rio de Janeiro, teams have trained health centers and hospitals in infection prevention and control, and have provided health education at the municipality’s restaurants. We are actively monitoring for people who show COVID-19 symptoms. In Rio’s favelas, MSF found that the already stretched health capacity is reaching the breaking point—several health centers have had to close. Living conditions make physical distancing almost impossible, so the risk of the virus spreading is high.
MSF is undertaking a range of health promotion, screening, and diagnosis activities in most of its project locations and is providing technical advice on infection prevention and control (IPC) to medical facilities and nursing homes. At the same time, MSF teams are scaling up psychosocial support for medical staff who have experienced trauma associated with the high mortality rate and the painful way that many people die from the disease. A team is also looking into opening a palliative care unit in São Paulo, to provide dignified end-of-life care for critical patients who are too sick to be cured in other hospitals.
Our teams continue to look at ways to expand activities with local health authorities, but we are reaching the limits of our capacity. More concerted national efforts are necessary to bring the outbreak under control.